Advancements in the Management of Schizophrenia
RELEASE DATE
May 1, 2024
EXPIRATION DATE
May 31, 2026
FACULTY
Yvette C. Terrie, BS Pharm, RPh
Clinical Pharmacist/Freelance Medical Writer
Haymarket, Virginia
FACULTY DISCLOSURE STATEMENTS
Dr. Terrie has no actual or potential conflicts of interest in relation to this activity.
Postgraduate Healthcare Education, LLC does not view the existence of relationships as an implication of bias or that the value of the material is decreased. The content of the activity was planned to be balanced, objective, and scientifically rigorous. Occasionally, authors may express opinions that represent their own viewpoint. Conclusions drawn by participants should be derived from objective analysis of scientific data.
ACCREDITATION STATEMENT
 Pharmacy
Pharmacy
Postgraduate Healthcare Education, LLC is accredited by the Accreditation Council for Pharmacy Education as a provider of continuing pharmacy education.
UAN: 0430-0000-24-055-H01-P
Credits: 2.0 hours (0.20 ceu)
Type of Activity: Knowledge
TARGET AUDIENCE
This accredited activity is targeted to pharmacists. Estimated time to complete this activity is 120 minutes.
Exam processing and other inquiries to:
CE Customer Service: (800) 825-4696 or cecustomerservice@powerpak.com
DISCLAIMER
Participants have an implied responsibility to use the newly acquired information to enhance patient outcomes and their own professional development. The information presented in this activity is not meant to serve as a guideline for patient management. Any procedures, medications, or other courses of diagnosis or treatment discussed or suggested in this activity should not be used by clinicians without evaluation of their patients' conditions and possible contraindications or dangers in use, review of any applicable manufacturer's product information, and comparison with recommendations of other authorities.
GOAL
To expand pharmacists' knowledge of schizophrenia management and the optimization of treatment through patient and caregiver education.
OBJECTIVES
After completing this activity, the participant should be able to:
- Describe the incidence, proposed pathogenesis, risk factors, clinical presentation, and diagnosis of schizophrenia.
- Discuss the American Psychiatric Association's practice guideline recommendations for schizophrenia treatment.
- Explain the recommended pharmacologic and nonpharmacologic therapies for schizophrenia.
- Define the pharmacist's role in managing schizophrenia, including counseling patients and caregivers about proper use of the selected therapy.
ABSTRACT: Schizophrenia is a complex, severe, and chronic mental health disorder characterized by hallucinations, delusions, phobia, disordered and abnormal thinking and behaviors, social and emotional challenges in relationships, and functional difficulty with daily tasks. Although there is no cure, advances in research have led to greater insight into the factors that may contribute to the pathogenesis of schizophrenia. In 2020, the American Psychiatric Association released an evidence-based practice guideline for the treatment of schizophrenia. Early diagnosis, clinical intervention, and patient adherence are important for effective management and improving clinical outcomes. Management generally involves long-term therapy with antipsychotics and psychotherapy, and treatment plans should be individualized to patient needs. Pharmacists can help develop patient-centered treatment plans and educate patients and caregivers about the selected therapy.
Schizophrenia, a severe and chronic mental health disorder, is characterized by a heterogeneous array of symptoms including (but not limited to) disruptions in thought processes, perceptions, emotional responsiveness, paranoia, and hallucinations.1,2 Although the clinical presentation and course of schizophrenia vary among individuals, this disorder imposes significant health and economic burdens on the patient, family members, society, and the healthcare system.1,2
INCIDENCE
According to the National Institute of Mental Health (NIMH), schizophrenia is one of the top 15 causes of disability in the United States and globally.1,2 The NIMH notes that although schizophrenia's precise incidence remains unknown because of its complexity and its common occurrence with other disorders, it is estimated that schizophrenia and related psychotic disorders occur in 0.25% to 0.64% of the U.S. population.2 The most recent statistics from the World Health Organization reveal that schizophrenia affects an estimated 24 million people globally (one in 300 individuals, or 0.32% of the population), including those in late adolescence; among adults, the rate is one in 222 individuals (0.45%).3
Rates of schizophrenia are low compared with other psychiatric disorders; however, schizophrenia frequently goes undiagnosed and underreported, and it often remains untreated as well.4 According to the Mental and Substance Use Disorders Prevalence Study (MDPS), which was published in 2023, an estimated 37 million U.S. adults aged 18 to 65 years (1.8%) had a lifetime history of schizophrenia spectrum disorders; additionally, in the past year, an estimated 1.2% of adults (an estimated 2.5 million individuals aged 18 to 65 years) met diagnostic criteria for a schizophrenia spectrum disorder, with prevalence rates two to three times higher than those reported by prior studies.5 The MDPS is the first study to approximate the prevalence of schizophrenia spectrum disorders in the U.S.5
Schizophrenia affects males and females equally, but males frequently experience an earlier disease onset.6 The symptom course and severity differ from patient to patient.6 According to the American Psychiatric Association (APA), the estimated lifetime incidence of schizophrenia is 0.7%; however, outcomes differ and are contingent upon demographics and other variables.6 The National Alliance on Mental Health notes that although schizophrenia can manifest at any age, it typically begins during the late teen years and early 20s in males, and during the late 20s to early 30s in females.7 It is uncommon for schizophrenia to be diagnosed in persons younger than age 12 years or those older than age 40 years.7
PATHOGENESIS AND RISK FACTORS
Multiple biological, psychological, and social environmental risk factors have been correlated with the development of schizophrenia.8-16 Although the precise pathogenesis of schizophrenia is largely unknown, significant advances have been made toward understanding the disorder, and clinical data indicate that schizophrenia involves a complex interaction between genetic and external or environmental factors.8,9 It has been hypothesized that neurotransmitter imbalances in dopamine, serotonin, glutamate, and gamma-aminobutyric acid could be a cause; other theories suggest that variations in brain structure, such as enlarged cerebral ventricles, thinning of the cortex, and reduced size of the anterior hippocampus and other brain regions, may also contribute to the pathogenesis.16,17 A recent study involving twins revealed that nearly 79% of schizophrenia risk may be attributed to genetic factors.13 Other studies have found that monozygotic twins have an estimated 40% to 50% risk of developing schizophrenia, and the risk is 40% if both parents have schizophrenia.14-16
