A Review of the Management of Nephrolithiasis
RELEASE DATE:
August 1, 2016
EXPIRATION DATE:
August 31, 2018
FACULTY:
Leena Myran, PharmD, BCPS
Clinical Assistant Professor
University of Wyoming School of Pharmacy
Laramie, Wyoming
Jaime R. Hornecker, PharmD, BCPS, CDE
Clinical Associate Professor
University of Wyoming School of Pharmacy
Laramie, Wyoming
FACULTY DISCLOSURE STATEMENTS:
Drs. Myran and Hornecker have no actual or potential conflicts of interest in relation to this activity.
Postgraduate Healthcare Education, LLC does not view the existence of relationships as an implication of bias or that the value of the material is decreased. The content of the activity was planned to be balanced, objective, and scientifically rigorous. Occasionally, authors may express opinions that represent their own viewpoint. Conclusions drawn by participants should be derived from objective analysis of scientific data.
ACCREDITATION STATEMENT:
Pharmacy
 Postgraduate Healthcare Education, LLC is accredited by the Accreditation Council for Pharmacy Education as a provider of continuing pharmacy education.
Postgraduate Healthcare Education, LLC is accredited by the Accreditation Council for Pharmacy Education as a provider of continuing pharmacy education.
UAN: 0430-0000-16-074-H01-P
Credits: 2.0 hours (0.20 ceu)
Type of Activity: Knowledge
TARGET AUDIENCE:
This accredited activity is targeted to pharmacists. Estimated time to complete this activity is 120 minutes.
Exam processing and other inquiries to:
CE Customer Service: (800) 825-4696 or cecustomerservice@jobson.com
DISCLAIMER:
Participants have an implied responsibility to use the newly acquired information to enhance patient outcomes and their own professional development. The information presented in this activity is not meant to serve as a guideline for patient management. Any procedures, medications, or other courses of diagnosis or treatment discussed or suggested in this activity should not be used by clinicians without evaluation of their patients’ conditions and possible contraindications or dangers in use, review of any applicable manufacturer’s product information, and comparison with recommendations of other authorities.
GOAL:
To educate the participant on the epidemiology, pathophysiology, and complications associated with nephrolithiasis and to discuss the nonpharmacologic and pharmacologic treatment and prevention options.
OBJECTIVES:
After completing this activity, the participant should be able to:
- Understand the epidemiology and pathophysiology of nephrolithiasis.
- Identify medications associated with drug-induced kidney stones.
- Develop a treatment approach for a patient with kidney stones.
- Recommend dietary modifications in patients with recurrent kidney stones.
ABSTRACT: Nephrolithiasis is a relatively common and potentially disabling condition for which patients seek medical care. Diet and lifestyle are important risk factors for the development of kidney stones, and when these factors are modified, they can assist with the prevention of nephrolithiasis. Treatment is dependent on multiple factors. Conservative management may be used in low-risk patients with mild symptoms and in those in whom passage of the stone is expected; more aggressive treatment, such as ureteroscopy or extracorporeal shock wave lithotripsy, may be necessary in patients with infection, uncontrollable pain, or obstructing stones. Special consideration should be given to pediatric patients and pregnant patients with nephrolithiasis.
Nephrolithiasis (formation of kidney stones) is a common condition for which patients seek medical care. Also known as urinary calculi, kidney stones affect nearly 9% of the U.S. population.1 In addition to the morbidity that nephrolithiasis causes patients, the impact on healthcare costs and utilization is significant.
Although traditionally rates of nephrolithiasis have been higher in men, prevalence appears to be on the rise in women, likely because of the increasing rate of obesity, which has long been recognized as a risk factor for nephrolithiasis. In addition to gender, multiple factors have been identified that increase the risk of nephrolithiasis, including age and ethnicity, as well as other disease states, such as hypertension and diabetes.1,2 Drugs—including triamterene, sulfonamides, indinavir, and antibiotics (ciprofloxacin, amoxicillin, nitrofurantoin)—have also been implicated as a cause of kidney stones.
