An Epidemic of Opioid Use and Infectious Disease
RELEASE DATE:
April 1, 2019
EXPIRATION DATE:
April 30, 2021
FACULTY:
Natasha Colvin, PharmD, BCACP
Assistant Professor of Pharmacy Practice
(at time of writing)
South University School of Pharmacy,
Columbia, South Carolina
Clinical Pharmacist (currently)
St. James-Santee Family Health Center
Georgetown, South Carolina
Danielle Thompson, PharmD Candidate 2019
South University School of Pharmacy,
Columbia, South Carolina
Eric Newman, MA
Professional Mentor
Friends of the Children,
Charlotte, North Carolina
FACULTY DISCLOSURE STATEMENTS
Dr. Colvin, Ms. Thompson, and Mr. Newman have no actual or potential conflicts of interest in relation to this activity.
Postgraduate Healthcare Education, LLC does not view the existence of relationships as an implication of bias or that the value of the material is decreased. The content of the activity was planned to be balanced, objective, and scientifically rigorous. Occasionally, authors may express opinions that represent their own viewpoint. Conclusions drawn by participants should be derived from objective analysis of scientific data.
ACCREDITATION STATEMENT:
Pharmacy
 Postgraduate Healthcare Education, LLC is accredited by the Accreditation Council for Pharmacy Education as a provider of continuing pharmacy education.
Postgraduate Healthcare Education, LLC is accredited by the Accreditation Council for Pharmacy Education as a provider of continuing pharmacy education.
UAN: 0430-0000-19-022-H01-P
Credits: 2.0 hours (0.20 ceu)
Type of Activity: Knowledge
TARGET AUDIENCE:
This accredited activity is targeted to pharmacists. Estimated time to complete this activity is 120 minutes.
Exam processing and other inquiries to:
CE Customer Service: (800) 825-4696 or cecustomerservice@powerpak.com
DISCLAIMER:
Participants have an implied responsibility to use the newly acquired information to enhance patient outcomes and their own professional development. The information presented in this activity is not meant to serve as a guideline for patient management. Any procedures, medications, or other courses of diagnosis or treatment discussed or suggested in this activity should not be used by clinicians without evaluation of their patients' conditions and possible contraindications or dangers in use, review of any applicable manufacturer's product information, and comparison with recommendations of other authorities.
GOAL:
To provide participants with an overview of the opioid crisis, including its link to opioid use disorder and rising numbers of infectious-disease cases, and to review screening and preventive measures that may be taken by pharmacists and other healthcare professionals.
OBJECTIVES:
After completing this activity, the participant should be able to:
- Describe opioid use disorder and its contribution to the current opioid crisis.
- Identify clinical manifestations that have been linked to the current opioid crisis.
- Recall specific medical conditions and infectious diseases that may result from opioid use disorder.
- Restate effective screening and preventive measures to reduce the incidence of infectious diseases due to opioid use disorder.
ABSTRACT: Historically, there have been a limited number of options for pain management. The discovery of opiates and their pain-relieving properties prompted their introduction into the medical community. Widespread use and a lack of education regarding prescriptive practices have contributed to the current epidemics of opioid use and infectious diseases. Reported cases of HIV, hepatitis, sexually transmitted diseases, infective endocarditis, septic arthritis, skin abscess, and osteomyelitis have increased significantly since the surge of opioid use in the United States. It is important for healthcare professionals to gain awareness about opioid use disorder (OUD) and ensure that opioids are being used appropriately and responsibly. Countermeasures such as prescription drug monitoring programs and patient treatment agreements may help combat the issue. To be cognizant of OUDs' clinical manifestations, health consequences, and screening/preventive measures is to be proactive in the fight to end the opioid crisis.