Although schizophrenia has genetic links, well documented nongenetic risk factors, including certain infections (e.g., Toxoplasma gondii, cytomegalovirus), cannabis use, psychosocial stress, childhood adversity, urban environment, and immigrant status also can contribute to its development.9 Environmental factors can impact gene expression, and an individual's genetic makeup can also affect the response to environmental stressors.8-11 Inflammation may also play a role in the development of schizophrenia because inflammation contributes to augmented activation of the immune system, which causes higher levels of circulating proinflammatory cytokines, and elevated proinflammatory cytokine levels have commonly been observed in patients with schizophrenia.12
Several studies have documented epidemiologic risk factors that are correlated with an increased risk of developing schizophrenia. Expanding on the risk factors mentioned earlier, these include—but are not restricted to—neurodevelopmental factors, including obstetric complications such as preeclampsia, low birthweight, and bleeding during pregnancy; exposure to certain viruses; cognitive impairments and brain abnormalities; substance use, including cannabis, amphetamines, and cocaine; trauma and social adversity during either childhood or adulthood; and advanced paternal age at conception.8-16
CLINICAL PRESENTATION
Although the clinical presentation of schizophrenia varies from patient to patient, the characteristic symptom associated with schizophrenia is psychosis (i.e., auditory hallucinations and delusions).6,7,17 In general, schizophrenia patients exhibit psychotic symptoms a mean of 8 to 15 months before obtaining medical evaluation; however, with the establishment of diagnostic criteria, schizophrenia is often identified earlier in the disease course, thus improving the probability of early clinical intervention.17 According to the APA, the distinguishing manifestations of schizophrenia characteristically include positive symptoms, disorganized speech, negative symptoms, and impairments in cognition, which are commonly associated with impaired social and occupational functioning.6,17
Similarly, the clinical presentation of schizophrenia is formally categorized into four domains: positive symptoms, negative symptoms, cognitive symptoms, and disorganization.6,17,18 Positive symptoms (those abnormally present) include hallucinations; paranoia; delusions; and exaggerated or distorted perceptions, beliefs, and behaviors. Negative symptoms (those abnormally absent) include a reduction or loss of normal functions and affect, including the ability to initiate plans, converse, or express emotion. Cognitive symptoms include impairments in memory, information processing, and problem-solving skills. Disorganization involves thought disorder, including confused thinking and speech and odd behavior.6,17,18 Signs and symptoms typically manifest during the teenage years or early adulthood.6,17,18 Because the clinical presentation varies from patient to patient, patients may exhibit signs and symptoms from one or all categories.6,7,17,18
Schizophrenia patients often have a higher incidence of other psychiatric conditions, such as depressive disorders, social anxiety disorders, obsessive-compulsive disorder (OCD), posttraumatic stress disorder, and a history of substance use disorders, including alcohol abuse. One study reported that 47% of individuals with schizophrenia battled drug or alcohol abuse, compared with 16% of those who did not have schizophrenia.19,20 Schizophrenia patients also have higher rates of suicidal ideation and suicidal behavior compared with those without schizophrenia.21,22 In general, persons with schizophrenia have a 4.5-fold increased risk of death by suicide.22
Schizophrenia comprises several phases: prodromal, acute, and residual. The prodromal phase may develop slowly over years, with patients exhibiting social withdrawal, decreased productivity, loss of motivation or interest in things, unusual rituals, illogical beliefs or superstitions, and odd sensory experiences; they may be unmotivated to maintain routine hygiene and may disconnect emotionally. In the acute phase, signs and symptoms must have a duration of at least 1 month, with the addition of anxiety, irritability, and anger (these signs may be more intense than in other disease phases); the patient also exhibits apparent disorganized behavior or difficulty thinking or speaking clearly and experiences hallucinations and delusions. In the residual phase, symptoms can endure for years and are often most disabling, with the addition of depression. Behavioral symptoms of the residual phase are comparable to prodromal-phase symptoms, but patients may have persistent and lower levels of functioning and disorganized behavior; they also have cognitive deficits, delusions, and hallucinations, but they are less intense.6,17,23,24
DIAGNOSIS
Early diagnosis, clinical intervention, and adherence to therapy are associated with better clinical outcomes. Diagnosing schizophrenia entails ruling out other mental health disorders, and clinicians typically conduct a physical examination and order screening tests, including laboratory testing, using the criteria established by the APA's Diagnostic and Statistical Manual of Mental Disorders, 5th Edition.25 For a confirmed diagnosis of schizophrenia, both of the following criteria must be met: 1) the presence of two or more typical symptoms (delusions, hallucinations, disorganized speech, disorganized behavior, negative symptoms) for at least 6 months (must include at least one of the first three symptoms), and 2) prodromal or attenuated signs of illness, with social, occupational, or self-care deficiencies apparent for 6 months, including 1 month of active symptoms.17,25,26
In September 2020, the APA released an evidence-based practice guideline for the treatment of patients with schizophrenia. The primary goals of the new guideline are to improve early recognition and diagnosis and to enhance treatment to reduce the morbidity, psychosocial and health consequences, and mortality rates associated with schizophrenia.26 TABLE 1 lists APA guideline recommendations for patient evaluation.26