PATHOPHYSIOLOGY AND DIAGNOSIS
The pathophysiology of nephrolithiasis differs according to where the stone originates.2 Most patients form calcium stones, which are usually composed of calcium oxalate or, less commonly, calcium phosphate. Primary hyperparathyroidism, which causes hypercalciuria, is a common condition associated with calcium stones; it may be present in up to 5% of patients with nephrolithiasis.3 Uric acid, struvite (magnesium ammonium phosphate), and cystine stones also may form under certain conditions, but they are much less common.2
The classic signs of nephrolithiasis include renal colic and hematuria, although the presentation may range from asymptomatic to more atypical symptoms, such as abdominal pain, nausea, and genitourinary pain. If a patient’s clinical presentation is suggestive of nephrolithiasis, further imaging may be necessary to confirm the presence of a kidney stone.
Whereas historically an abdominal plain film (or KUB, for kidney, ureters, and bladder) was used for imaging, technological advances have led to noncontrast helical CT scan as the imaging study of choice for the diagnosis of kidney stones. Ultrasonography also may be used, but because it is less sensitive than CT, further diagnostic imaging may be required to identify a stone.4
Studies show that in patients who pass a first kidney stone, the risk of recurrence gradually increases to as high as 50% to 60% at 10 years, especially in men.5 The American Urological Association recommends the analysis of the composition of a stone, when this is possible, since knowledge of the type of stone can guide treatment and prevention strategies and in some instances may point to the underlying cause, such as a genetic or metabolic abnormality.2
Nephrolithiasis is often uncomfortable for the patient, but significant complications rarely occur. In severe cases, complications such as urosepsis, acute kidney injury, or obstruction may necessitate more aggressive treatment and referral to a urologist. Pregnant women and patients with stones that measure >5 mm in diameter by imaging should also consult a urologist.6
MANAGEMENT AND TREATMENT APPROACH
Management decisions regarding the treatment of nephrolithiasis are based on several factors, including the stone’s location, composition, size, and shape and the patient’s symptoms. The most important factors in predicting spontaneous stone passage are stone size and location.7
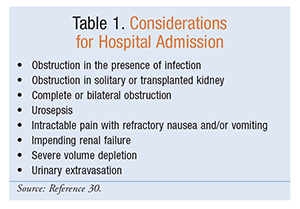
Conservative management that involves supportive care and facilitation of stone passage is preferred if passage is likely within a reasonable time frame (i.e., within 4 weeks) and the patient has acceptable symptoms and a low risk of complications.7,8 Patients may be managed at home if they can tolerate oral intake and do not have severe or suspicious symptoms that may necessitate hospitalization. Suspicious symptoms and complications that require patients to be managed in the hospital include uncontrollable pain, inability to tolerate oral medications, infectious symptoms (e.g., fever), and obstructing stones (TABLE 1).8 A urologist should be consulted when a patient is hospitalized.
Patients with kidney stones that block one or both ureters are at risk for progression to renal failure; therefore, the management of acute renal injury and complete obstruction should be considered.7 Treatment of renal colic or sepsis from an obstructed kidney requires emergency intervention, including adequate drainage with decompression and antibiotics.7,8 Drainage of the obstructed kidney may be accomplished with a ureteral stent or percutaneous nephrostomy tube. Following drainage, stone clearance is further facilitated with endoscopy or extracorporeal shock wave lithotripsy (ESWL).7 Both ESWL and ureteroscopy are safe and effective for the treatment of ureteral stones; however, ureteroscopy is associated with a higher likelihood of achieving stone-free status, particularly for distal stones. The benefits of ureteroscopy should be weighed against the increased risk of complications. Stones composed of cystine, calcium oxalate monohydrate, and brushite are more resistant to ESWL and are better treated with ureteroscopic management.8
Antibiotics