The opioid crisis has surged exponentially throughout the United States over the past several years. In 2017, approximately 72,000 Americans died from opioid overdose, according to preliminary estimates from the CDC.1
At the same time, persons who inject drugs (PWID) are being impacted by increasing infectious-disease transmission that is likely facilitated by contaminated needles, unprotected sex, homelessness, lack of access to medical care, and other socioeconomic factors.1,2 The number of cases of hepatitis A, B, and C, and sexually transmitted diseases (STDs), including HIV, have escalated with the growing opioid crisis.2 According to the CDC, between August 2016 and March 2018 the number of hepatitis A cases almost doubled compared with the previous 2 years, and between 2009 and 2016, hepatitis C cases nearly quadrupled.2 Since 2015, several localized outbreaks of HIV contracted through injection-drug use have been identified, resulting in the CDC recognizing 220 counties at particular risk.
Early diagnosis of infectious disease is crucial to getting patients treated appropriately and preventing further transmission. To help prevent outbreaks, it has been suggested that drug rehabilitation and treatment facilities can offer infectious-disease testing, thereby playing a vital role in identifying and interrupting transmission.1 The integration of skills and expertise from various healthcare professionals, including pharmacists, may aid in combating and resolving the U.S. opioid crisis and its infectious-disease consequences by way of screening for these diseases or recommending initiation of effective FDA-approved medications.
THE OPIOID CRISIS
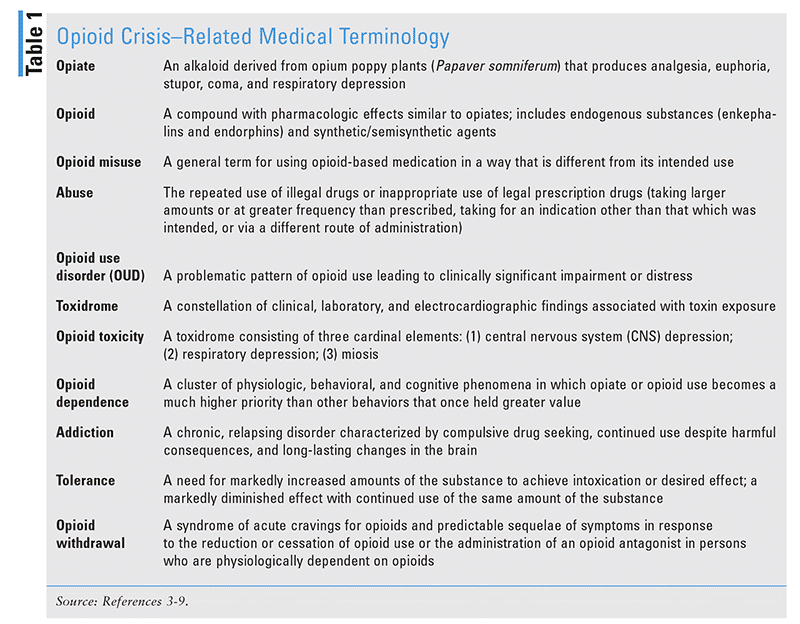
To better understand the opioid crisis and its impact, it is important to understand the related terminology (TABLE 1).3-9
Statistics compiled by the National Institute on Drug Abuse show that roughly 21% to 29% of patients prescribed opioids for chronic pain misuse them; 8% to 12% develop opioid use disorder (OUD); 4% to 6% transition to heroin; and 80% of people who used heroin first misused prescription opioids.10 The opioid crisis had its beginnings as early as the mid-1800s when there were very few options available for pain management.11 Opium tincture and morphine were viewed by patients and providers as magical potions to treat health problems as varied as diarrhea, painful injuries, and hangovers. The sale of morphine was not well controlled, allowing many people to acquire and inject the drug.11 With improved physician education, use of morphine had diminished by the early 20th century.11
Oxycontin, an extended-release formulation of oxycodone, was introduced in 1995.11 Subsequently, opioid prescribing increased, as did widespread diversion, medication misuse, and overdoses—currently the leading cause of death among Americans younger than age 50 years.10-12 As of early 2019, estimates are that more than 130 Americans die each day from opioid overdose, and nearly 2 million suffer from substance use disorders related to prescription opioids.10 The Department of Health and Human Services has declared the situation a public health crisis.10
OPIOID USE DISORDER
OUD is a problematic pattern of opioid use leading to clinically significant impairment or distress.5 It can involve misuse of prescribed opioid medications, use of diverted opioid medications, or use of illicitly obtained heroin.13
The International Classification of Diseases, 10th Revision, describes criteria that may be used to classify signs of opioid dependence.14 The Diagnostic and Statistical Manual of Mental Disorders, (Fifth Edition; DSM-5) is used to diagnose and determine the severity of OUD (mild: 2-3 symptoms; moderate: 4-5 symptoms; or severe: 6 or more symptoms). In order to confirm a diagnosis, at least two of the following should be observed within a 12-month period 15:
- Opioids are often taken in larger amounts or over a longer period than was intended.