The diagnosis of schizophrenia early in the disease course helps increase the odds of improved clinical outcomes. In a recent study, researchers described precision medicine findings that could make it easier to screen for current severity of and future risk of schizophrenia.27 The researchers were able to detect biomarkers that were predictive of both high hallucinations and high delusion states as well as future psychiatric hospitalizations related to both of the former; additionally, some of the biomarkers were targets of existing drug therapies.27
ASSOCIATED COMORBIDITIES
The NIMH has said that schizophrenia is one of the primary causes of disability globally, and some studies demonstrate that schizophrenia patients have a 12-fold higher mortality risk compared with the general population, with reasons including somatic comorbidities, unhealthy lifestyle, and increased suicide rates.26,28,29 Premature mortality, which is two to three times more likely in those with schizophrenia than in the general population, often results from other comorbidities.28-32 Compared with the general population, schizophrenia patients also have a heightened risk of cardiovascular disease, dyslipidemia, dementia, sleep disorders, eating disorders, and type 2 diabetes, with a resulting decrease in average lifespan of up to 20 years.28-32
Schizophrenia can occur in conjunction with other mental health conditions, such as OCD.17 It is estimated that 80% of schizophrenia patients also experience one or more episodes of major depression in their lifetime.17
MANAGEMENT
The management of schizophrenia typically entails a multidisciplinary approach that incorporates the implementation of both pharmacologic and nonpharmacologic treatments, with the latter including psychotherapy and cognitive-behavioral therapy (CBT). Although psychosocial and psychotherapeutic interventions are essential for improving outcomes, antipsychotic drug therapy remains the foundation of managing schizophrenic psychosis.26
According to the APA guideline, schizophrenia treatment is generally divided into three phases: acute, stabilization, and maintenance. The goal of maintenance therapy is to prevent the recurrence or relapse of schizophrenia episodes in outpatients.26 In general, the treatment goals for schizophrenia include identifying and addressing factors that cause acute episodes, establishing short-term and long-term goals, improving symptoms, reducing or preventing adverse drug reactions (ADRs), preventing relapses, and enhancing the patient's productivity and quality of life (QoL).26 Clinical data from the NIMH's RAISE (Recovery After an Initial Schizophrenia Episode) initiative show that the earlier treatment is initiated and the more intensive it is, the better the outcome.33
APA Schizophrenia Treatment Guideline
Despite extensive, robust research on the treatment of schizophrenia, many patients do not receive evidence-based pharmacologic and nonpharmacologic therapies.26,34 The APA guideline recommends that patients receive a documented, comprehensive, and patient-centered treatment plan that includes evidence-based nonpharmacologic and pharmacologic therapies.26 Clinicians should consider certain factors when prescribing medications, such as the patient's treatment preferences, current medical and medication history, ADR profile, risk factors, presence of other comorbidities, dosage formulations and frequency of administration, response to previous therapies (if applicable), tolerability, potential contraindications, history of adherence to previous therapies, drug-drug interactions, and drug costs. Clinicians should also discuss the risks versus benefits of selected therapies compared with other options. With regard to pharmacotherapy, the APA recommends the following26:
- Patients should receive antipsychotic therapy and should be monitored for effectiveness and ADRs.
- Antipsychotic therapy should be continued in patients with improved symptoms.*
- It is suggested that patients who have had symptom improvement with an antipsychotic agent continue treatment with the same antipsychotic agent.*
- Patients with treatment-resistant schizophrenia should receive clozapine treatment.*
- Patients should receive clozapine treatment if the risk of suicide attempts or suicide remains substantial in spite of other treatments.*
- It is suggested that patients receive clozapine treatment if the risk of aggressive behavior remains considerable regardless of other therapies.*
- It is suggested that patients receive long-acting injectable (LAI) antipsychotic treatment if they favor it or have a history of poor or uncertain adherence.*
- Patients with acute dystonia related to antipsychotic therapy should be treated with an anticholinergic agent.
- In patients with parkinsonism related to antipsychotic therapy, suggested options include lowering the antipsychotic dosage, switching to a different antipsychotic, or initiating an anticholinergic agent.
- In patients with akathisia related to antipsychotic therapy, suggested options include lowering the antipsychotic dosage, switching to a different antipsychotic, or adding a benzodiazepine or beta-adrenergic blocker.
- Patients with moderate-to-severe or disabling tardive dyskinesia related to antipsychotic therapy should receive treatment with a reversible inhibitor of the vesicular monoamine transporter 2.
The APA guideline advises that the statements marked with an asterisk (*) should be implemented in the context of a person-centered treatment plan including evidence-based pharmacologic and nonpharmacologic schizophrenia therapies.
Pharmacologic Management
A variety of antipsychotic agents, available in a number of different dosage forms, are effective for reducing the psychotic symptoms present in the acute phase of schizophrenia.6 These medications can also help lessen the potential for future acute episodes as well as their severity.6
In the absence of contraindications, antipsychotics are standard first-line therapy; their use has been extensively studied, and they have been shown to be effective for treating schizophrenia.34-36 A meta-analysis of 402 studies involving more than 50,000 participants examined the efficacy of more than 30 different first-generation and second-generation antipsychotics in patients with acute symptoms of schizophrenia or related disorders.35 All of the antipsychotics in the meta-analysis were determined to decrease overall symptoms more than placebo.35
To lessen symptoms, improve QoL, maintain function, and reduce rates of relapse and rehospitalization, effective management of schizophrenia requires early intervention with patient-centered treatment plans, establishment of treatment goals, patient adherence, and routine monitoring and implementation of both pharmacologic measures and nonpharmacologic measures.26,35,37-39 Some examples of nonpharmacologic measures include CBT and supportive psychotherapy tailored to patient need.