Antibiotics have a role in the perioperative setting, as well as in patients with a frank urinary tract infection due to the kidney stone.9 Perioperative antibiotics are critical to prevent surgical infections. Antibiotics are recommended for ≤24 hours in all patients undergoing endoscopic stone treatment without evidence of preexisting infection.2 Cefazolin is the first-line agent for surgical prophylaxis in patients undergoing clean urologic procedures with entry into the urinary tract, such as ESWL and ureteroscopy. Alternative antimicrobials include fluoroquinolones, the combination of an aminoglycoside plus metronidazole, or an aminoglycoside plus clindamycin.10
Obstructive pyelonephritis is a urologic emergency that can result in urosepsis and death; however, antibiotic treatment alone is not recommended for infected stones.11,12 The optimal management of infected stones includes complete stone removal in addition to antibiotic therapy.12 Definitive stone removal should be delayed until the infection is cleared following a complete course of antimicrobial therapy.7
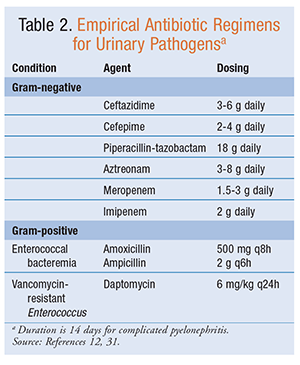
Although evidence for specific antibiotic regimens for urosepsis is lacking, empirical IV antibiotics (TABLE 2) should be initiated immediately that are directed against uropathogens such as Escherichia coli and Staphylococcus, Enterobacter, Proteus, and Klebsiella species.8,9 Ideally, urine cultures should be obtained prior to initiation of antibiotics so that the causative pathogens can be addressed once susceptibilities are available.7
Struvite stone formation is associated with bacteria that produce urease. Producers of urease include gram-positive and gram-negative species from such genera as Proteus, Klebsiella, Providencia, Pseudomonas, and Staphylococcus.All staghorn calculi should be assumed to be struvite and should be treated with prophylactic or suppressive antibiotic therapy with amoxicillin-clavulanate, cefixime, or ciprofloxacin.9
Fluids
Patients with renal colic may have a decreased oral intake owing to the associated nausea and vomiting. Fluid administration should be considered in patients with signs or symptoms of dehydration or with a risk of renal failure.13 Although hydration is the focus of treatment in patients who are at risk for progression to renal failure, universal use of IV fluid administration does not generally play a role in the acute management of kidney stones or renal colic because it is not associated with an increased stone-passage rate or a reduction in pain.8,13,14
Fluids—Targeting Urine Volume: An increase in urine volume theoretically prevents stagnant urine and promotes diuresis, whereas dilute urine alters the supersaturation of stone-forming components.15 Urine volume is primarily the target for the prevention of kidney stones, with fluid intake being the main determinant of urine output; however, a specific amount of fluid intake is not recommended for the prevention of kidney stones owing to patient-specific factors such as insensible losses and intake of fluid-containing food.7 Increased fluid intake has been shown to reduce the stone-recurrence rate by ≥50% and to prolong the interval between recurrences.16 Therefore, high fluid intake spread out throughout the day, targeting a urine volume of ≥2 to 2.5 L daily, is recommended to prevent the recurrence of most types of kidney stones.2,7,16 Cystine stone formers benefit from achieving a urine output of >3 L per day.17
No specific type of fluid is recommended to promote increased urine output for the prevention of stones. Alcohol, coffee, decaffeinated coffee, tea, and wine have been associated with a lower risk of stone formation in observational studies.2,7,16 Observational trials have also demonstrated an association between sugar-sweetened beverages (e.g., soda) and an increase in stone formation; therefore, these drinks should be avoided.2 Additionally, one randomized trial evaluated the efficacy of discontinuing soda intake in the reduction of stone formation. This trial found a reduction of 6% in stone formation over 3 years in patients who lessened their consumption of soda.2,16
Analgesia
Analgesia is the primary goal for patients who present with kidney stones that are expected to pass spontaneously (i.e., <5 mm in size). Nonsteroidal anti-inflammatory drugs (NSAIDs), opioids, and anti-spasmodic agents have been used alone and in combination in the treatment of acute renal colic.18