- There is a persistent desire or there are unsuccessful efforts to cut down or control opioid use.
- A great deal of time is spent in activities necessary to obtain the opioid, use the opioid, or recover from its effects.
- Craving, or a strong desire or urge to use opioids, occurs.
- Recurrent opioid use results in a failure to fulfill major role obligations at work, school, or home.
- Opioid use continues despite having persistent or recurrent social or interpersonal problems caused or exacerbated by the effects of opioids.
- Important social, occupational, or recreational activities are given up or reduced because of opioid use.
- Opioid use recurs in situations in which it is physically hazardous.
- Opioid use continues despite knowledge of having a persistent or recurrent physical or psychological problem that is likely to have been caused or exacerbated by the substance.
- User exhibits tolerance.
- User exhibits withdrawal.
Typically, OUD is a chronic, relapsing illness that can lead to significant morbidity and mortality if not appropriately treated. Options for long-term maintenance therapy include an opioid agonist (i.e., methadone or buprenorphine); an opioid antagonist (naltrexone); or abstinence-based treatment.13 In an attempt to prevent clinical manifestations and relapse, it is important to initiate appropriate maintenance therapy.
CLINICAL MANIFESTATIONS
It is vital for pharmacists and other healthcare professionals (HCPs) to be cognizant of the hallmark signs of acute opioid intoxication as well as symptoms of opioid withdrawal, both of which can evolve into emergent situations that may necessitate immediate action. Patients may present with physical or psychological signs/symptoms of acute opioid intoxication or withdrawal; however, it is possible for patients who have developed a tolerance to appear asymptomatic at initial presentation.13
Persons experiencing opioid intoxication may present with the following physical characteristics16:
- Skin irritation/rash (possibly indicative of opioid-induced histamine release)
- Piloerection
- Flushing
- Diaphoresis
- Track marks/pock marks
- Cellulitis
- Pitting edema
- Ptosis
- Conjunctivitis
- Epistaxis
- Miosis
- Nasal septum excoriation or perforation
- Nodding head
- Jaundice
- Oral abscesses
- Orthostatic hypotension
- Bradycardia
Organ systems may be affected as well, including the circulatory system (murmur or arrrythmia); respiratory (decreased respiratory rate, asthma, dyspnea, rales, chronic cough); digestive (constipation); and nervous system (euphoria, dysphoria, drowsiness, slurred speech, impaired concentration or judgment).16
Signs specific to opioid withdrawal include tachycardia, elevated blood pressure, restlessness, agitation, tremor, yawning, piloerection, diaphoresis, lacrimation, mydriasis, delirium, increased bowel sounds, and seizures.17
Patients who exhibit mild symptoms of OUD usually have normal social functioning and may require detailed interviewing and evaluation to elucidate any existing drug use, whereas patients who have severe OUD may have a social history remarkable for illegal drug-seeking behaviors including burglary, shoplifting, or prostitution. They may also forfeit personal hygiene, work, and relationships as addiction and physical and psychological dependence on opioids increases.13 Eventually, patients with OUD may engage in risky behaviors that increase the likelihood of exposure to, and the incidence of, infectious diseases.13
INFECTIOUS DISEASE CONSEQUENCES
The ongoing opioid epidemic in the U.S. has heightened the concern as to how misuse of opioids, whether via oral use, insufflation, or injection, might fuel transmission of infectious diseases.18,19 It is reported that an estimated 10% to 20% of people who abuse prescription opioids eventually move on to inject either prescription opioids or heroin and thereby increase their risk of developing infections such as HIV, hepatitis, STDs, infective endocarditis (IE), septic arthritis, skin abscess, and osteomyelitis.12,13,20
HIV