First-Generation Versus Second-Generation Antipsychotics: The APA recommends that patients with schizophrenia receive antipsychotic therapy and monitoring for effectiveness and ADRs.26 Both first-generation antipsychotics (FGAs) and second-generation antipsychotics (SGAs), which were developed in the 1950s and 1980s, respectively, may be used for the treatment of schizophrenia.40 FGAs and SGAs (except clozapine) are indicated for treatment of an acute episode of psychosis and as maintenance therapy for schizophrenia and schizoaffective disorders.41 FGAs and SGAs have comparable clinical efficacy, with the exception of clozapine, an SGA with unique efficacy in treatment-resistant schizophrenia.41 FGAs (also known as typical antipsychotics) are better for treating positive symptoms of schizophrenia, such as hallucinations and delusions, and also reduce the risk of a repeat episode of psychosis.40-42 SGAs (also known as atypical antipsychotics) are serotonin-dopamine antagonists; they are often prescribed to treat positive symptoms and negative symptoms of schizophrenia, such as withdrawal, detachment, and ambivalence, and are proven effective for reducing relapse.41 See TABLE 2 for a brief summary of selected FGAs and TABLE 3 for a brief summary of selected SGAs.40-44

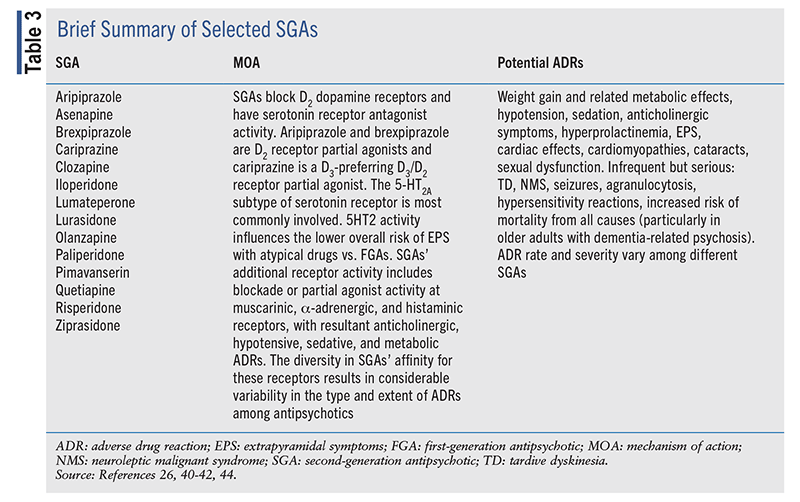
The APA guideline notes that the substantial heterogeneity in designs of clinical trials, the limited amount of trial data for some antipsychotics, and the small number of head-to-head comparisons of antipsychotics prevent an evidence-based ranking of SGAs and FGAs or an algorithmic approach to the selection of antipsychotics. Similarly, a preference for either SGAs or FGAs cannot be determined at present. Although clinically meaningful distinctions may exist in the response to, and tolerability of, different antipsychotics in individual patients, no definitive evidence exists—except possibly for clozapine—that one antipsychotic will have consistently superior efficacy over another antipsychotic.26
A recent review found that FGAs might provoke hyperprolactinemia and frequent adverse motor effects, such as extrapyramidal symptoms (EPS), which can contribute to decreased therapy adherence and increase disability and stigmas related to schizophrenia.39 In some studies, adherence was higher in patients taking SGAs versus those taking FGAs. Both FGAs and SGAs are effective for relieving positive symptoms of schizophrenia; however, efficacy for negative, affective, and cognitive symptoms is lacking, and these aspects of the disease remain unmet needs in schizophrenia treatment.39
Although trial data vary, SGA use has been associated with a reduced incidence of extrapyramidal ADRs compared with FGAs, with a few distinctions between the classes.39 In first-episode patients, the incidence of metabolic syndrome and weight gain is three times higher with SGA use compared with FGA use.39 SGAs have demonstrated greater efficacy than FGAs in terms of relapse-free survival and rates of psychiatric hospitalization as well as for treating negative symptoms.39 A recent study that compared the efficacy of FGAs and SGAs for treating schizophrenia discovered that xerostomia, sedation, and EPS were common with FGAs, whereas xerostomia, cardiac arrhythmias, and sexual dysfunction were common with SGAs.40,41
Inadequate Treatment Response and Treatment Resistance: Approximately 10% to 30% of patients with schizophrenia are refractory to antipsychotic drugs, and an additional 50% to 60% achieve only a partial response.42,45 An estimated 20% to 30% of schizophrenia patients experience treatment resistance (insufficient response to two antipsychotics, each at an adequate dose and duration), which is linked to poorer outcomes, worsened social functioning, and augmented risk of suicide.46-49
Clozapine is the only agent approved for treatment-resistant schizophrenia, and it is often underprescribed.50 In a recent study investigating the experiences of 1,487 patients taking clozapine, most patients reported positive experiences with clozapine, with overall high degrees of satisfaction, symptom improvement, and preference over previously used medications.46 Negative experiences were less common, primarily comprising issues related to required blood testing (monitoring for risk of clozapine-induced agranulocytosis and neutropenia) and common ADRs (e.g., weight gain, hypersalivation).46 The APA guideline recommends that when clozapine is being considered, clinicians should discuss the benefits versus harms of therapy and employ shared decision-making strategies to ascertain what is best for the individual patient. The APA adds that when clozapine is initiated, slow dose titration is critical to reduce the risk of seizures, orthostatic hypotension, and excessive sedation, and routine monitoring is essential.26
LAI Antipsychotics: Because LAI antipsychotics provide another route of administration, thereby easing the burden of taking oral formulations daily or multiple times per day, they have the potential to improve adherence rates.38,45,51 The use of LAIs demonstrated a statistically significant reduction in 30-day rehospitalizations compared to oral antipsychotics, and hospital inpatient free trial programs helped increase patient access to LAIs.52 Given the well-documented and robust correlation between nonadherence and rates of relapse among patients with schizophrenia, the use of LAIs has the potential to decrease rates of relapse, slow disease progression, and improve overall long-term outcomes.38,52 In a large literature review, switching to LAIs was significantly associated with a lower incidence of treatment failure compared with oral SGA monotherapy.39 Additionally, patients treated with LAIs demonstrated noteworthy improvements in general functionality, subjective well-being, and total score on global satisfaction tests, as well as improved personal and social performance.39