For renal colic, NSAIDs have better analgesic efficacy compared with opioids, as NSAIDs have been shown to have lower requirements for rescue analgesia, as well as fewer adverse effects.7,19,20 This was demonstrated in a systematic review that evaluated NSAIDs versus opioids for pain associated with acute renal colic. Patients treated with NSAIDs were significantly less likely to require rescue medication, and those receiving opioids had a higher rate of adverse effects compared with NSAIDs. There was no significant difference between NSAIDs and opioids in the proportion of patients who achieved complete pain relief. Although both NSAIDs and opioids led to clinically significant analgesia, a greater number of opioid patients required additional analgesia within an hour of study drug administration.20 NSAIDs have also been shown to be more effective than other nonopioid analgesics, including antispasmodics (e.g., tamsulosin), for pain reduction and lessened need for additional medication.21
NSAIDs: NSAIDs such as diclofenac, ketorolac, indomethacin, and ibuprofen are first-line analgesics for patients with renal colic and have no contraindications.7 NSAIDs provide analgesia through inhibition of prostaglandin synthesis, which reduces glomerular filtration and renal pelvic pressure, ureteric peristalsis, and ureteric edema.11,18 NSAIDs have been shown to reduce the number of new colic episodes and the incidence of hospital readmission.11 In addition to their effects on prostaglandin synthesis, NSAIDs prevent afferent arterial vasodilation and increase vascular permeability, leading to diuresis and increased pressure within the renal pelvis. NSAIDs also reduce edema, inflammation, and ureteral muscular hyperactivity.18
NSAIDs increase the risk of cardiovascular events or severe bleeding and should be used with caution in patients with renal dysfunction or recent gastrointestinal bleeding. They should not be administered to patients with a history of ischemic heart disease, stroke, heart failure, or recent coronary artery bypass grafting.22
Opioids: Second-line analgesics for renal colic include opioids such as morphine, hydromorphone, and tramadol.7 Opioids may be administered parenterally or orally. Common adverse effects of opioids include sedation, dizziness, nausea, vomiting, pruritus, and constipation.18,22 Respiratory depression is a severe adverse reaction that may be potentiated by concurrent use of other depressant medications (e.g., benzodiazepines), and the risk is increased in high doses.22
Tramadol exerts its analgesic effects by inhibiting norepinephrine and serotonin and binding mu-opioid receptors.22 Tramadol is as effective as morphine and has fewer potential side effects (e.g. respiratory depression, constipation).18 Common side effects include nausea, vomiting, dry mouth, dizziness, sedation, and seizures.18,22 Tramadol should be used with caution in patients with a history of a seizure disorder and in patients taking selective serotonin reuptake inhibitors.22
Medical Expulsive Therapy
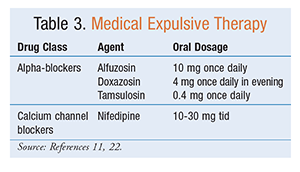
The use of medications to enhance the passage of ureteral stones is known as medical expulsive therapy (MET).8 Without MET, kidney stones <5 mm in size are associated with an 85% to 95% spontaneous-passage rate within 40 days, and stones <6 mm also have a high stone-passage rate; however, MET can reduce the associated pain and need for analgesics.7,8 MET can potentially shorten the duration and increase the likelihood of spontaneous stone passage; therefore, it should be offered to patients with distal ureteral stones measuring <10 mm.8,23 MET can also be used as an adjunct to ESWL to increase stone-fragment passage.7,8,24 Consideration should be given to offering MET to patients with distal ureteral stones measuring <10 mm to shorten the time to stone passage.8 TABLE 3 provides a summary of MET.
The utility of MET in facilitating spontaneous kidney-stone passage is controversial. A 2006 meta-analysis reported that patients treated with calcium channel blockers or alpha-blockers had a 65% (absolute risk reduction = 0.31; 95% CI, 0.25-0.38) greater likelihood of stone passage compared with those not treated with MET (pooled risk ratio 1.65; 95% CI, 1.45-1.88).23 However, this meta-analysis was limited by significant heterogeneity and poor quality of trials.