In comparison with the general population, the likelihood of contracting HIV is significantly higher in substance abusers by way of direct exposure to contaminated needles or high-risk behavior.20 HIV is an infectious disease that destroys the CD4+ cells that are responsible for assisting the immune system in combating common diseases and infections.21 In people living with HIV, substance use can hasten disease progression, affect adherence to antiretroviral therapy, and worsen their overall prognosis.21 Data show that approximately 15% of HIV-infected persons in the U.S. remain unaware of their HIV infection, leading to significant morbidity and the risk of further transmission.22
Without proper preventive treatment, an HIV-infected individual's CD4+ cell count may drop, placing them at increased risk of opportunistic infections such as Pneumocystic jirovecii pneumonia (PCP), Toxoplasma encephalitis (TE), and Mycobacterium avium complex (MAC) (TABLE 2).23
Hepatitis A, B, and C
The opioid crisis is also allowing hepatitis (especially hepatitis C), an infection that causes inflammation of the liver, to gain a foothold among a new generation of Americans at an alarming rate. The CDC reports that injection-drug use–related hepatitis C infection rates increased 350% between 2010 and 2016, killing approximately 20,000 people annually.1,2
Hepatitis A is a vaccine-preventable virus usually transmitted through fecal matter.2 It is most commonly seen among adults experiencing homelessness.24
Hepatitis B is a vaccine-preventable virus usually spread through bodily fluids such as blood or semen. It is most commonly seen among individuals who use needles.2 Progress on the prevention of hepatitis B has stalled in many areas of the country because of increasing infections among unvaccinated individuals over age 30 years.25
Hepatitis C, the more common of the three, is a non–vaccine-preventable virus usually transmitted through blood. It is also commonly transmitted via needle use.2 Fortunately, there are medications to treat hepatitis C; however, PWID may not realize that they are infected, inject a drug, and pass the needle on to another person, thereby transmitting the virus.
Other Infectious Diseases
PWID who engage in risky behaviors increase their risk of other STDs including, but not limited to, syphilis, chlamydia, genital herpes, human papilloma virus, and gonorrhea.26 They may also develop these infections because of injection-site reactions or hematogenous spread. IE is typically associated with congenital heart disease and instrumentation of the heart; however, it is becoming an increasingly prevalent infectious disease among injection-drug users. The mechanism is thought to be damage to the heart valves from injected particulate matter in the setting of injected bacterial loads, with Staphylococcus aureus being the most common infective organism. The health consequences of IE include persistent fever, bacteremia, and multiple pulmonary emboli. S aureus skin abscesses may also cause bacteremia, which could allow the organism to travel to the joints and bones, causing septic arthritis and osteomyelitis.27
It is vital that all HCPs take an active role in preventing these infectious diseases; untreated OUD may result in prolonged hospital stays, frequent readmissions due to lack of adherence to antibiotic regimens or reinfection, substantial morbidity, and a heavy financial burden on the healthcare system.28
PREVENTION
Preventive measures to effectively attenuate OUD are imperative. Guidelines are available to help assist clinicians with prescribing appropriate doses of opioid medications to reduce pain. Category A recommendations from the 2016 CDC Guidelines for Prescribing Opioids for Chronic Pain suggest that prescribers establish realistic treatment goals, evaluate benefits and harms, prescribe the lowest effective dosage, and review the patient's history of controlled substance prescriptions using state prescription drug monitoring programs.29 The guidelines also recommend, albeit with a lower recommendation (Category B), drug testing of urine prior to initiating an opioid regimen and annual assessment for prescribed medications as well as other controlled prescription drugs and illicit drugs.29
The American Pain Society and the American Academy of Pain Medicine have established guidelines for patients on opioid therapy for chronic noncancer pain. These guidelines give strong recommendations for reassessing patients periodically and as warranted for pain intensity and level of functioning, progress toward therapeutic goals, adverse events, and adherence.30 The guidelines also suggest tapering down or weaning off chronic opioid therapy if patients experience repeated aberrant drug-related behaviors or drug abuse or diversion, no progress toward goals, or intolerable adverse effects.30