Some examples of LAI FGAs include fluphenazine and haloperidol, which are potent dopamine blockers that have less receptor activity for other neurotransmitters. LAI SGAs include aripiprazole monohydrate, aripiprazole lauroxil, paliperidone (4-week, 12-week, and 6-month), risperidone (subcutaneous and as microspheres), and olanzapine, which act to block both dopamine receptors and serotonin receptors.53
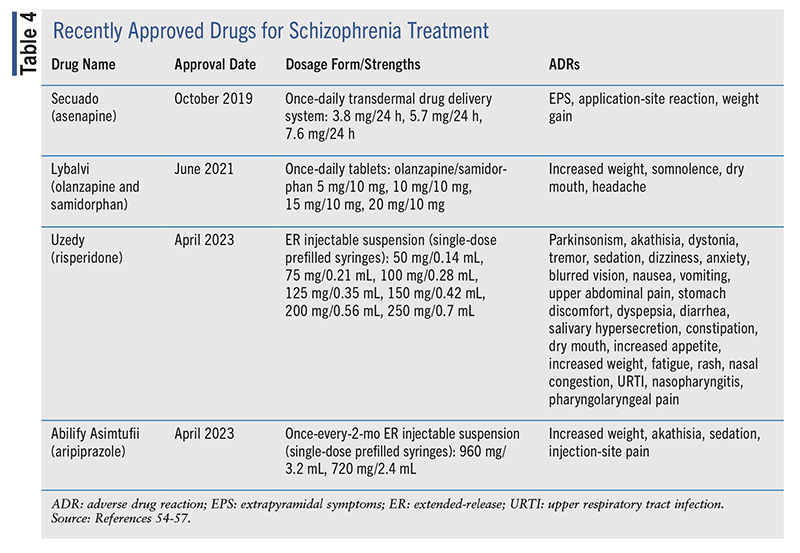
Recent Approvals: Drugs recently approved by the FDA for the treatment of schizophrenia include the first (and only) once-daily transdermal patch, a once-daily tablet combining an atypical antipsychotic with an opioid antagonist, and an extended-release injectable suspension. See TABLE 4 for a brief summary of these recently approved drugs.54-57
Emerging Agent: In November 2023, the FDA accepted the New Drug Application for xanomeline-trospium (KarXT), an agent developed for the treatment of schizophrenia.58 KarXT, which acts as a dual M1 /M4 muscarinic acetylcholine receptor agonist in the central nervous system, is thought to improve positive, negative, and cognitive symptoms of schizophrenia. Unlike other schizophrenia agents, this drug does not directly block dopamine receptors, offering a new approach to treating schizophrenia. The Prescription Drug User Fee Act date has been set for September 26, 2024.58
Nonadherence to Treatment: Only 40% to 60% of schizophrenia patients with documented factors that contribute to treatment nonadherence (ADRs; younger age; lack of understanding about the disease; medication costs; lack of access to care and insurance; low economic status; substance abuse; and negative perceptions about treatment, including lack of perceived therapeutic benefit) adhere to their prescribed medication.39,59-66 Nonadherence to maintenance therapy results in a subsequent episode within 12 months in 70% to 80% of patients, and treatment adherence can reduce the 1-year relapse rate to about 30% or lower with long-acting drugs.17 One-third of patients achieve significant and lasting improvement, one-third improve somewhat but have sporadic relapses and residual disability, and one-third are severely debilitated.17 Some longitudinal studies have found that nonadherence to antipsychotic treatment heightens the risk of psychotic relapses and is correlated with increased risk of substance use, poor cognition, suicidal behavior, and overall mortality.60 Some examples of nonadherence in patients include not filling initial prescriptions, changing the dosing regimen, or completely discontinuing medications.60-62 It is well documented that poor adherence is associated with heightened risk of relapse, rehospitalizations, increased risk of suicidal and aggressive behaviors, and premature mortality.26,63-67
Nonpharmacologic Therapies
The APA guideline states that effective management of schizophrenia also involves the use of psychotherapy, including CBT. Key APA recommendations include the following26:
- Patients who are experiencing a first episode of psychosis should be treated in a coordinated specialty care program.*
- Patients should receive CBT for psychosis; psychoeducation; and supported employment services.*
- Patients with a history of poor engagement with services that leads to frequent relapse or social disruption (e.g., legal difficulties, including imprisonment; homelessness) should receive assertive community treatment.*
- It is suggested that patients receive family interventions if they have ongoing contact with family members.*
- It is suggested that patients receive interventions targeted to developing self-management skills and enhancing person-oriented recovery.*
- It is also suggested that patients receive cognitive remediation.*
- It is suggested that patients with a therapeutic goal of enhanced social functioning receive social-skills training.*
- It is suggested that patients also receive supportive psychotherapy.*
The APA guideline advises that the statements marked with an asterisk (*) should be implemented in the context of a person-centered treatment plan including evidence-based pharmacologic and nonpharmacologic schizophrenia therapies.
UNDIAGNOSED AND UNTREATED SCHIZOPHRENIA
Schizophrenia that remains undiagnosed and untreated presents an array of challenges for the patient, family members, society, and the healthcare system. The estimated annual economic burden associated with schizophrenia is $173.6 billion.68 Compared with the general population, the rates of homelessness and unemployment are higher in individuals with schizophrenia, especially those with undiagnosed and untreated schizophrenia, who are more likely to experience other undiagnosed and untreated health issues and economic, professional, social, and functional challenges in daily life.69 Additionally, lack of healthcare access may increase morbidity and mortality rates.26
THE PHARMACIST'S ROLE
As frontline healthcare providers, pharmacists are well poised to serve as educators and advocates for not only patients with schizophrenia, but also their families and caregivers. Their drug expertise renders pharmacists indispensable in the multidisciplinary care involved in managing schizophrenia. Pharmacists can be instrumental in improving medication therapy outcomes, reducing medication errors, identifying and addressing polypharmacy, monitoring patients for ADRs, and implementing measures to promote adherence, such as refill reminders or reminders that alert patients to take their medication, which can aid in reducing rates of relapse and readmissions.70-72 Pharmacists can also play a key role in screening for potential contraindications and drug-drug interactions and in educating patients about how to identify potential ADRs and when to contact prescribers.