Although MET is commonly used for the treatment of nephrolithiasis, the SUSPEND (Spontaneous Urinary Stone Passage ENabled by Drugs) trial found no benefit of tamsulosin or nifedipine in reducing the time to kidney-stone passage.25 SUSPEND was a multicenter, randomized, placebo-controlled trial evaluating differences in spontaneous stone passage at 4 weeks between tamsulosin 0.4 mg, nifedipine 30 mg, and placebo. Patients were aged 18 to 65 years and had symptomatic renal colic caused by a single kidney stone of ≤10 mm located in any segment of the ureter. The SUSPEND trial concluded that overall spontaneous stone passage at 4 weeks did not differ between the groups. There was also no difference in stone-passage rates with regard to stone size (≤5 mm vs. >5 mm) or location in the ureter.25
A subsequent double-blind, randomized, placebo-controlled, multicenter trial assessed the efficacy and safety of tamsulosin 0.4 mg compared with placebo.26 Approximately 400 patients aged ≥18 years with symptoms of renal colic and a kidney stone in the distal ureter ≤10 mm that was demonstrated on CT were included. Patients were excluded if they had a temperature >38˚C, a glomerular filtration rate <60 mL/ min, a stone diameter >10 mm, a solitary or transplanted kidney, a history of ureteral strictures, a known allergic reaction to the study medication, or a systolic blood pressure <100 mmHg; were taking a current calcium channel blocker or alpha-blocker; or were pregnant or planning to become pregnant. This trial concluded that, overall, there was no benefit of tamsulosin compared with placebo. However, in patients with large stones (5-10 mm), tamsulosin significantly increased the like-lihood of stone passage at 4 weeks.26
Alpha-Receptor Blockers: Alpha-receptor blockers have been shown to facilitate stone passage with or without ESWL. Alpha-blockers enable smooth-muscle relaxation, inhibit peristalsis, relieve spasm, and decrease the force and frequency of ureteral contraction, which may facilitate stone passage.7,8,11 Although tamsulosin is one of the most commonly used alpha-blockers, studies evaluating other alpha-blockers have demonstrated similar effects, indicating a possible class effect.7
Alpha-blocking agents are generally well tolerated and inexpensive. However, patients taking alpha-blockers are at increased risk for postural hypotension, dizziness, and syncope. Other common side effects of alpha-blockers include nasal congestion, ejaculatory disturbances, and hypotension.11,22 Allergic reactions to tamsulosin are possible in patients with sulfonamide sensitivity; accordingly, tamsulosin should be used with caution in patients with a severe sulfonamide allergy.22
In patients undergoing cataract surgery, intraoperative floppy iris syndrome is associated with alpha-blocker treatment.11,22 Intraoperative floppy iris syndrome was observed during cataract surgery in some patients receiving alpha-blocking medications. Most reported cases were in patients who continued alpha-blocker therapy during the time of cataract surgery.22
Calcium Channel Blockers: The calcium channel blocker nifedipine has been studied in the facilitation of kidney-stone passage. Nifedipine has been shown to relax smooth muscle in the distal ureter.11 Although nifedipine has been shown to improve stone expulsion in distal kidney stones <10 mm, when patients taking nifedipine are compared with patients not receiving MET, it is less effective than alpha-blocking agents.7,22
Nifedipine may cause additive hypotension in patients concurrently taking antihypertensive agents or in those who are not hypertensive at baseline. It may also increase the incidence of peripheral edema and the risk of heart failure.22
Chemolysis and Urinary Alkalinization
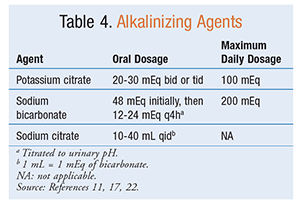
Potassium citrate should be offered to patients with recurrent uric acid, cystine, or calcium stones and low or normal urinary citrate.2 Oral chemolysis (i.e., dissolution) is most beneficial in the treatment of uric acid stones. Oral chemolysis of uric acid kidney stones is based on urinary alkalinization to a goal pH of 7.0 to 7.2.7,8 Persistently low urinary pH (≤5.5) is the most important factor in the formation of uric acid stones.8 The same medications (TABLE 4) that are used for oral chemolysis are also used to alkalinize the urine to prevent new kidney stone formation. Alkalinization therapy is also associated with a reduced risk of recurrent uric acid, cystine, and calcium stones.2
Alkalinization with potassium citrate, sodium citrate, or sodium bicarbonate may be used in conjunction with MET to facilitate stone passage.8,11 Potassium citrate is preferred over sodium bicarbonate or sodium citrate because the increase in sodium intake can lead to further urine calcium excretion, which opposes the benefits of raising urine citrate.2,11 Citrate in urine also has a protective effect on calcium crystal formation because it inhibits kidney stone growth by chelating the calcium ions.11
Common adverse effects of all alkalinizing agents include gastrointestinal upset, abdominal bloating, and diarrhea.11,17,22 It is important for the patient to maintain adequate hydration while taking these agents because urinary alkalinization may increase the risk of calcium phosphate stones.11 The use of potassium citrate is contraindicated in patients with renal insufficiency or chronic renal failure.22 Potassium-containing products may cause hyperkalemia in patients with renal insufficiency and in those concomitantly taking medications that limit renal potassium excretion (e.g., potassium-sparing diuretics, ACE inhibitors, angiotensin II receptor blockers); therefore, alternative treatment with a sodium formulation (sodium citrate, sodium bicarbonate) should be considered.11,17,22
PREVENTION
After an initial kidney stone, the recurrence rate is approximately 30% to 50% within 5 years and 60% to 80% within a lifetime.13,16 In addition to acute management of nephrolithiasis, patient education and treatment to prevent stone recurrence are necessary. Various dietary modifications may contribute to the reduced likelihood of stone recurrence.
For patients who have recurrent nephrolithiasis despite adequate fluid intake, pharmacologic treatment with a thiazide diuretic, citrate, or allopurinol is recommended to prevent stone recurrence.16
Diuretics
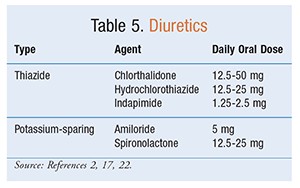
See TABLE 5 for a summary of diuretics used to prevent nephrolithiasis.
Thiazide Diuretics: Thiazide diuretic treatment is appropriate for the prevention of recurrent calcium stones.2,11,16 High-risk patients, such as those with a solitary kidney, hypertension, or a large stone burden or who are refractory to dietary interventions, might also benefit from thiazide therapy.2 Thiazides decrease urine calcium by increasing calcium absorption in the proximal tubule.11 The side effects of thiazide diuretics are dose-dependent and include hypokalemia, hyperglycemia, hyperlipidemia, hyperuricemia, hypo-magnesemia, gout, and hypocitraturia.11,17 Associated hypokalemia or hypocitraturia should be treated with potassium citrate.17
Potassium-Sparing Diuretics: Nonthiazide diuretics (e.g., amiloride and spironolactone) increase water excretion while conserving potassium. Therefore, they may prevent the need for potassium supplementation that may be required with thiazide therapy. These diuretics lower urinary calcium to a lesser extent com-pared with thiazide diuretics.2,22 Triamterene should be avoided because it has been found to provoke stone formation through precipitation of the drug.2
Urate-Lowering Therapy
Urate-lowering therapy (ULT) should not be offered first-line to patients with uric acid stones; however, it may be considered when urinary alkalinization is unsuccessful.2 Uric acid stone formers and patients who have recurrent calcium oxalate stones plus a history of gout or hyperuricosuria refractory to dietary interventions may also benefit from ULT with allopurinol (100-300 mg daily).2,17 Common side effects of allopurinol include liver-enzyme abnormalities and rash.17
Dietary Interventions
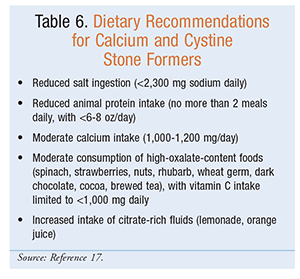
Observational and case-control trials have shown that dietary interventions are associated with a reduction in kidney stone recurrence.2,27 The goal of dietary interventions is to promote changes in the urinary environment that prevent stone formation and growth.2 In addition to the recommended fluid intake, dietary interventions (TABLE 6) including normal calcium, reduced sodium, and reduced animal protein are protective against the risk of stone formation.2,16,27
Calcium: Although it seems counterintuitive, a low-calcium diet is strongly discouraged in calcium stone formers because lower dietary calcium intake is associated with increased stone formation.17 In one study, patients with normal or high dietary calcium intake (1,200 mg/ day) were less likely to experience stone recurrence compared with patients with low dietary calcium intake (400 mg/day).16 Therefore, dietary calcium intake of 1,000 mg to 1,200 mg daily is encouraged for most individuals, as it is associated with a reduced risk of stone recurrence.2,16 However, calcium supplementation has been associated with an increased risk of stone formation and should be avoided.2
Sodium: Dietary sodium is linked to urinary calcium excretion and the potential for increased stone formation.2,17 Sodium restriction (<2,300 mg daily) should be encouraged, especially in patients taking thiazide diuretics, in order to maintain the hypocalciuric effect and limit potassium loss.2
Protein: Moderate animal protein intake (<6-8 oz/day) is recommended for patients with kidney stones of any composition. Decreased animal protein intake causes a reduction of urinary calcium, uric acid, and oxalate, leading to decreased stone recurrence.2,15,17
Fruits and Vegetables: Vegetables and both citrus and noncitrus fruits (e.g., melon, cranberry) are associated with a reduction in kidney stone formation.They increase body citrate, leading to higher urine pH, and may be considered as an alternative to pharmacologic citrate therapy in patients intolerant to the alkalinizing agents. Fruit juices may also reduce the risk of stone formation; however, the evidence of a benefit is less clear.2,15