According to the American Pharmacists Association, pharmacists can be instrumental in optimizing care for patients with serious mental illnesses by managing medication therapy, monitoring patient responses, implementing patient-education strategies to improve adherence, and making recommendations when changes in therapy are warranted.71 During counseling, it is critical that pharmacists remind patients about the importance of adherence to the selected therapy because treatment adherence not only reduces the incidence of relapses and rehospitalizations but may also improve overall health-related QoL and patient functioning.70,71 Pharmacists can also make patient-centered recommendations for drug formulations that may increase adherence rates, such as once-daily oral dosage forms, LAIs, and rapidly dissolving tablets for patients with swallowing difficulties.26
By implementing effective and routine patient-education initiatives tailored to the patient's level of understanding, including both verbal and written information, pharmacists can aid in improving rates of adherence and can also encourage patients to learn more about schizophrenia and seek support from available patient resources. Pharmacists can also help patients and family members obtain information about schizophrenia and manufacturer-sponsored savings programs for eligible patients to expand access to therapies. Pharmacists should remind patients about the importance of routine healthcare, including obtaining care for other comorbidities, if applicable.
When counseling patients and caregivers, pharmacists can discuss therapy goals and the proper use of medications—including treatment expectations, dosage, dosing frequency, administration, potential ADRs, and monitoring parameters—as well as the importance of adherence to therapy to improve clinical outcomes and reduce relapse rates. Patients and caregivers should be reminded that therapy discontinuation or nonadherence is a significant risk factor that increases relapse rates and hospital admissions. Pharmacists can also help patients and caregivers understand various aspects of schizophrenia, the established goals of therapy, and the significance of routine care and follow-up with healthcare providers.
CONCLUSION
Because of their accessibility, pharmacists can be instrumental in making patient-centered recommendations regarding drug therapy, and they can help optimize treatment by educating patients and caregivers about the selected medications as well as treatment goals and expectations. Overcoming the stigmas associated with schizophrenia and other mental health disorders is a critical step in encouraging patients to seek medical care. Continued advancements in the treatment of schizophrenia, especially novel therapies that have the potential to improve long-term adherence, hold promise for these patients, and it is hoped that they will improve clinical outcomes and patient health-related QoL while also reducing relapse rates.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
REFERENCES
- GBD 2016 Disease and Injury Incidence and Prevalence Collaborators. Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990-2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet. 2017;390(10100):1211-1259.
- National Institute of Mental Health. Schizophrenia. www.nimh.nih.gov/health/statistics/schizophrenia#part_2543. Accessed April 4, 2024.
- World Health Organization. Schizophrenia. www.who.int/news-room/fact-sheets/detail/schizophrenia. Accessed February 1, 2024.
- Solmi M, Seitidis G, Mavridis D, et al. Incidence, prevalence, and global burden of schizophrenia—data, with critical appraisal, from the Global Burden of Disease (GBD) 2019. Mol Psychiatry. 2023 Jul 27. Epub ahead of print.
- Ringeisen H, Edlund M, Guyer H, et al. Mental and Substance Use Disorders Prevalence Study (MDPS): Findings Report. Research Triangle Park, NC: RTI International; 2023.
- American Psychiatric Association. What is schizophrenia? www.psychiatry.org/patients-families/schizophrenia/what-is-schizophrenia. Accessed February 1, 2024.
- National Alliance on Mental Illness. Schizophrenia. https://nami.org/About-Mental-Illness/Mental-Health-Conditions/Schizophrenia. Accessed February 2, 2024.
- Nakamura T, Takata A. The molecular pathology of schizophrenia: an overview of existing knowledge and new directions for future research. Mol Psychiatry. 2023;28(5):1868-1889.
- Wahbeh MH, Avramopoulos D. Gene-environment interactions in schizophrenia: a literature review. Genes (Basel). 2021;12(12):1850.
- Stilo SA, Murray RM. Non-genetic factors in schizophrenia. Curr Psychiatry Rep. 2019;21(10):100.
- Davis J, Eyre H, Jacka FN, et al. A review of vulnerability and risks for schizophrenia: beyond the two-hit hypothesis. Neurosci Biobehav Rev. 2016;65:185-194.
- Miller BJ, Buckley P, Seabolt W, et al. Meta-analysis of cytokine alterations in schizophrenia: clinical status and antipsychotic effects. Biol Psychiatry. 2011;70(7):663-671.
- Hilker R, Helenius D, Fagerlund B, et al. Heritability of schizophrenia and schizophrenia spectrum based on the nationwide Danish Twin Register. Biol Psychiatry. 2017;83(6):492-498.
- Kringlen E. Twin studies schizophrenia with special emphasis on concordance figures. Am J Med Genet. 2000;97(1):4-11.
- Cardno AG, Marshall EJ, Coid B, et al. Heritability estimates for psychotic disorders: the Maudsley twin psychosis series. Arch Gen Psychiatry. 1999;56(2):162-168.
- Hany M, Rehman B, Azhar Y, Chapman J. Schizophrenia. In: StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing; 2024 Jan-.
- Tamminga C. Schizophrenia. Merck Manual Professional Version. www.merckmanuals.com/professional/psychiatric-disorders/schizophrenia-and-related-disorders/schizophrenia. Accessed April 4, 2024.
- Patel KR, Cherian J, Gohil K, Atkinson D. Schizophrenia: overview and treatment options. P T. 2014;39(9):638-645.
- Masroor A, Khorochkov A, Prieto J, et al. Unraveling the association between schizophrenia and substance use disorder—predictors, mechanisms and treatment modifications: a systematic review. Cureus. 2021;13(7):e16722.