Complementary and Alternative Supplementation
Vitamin C and other supplements should be avoided.2,15 Turmeric supplements, cranberry supplements, and high doses of vitamin C (ascorbic acid) contribute to increased urine oxalate. Evidence for the use of vitamin B6 (pyridoxine), omega-3 fatty acids, and probiotics is limited.2
SPECIAL POPULATIONS
Pediatric Patients
Kidney stones in pediatric patients are similar in composition to those in adults. Ultrasound is recommended as the initial imaging method to evaluate children with suspected kidney stones. Noncontrast CT should be reserved for individual pediatric patients in whom ultrasound is nondiagnostic and the suspicion of nephrolithiasis remains high. Management of nephrolithiasis in pediatric patients is primarily extrapolated from therapy for adult patients, and all treatments used in adult patients are assumed to be as efficacious in pediatric patients; however, long-term efficacy in this population is unknown.28
Pregnancy
Nephrolithiasis during pregnancy is associated with recurrent miscarriages, mild preeclampsia, cesarean delivery, gestational diabetes mellitus, chronic hypertension, urinary tract infections, hydronephrosis, and hydroureter.29 Imaging techniques are limited in pregnancy compared with usual care.7,8 To avoid radiation exposure, ultrasound is the primary diagnostic tool for detecting stones during pregnancy. Low-dose CT or MRI may also be used. CT has potential hazards and should be reserved for selected cases.7 Conservative management with hydration and analgesia is preferred in pregnancy because most ureteral stones are expected to pass spontaneously. The need for immediate emergency management is the same as in nonpregnant patients. In addition to sepsis, renal failure, and unrelenting pain, the induction of premature labor or fetal distress is cause for immediate intervention with nephrostomy-tube or ureteralstent insertion. Pregnancy is a contraindication to ESWL and should be avoided.7,8
CONCLUSION
The prompt evaluation and management of nephrolithiasis is important because of the risk of poor outcomes associated with obstructive kidney stones and infection. Emergency treatment is required for obstructing stones and urosepsis. The use of fluids should be individualized and targeted to maintain adequate urine volume. Treatment with MET is controversial, and the pros and cons of these therapies must be considered. Education on the prevention of recurrent stones should be provided to all patients because the risk of recurrence is high. Dietary modifications and consistent hydration targeting a urine volume >2 L per day are important in the prevention of recurrent nephrolithiasis.
REFERENCES
- Scales CD Jr, Smith AC, Hanley JM, Saigal CS; Urologic Diseases in America Project. Prevalence of kidney stones in the United States. Eur Urol. 2012;62:160-165.
- Pearle MS, Goldfarb DS, Assimos DG, et al; American Urological Association. Medical management of kidney stones: AUA guideline. J Urol. 2014;192:316-324.
- Curhan GC. Epidemiology of stone disease. Urol Clin North Am. 2007;34:287-293.
- Smith-Bindman R, Aubin C, Bailitz J, et al. Ultrasonography versus computed tomography for suspected nephrolithiasis. N Engl J Med. 2014;371:1100-1110.
- Uribarri J, Oh MS, Carroll HJ. The first kidney stone. Ann Intern Med. 1989;111:1006-1009.
- Frassetto L, Kohlstadt I. Treatment and prevention of kidney stones: an update. Am Fam Physician. 2011;84:1234-1242.
- Türk C, Knoll T, Petrik A, et al. European Association of Urology guidelines on urolithiasis. http://uroweb.org/wp-content/uploads/EAU-Guidelines-Urolithiasis-2015-v2.pdf. Accessed March 29, 2016.
- Ordon M, Andonian S, Blew B, et al. CUA Guideline: management of ureteral calculi. Can Urol Assoc J. 2015;9:e837-e851.
- Flannigan R, Choy WH, Chew B, Lange D. Renal struvite stones—pathogenesis, microbiology, and management strategies. Nat Rev Urol. 2014;11:333-341.
- Bratzler DW, Dellinger EP, Olsen KM, et al; American Society of Health-System Pharmacists; Infectious Diseases Society of America; Surgical Infection Society; Society for Healthcare Epidemiology of America. Clinical practice guidelines for antimicrobial prophylaxis in surgery. Am J Health Syst Pharm. 2013;70:195-283.
- Xu H, Zisman AL, Coe FL, Worcester EM. Kidney stones: an update on current pharmacological management and future directions. Expert Opin Pharmacother. 2013;14:435-447.
- Marien T, Miller NL. Treatment of the infected stone. Urol Clin North Am. 2015;42:459-472.
- Parsa MD, Khafi MM. Current management of nephrolithiasis. Emerg Med. 2016;48:106-113.
- Worster AS, Bhanich Supapol W. Fluids and diuretics for acute ureteric colic. Cochrane Database Syst Rev. 2012;(2):CD004926.
- Prezioso D, Strazzullo P, Lotti T, et al; CLU Working Group. Dietary treatment of urinary risk factors for renal stone formation. A review of CLU Working Group. Arch Ital Urol Androl. 2015;87:105-120.
- Qaseem A, Dallas P, Forciea MA, et al; Clinical Guidelines Committee of the American College of Physicians. Dietary and pharmacologic management to prevent recurrent nephrolithiasis in adults: a clinical practice guideline from the American College of Physicians. Ann Intern Med. 2014;161:659-667.
- Paterson R, Fernandez A, Razvi H, Sutton R. Evaluation and medical management of the kidney stone patient. Can Urol Assoc J. 2010;4:375-379.
- Golzari SE, Soleimanpour H, Rahmani F, et al. Therapeutic approaches for renal colic in the emergency department: a review article. Anesth Pain Med. 2014;4:e16222.
- Pathan SA, Mitra B, Straney LD, et al. Delivering safe and effective analgesia for management of renal colic in the emergency department: a double-blind, multigroup, randomised controlled trial. Lancet. 2016;387:1999-2007.
- Holdgate A, Pollock T. Nonsteroidal anti-inflammatory drugs (NSAIDs) versus opioids for acute renal colic. Cochrane Database Syst Rev. 2005;(2):CD004137.
- Afshar K, Jafari S, Marks AJ, et al. Nonsteroidal anti-inflammatory drugs (NSAIDs) and non-opioids for acute renal colic. Cochrane Database Syst Rev. 2015;(6):CD006027.
- Lexicomp Online. Hudson, OH: Lexi-Comp, Inc; 2016. http://online. lexi.com. Accessed May 31, 2016.
- Hollingsworth JM, Rogers MA, Kaufman SR, et al. Medical therapy to facilitate urinary stone passage: a meta-analysis. Lancet. 2006;368:1171-1179.
- Preminger GM, Tiselius HG, Assimos DG, et al. American Urological Association Education and Research, Inc; European Association of Urology. 2007 guideline for the management of ureteral calculi. Eur Urol. 2007;52:1610-1631.
- Pickard R, Starr K, MacLennan G, et al. Medical expulsive therapy in adults with ureteric colic: a multicentre, randomised, placebo-controlled trial. Lancet. 2015;386:341-349.
- Furyk JS, Chu K, Banks C, et al. Distal ureteric stones and tamsulosin: a double-blind, placebo-controlled, randomized, multicenter trial. Ann Emerg Med. 2016;67:86-95.e2.
- Fink HA, Wilt TJ, Eidman KE, et al. Medical management to prevent recurrent nephrolithiasis in adults: a systematic review for an American College of Physicians Clinical Guideline. Ann Intern Med. 2013;158:535-543.
- Tasian GE, Copelovitch L. Evaluation and medical management of kidney stones in children. J Urol. 2014;192:1329-1336.
- Tan YK, Cha DY, Gupta M. Management of stones in abnormal situations. Urol Clin North Am. 2013;40:79-97.
- Carter MR, Green BR. Renal calculi: emergency department diagnosis and treatment. Emerg Med Pract. 2011;13:1-17.
- Kumar S, Dave A, Wolf B, Lerma EV. Urinary tract infections. Dis Mon. 2015;61:45-59.