- Kiran C, Chaudhury S. Prevalence of comorbid anxiety disorders in schizophrenia. Ind Psychiatry J. 2016;25(1):35-40.
- Bai W, Liu ZH, Jiang YY, et al. Worldwide prevalence of suicidal ideation and suicide plan among people with schizophrenia: a meta-analysis and systematic review of epidemiological surveys. Transl Psychiatry. 2021;11(11):552.
- Olfson M, Stroup TS, Huang C, et al. Suicide risk in Medicare patients with schizophrenia across the life span. JAMA Psychiatry. 2021;78(8):876- 885.
- Girdler SJ, Confino JE, Woesner ME. Exercise as a treatment for schizophrenia: a review. Psychopharmacol Bull. 2019;49(1):56-69.
- SMI Adviser. Schizophrenia. https://smiadviser.org/wp-content/uploads/2020/08/SMI_NAMI_Schizophrenia.pdf. Accessed April 4, 2024.
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition, Text Revision (DSM-5-TR). Washington, DC; American Psychiatric Association Publishing; 2022.
- Keepers GA, Fochtmann LJ, Anzia JM, et al. The American Psychiatric Association Practice Guideline for the Treatment of Patients With Schizophrenia. Am J Psychiatry. 2020;177(9):868-872.
- Hill MD, Gill SS, Le-Niculescu H, et al. Precision medicine for psychotic disorders: objective assessment, risk prediction, and pharmacogenomics. Mol Psychiatry. 2024 Feb 8. Epub ahead of print.
- Wu TY, Tien N, Lin CL, et al. Influence of antipsychotic medications on hyperlipidemia risk in patients with schizophrenia: evidence from a population-based cohort study and in vitro hepatic lipid homeostasis gene expression. Front Med (Lausanne). 2023;10:1137977.
- Schmitt A, Maurus I, Rossner MJ, et al. Effects of aerobic exercise on metabolic syndrome, cardiorespiratory fitness, and symptoms in schizophrenia include decreased mortality. Front Psychiatry. 2018;9:690.
- Stroup TS, Olfson M, Huang C, et al. Age-specific prevalence and incidence of dementia diagnoses among older US adults with schizophrenia. JAMA Psychiatry. 2021;78(6):632-641.
- El Miniawi S, Orgeta V, Stafford J. Non-affective psychotic disorders and risk of dementia: a systematic review and meta-analysis. Psychol Med. 2022;52(15):1-13.
- Olfson M, Gerhard T, Huang C, et al. Premature mortality among adults with schizophrenia in the United States. JAMA Psychiatry. 2015;72(12):1172-1181.
- National Institute of Mental Health. Recovery After an Initial Schizophrenia Episode (RAISE). www.nimh.nih.gov/research/research-funded-by-nimh/research-initiatives/recovery-after-an-initial-schizophrenia-episode-raise. Accessed April 4, 2024.
- Fochtmann LJ, Medicus J, Hong SH. Performance in practice: practice assessment tool for the care of patients with schizophrenia. Focus (Am Psychiatr Publ). 2020;18(4):402-423.
- Zhang JP, Gallego JA, Robinson DG, et al. Efficacy and safety of individual second-generation vs. first-generation antipsychotics in first-episode psychosis: a systematic review and meta-analysis. Int J Neuropsychopharmacol. 2013;16(6):1205-1218.
- Leucht S, Cipriani A, Spineli L, et al. Comparative efficacy and tolerability of 15 antipsychotic drugs in schizophrenia: a multiple-treatments meta-analysis. Lancet. 2013;382(9896):951-962.
- Mucci A, Kawohl W, Maria C, Wooller A. Treating schizophrenia: open conversations and stronger relationships through psychoeducation and shared decision-making. Front Psychiatry. 2020;11:761.
- Fitzgerald HM, Shepherd J, Bailey H, et al. Treatment goals in schizophrenia: a real-world survey of patients, psychiatrists, and caregivers in the United States, with an analysis of current treatment (long-acting injectable vs oral antipsychotics) and goal selection. Neuropsychiatr Dis Treat. 2021;17:3215-3228.
- Fabrazzo M, Cipolla S, Camerlengo A, et al. Second-generation antipsychotics' effectiveness and tolerability: a review of real-world studies in patients with schizophrenia and related disorders. J Clin Med. 2022;11(15):4530.
- Abou-Setta AM, Mousavi SS, Spooner C, et al. First-Generation Versus Second-Generation Antipsychotics in Adults: Comparative Effectiveness [Internet]. Rockville, MD: Agency for Healthcare Research and Quality (US); 2012 (Comparative Effectiveness Reviews, No. 63).
- Chokhawala K, Stevens L. Antipsychotic medications. In: StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing; 2024 Jan-.
- Zubair UB, Ali SA, Taj R, Batool SM. Comparison of effectiveness of antipsychotics in schizophrenia: second-generation versus the first generation. J Ayub Med Coll Abbottabad. 2020;32(1):24-27.
- Jibson MD. First-generation antipsychotic medications: pharmacology, administration, and comparative side effects. UpToDate. www.uptodate.com/contents/first-generation-antipsychotic-medications-pharmacology-administration-and-comparative-side-effects#H272233773. Accessed February 28, 2024.
- Jibson M. Second-generation antipsychotic medications: pharmacology, administration, and side effects. UpToDate. www.uptodate.com/contents/second-generation-antipsychotic-medications-pharmacology-administration-and-side-effects#H191680213. Accessed February 28, 2024.
- Kane JM, Agid O, Baldwin ML, et al. Clinical guidance on the identification and management of treatment-resistant schizophrenia. J Clin Psychiatry. 2019;80(2):18com12123.
- Parkes S, Mantell B, Oloyede E, Blackman G. Patients' experiences of clozapine for treatment-resistant schizophrenia: a systematic review. Schizophr Bull Open. 2022;3(1):sgac042.
- Mørup MF, Kymes SM, Oudin Åström D. A modelling approach to estimate the prevalence of treatment-resistant schizophrenia in the United States. PLoS One. 2020;15(6):e0234121.
- Nucifora FC Jr, Woznica E, Lee BJ, et al. Treatment resistant schizophrenia: clinical, biological, and therapeutic perspectives. Neurobiol Dis. 2019;131:104257.
- Elkis H, Buckley PF. Treatment-resistant schizophrenia. Psychiatr Clin North Am. 2016;39(2):239-265.
- Fenton C, Kang C. Clozapine is the approved option in treatment-resistant schizophrenia and requires careful management. Drugs Ther Perspect. 2023;39(3):107-113.
- Kantrowitz JT, Correll CU, Jain R, Cutler AJ. New developments in the treatment of schizophrenia: an expert roundtable. Int J Neuropsychopharmacol. 2023;26(5):322-330.
- Thaman P, Kulig CE, Greer D. Efficacy of long-acting injectable antipsychotics versus oral antipsychotics in preventing psychiatric rehospitalizations. J Clin Psychopharmacol. 2024;44(2):96-99.
- Lauriello J. Schizophrenia in adults: pharmacotherapy with long- acting injectable antipsychotic medication. UptoDate. www.uptodate.com/contents/schizophrenia-in-adults-pharmacotherapy-with-long-acting-injectable-antipsychotic-medication. Accessed April 4, 2024.
- Brooks M. FDA clears first transdermal patch for schizophrenia. Medscape. www.medscape.com/viewarticle/919887. Accessed January 30, 2024.
- Potkin SG, Kunovac J, Silverman BL, et al. Efficacy and safety of a combination of olanzapine and samidorphan in adult patients with an acute exacerbation of schizophrenia: outcomes from the randomized, phase 3 ENLIGHTEN-1 study. J Clin Psychiatry. 2020;81(2):19m12769.
- Uzedy (risperidone) product information. Parsippany, NJ: Teva Neuroscience, Inc; May 2023.
- Otsuka. FDA approves Otsuka and Lundbeck's ABILIFY ASIMTUFII® (aripiprazole), the first once-every-two-months long-acting injectable (LAI) for the treatment of schizophrenia or maintenance monotherapy treatment of bipolar I disorder in adults. https://otsuka-us.com/news/fda-approves-otsuka-and-lundbecks-abilify-asimtufiir-aripiprazole-first-once-every-two-months. Accessed April 4, 2024.
- Karuna Therapeutics. Karuna Therapeutics announces U.S. Food and Drug Administration accepts New Drug Application for KarXT for the treatment of schizophrenia. https://investors.karunatx.com/news-releases/news-release-details/karuna-therapeutics-announces-us-food-and-drug-administration. Accessed April 4, 2024.
- Leijala J, Kampman O, Suvisaari J, Eskelinen S. Daily functioning and symptom factors contributing to attitudes toward antipsychotic treatment and treatment adherence in outpatients with schizophrenia spectrum disorders. BMC Psychiatry. 2021;21(37).
- Valenstein M, Blow FC, Copeland LA, et al. Poor antipsychotic adherence among patients with schizophrenia: medication and patient factors. Schizophr Bull. 2004;30(2):255-264.
- Lieslehto J, Tiihonen J, Lähteenvuo M, et al. Primary nonadherence to antipsychotic treatment among persons with schizophrenia. Schizophr Bull. 2022;48(3):655-663.
- Vega D, Acosta FJ, Saavedra P. Nonadherence after hospital discharge in patients with schizophrenia or schizoaffective disorder: a six-month naturalistic follow-up study. Compr Psychiatry. 2021;108:152240.
- Bowtell M, Eaton S, Thien K, et al. Rates and predictors of relapse following discontinuation of antipsychotic medication after a first episode of psychosis. Schizophr Res. 2018;195:231-236.
- Cassidy RM, Yang F, Kapczinski F, Passos IC. Risk factors for suicidality in patients with schizophrenia: a systematic review, meta-analysis, and meta-regression of 96 studies. Schizophr Bull. 2018;44(4):787-797.
- Kishi T, Ikuta T, Matsui Y, et al. Effect of discontinuation v. maintenance of antipsychotic medication on relapse rates in patients with remitted/stable first-episode psychosis: a meta-analysis. Psychol Med. 2019;49(5):772-779.
- García S, Martínez-Cengotitabengoa M, López-Zurbano S, Zorrilla I, et al. Adherence to antipsychotic medication in bipolar disorder and schizophrenic patients: a systematic review. J Clin Psychopharmacol. 2016;36(4):355-371.
- Guo J, Lv X, Liu Y, et al. Influencing factors of medication adherence in schizophrenic patients: a meta-analysis. Schizophr (Heidelb). 2023;9(1):31.
- Martins R, Kadakia A, Williams GR, et al. The lifetime burden of schizophrenia as estimated by a government-centric fiscal analytic framework. J Clin Psychiatry. 2023;84(5):22m14746.
- Lin D, Kim H, Wada K, et al. Unemployment, homelessness, and other societal outcomes in patients with schizophrenia: a real-world retrospective cohort study of the United States Veterans Health Administration database. BMC Psychiatry. 2022;22(1):458.
- Mohiuddin AK. Psychiatric pharmacy: new role of pharmacists in mental health. J Psychiatry Mental Disord. 2019;4(1):1010.
- Eaves S, Gonzalvo J, Hamm JA, et al. The evolving role of the pharmacist for individuals with serious mental illness. J Am Pharm Assoc (2003). 2020;60(5S):s11-s14.
- Ceraso A, Lin JJ, Schneider-Thoma J, et al. Maintenance treatment with antipsychotic drugs in schizophrenia: a Cochrane systematic review and meta-analysis. Schizophr Bull. 2022;48(4):738-740.