Additional prevention strategies include treatment agreements; these are written contracts on pain management between physicians and patients. A standard treatment agreement may, at a minimum, hold the patient accountable for filling opioid medications at only one pharmacy; prohibit the patient from sharing or selling their medication; or obligate the patient to take random drug tests or be prepared for random pill counts, if selected.31
Use of abuse-deterrent opioid formulations, vaccinations, and/or pre-exposure prophylaxis (PrEP) for HIV are other preventive measures that may deter potential opioid abuse/misuse (i.e., snorting or injecting) and disease transmission.31,32 PrEP is a course of antiretroviral drugs taken once daily to help prevent an HIV-negative person from contracting the virus from a sexual or injection-drug–using partner who is positive. It is a combination pill comprised of two HIV medications, tenofovir and emtricitabine. The World Health Organization recommended PrEP for PWID in 2015 because it has been shown to reduce the risk of HIV transmission by more than 70% in this population when used consistently as prescribed.32
These preventive measures are effective; however, there are certain barriers that hinder prevention efforts, such as the willingness of patients with OUD or who use illicit drugs to seek much-needed treatment. Barriers also include homelessness, unemployment, poverty, fear of arrest, and stigma.33 Depending on the pharmacy-practice setting, pharmacists may be able to build rapport with patients as well as identify clinical manifestations of OUD. Once a level of trust is gained, patients with OUD may be more apt to admit to drug abuse/misuse and pursue appropriate pharmacist intervention or treatment measures, if needed.
SCREENING AND ASSESSMENT
Identifying patients with the potential for aberrant opioid use is critical. These individuals are at an increased risk for infectious diseases, potential drug interactions, eventual precipitation of withdrawal, and adverse effects commonly associated with opioid-containing products.34 Screening for opioid abuse primarily consists of assessment for history of past and current substance abuse, risk-factor stratification, and use of opioid-assessment screening tools.35
There are certain risk factors associated with increased likelihood of opioid misuse/abuse. Identifying these risk factors can aid in determining if additional measures such as screening tools and assessments or laboratory tests should be conducted.
Risk factors include but are not limited to35:
- Prior history of substance use disorder
- Demographic features (i.e., younger age)
- Patients who report more subjective pain, multiple pain complaints, and/or a greater degree of pain-related limitations
- Co-occurring mental disorders (i.e., history of mood disorder, psychological problems, or psychosocial stressors)
Urine is the most common biological fluid used in drug screening. Opioid metabolites can be detected in chronic users 24 to 72 hours following the last dose on standard urine drug screens.36 However, it is important to note that urine drug tests are not definitive and false-positive or false-negative results may occur.34 Adulteration to urine specimens is possible owing to privacy during the collection process.37 Opioids can also be detected in other biological samples such as serum, saliva, sweat, or hair.
The Substance Abuse and Mental Health Services Administration's Treatment Improvement Protocol (TIP) Part 2: Addressing Opioid Use Disorder in General Medical Settings recommends patients with OUD undergo laboratory testing because of increased risk for liver disease and blood-borne viral infections.34 Laboratory testing, per TIP recommendations, includes pregnancy testing, liver-function tests, HIV serology, and hepatitis B and C serologies. Additionally, serologic testing for syphilis, a complete blood count, and purified protein derivative testing should be performed in PWID. Appropriate patient counseling should also be used as an adjunct to laboratory testing.36
Screening assessments varying in administration time, validity (as defined by sensitivity and specificity), reliability, and content are available for use in patients with potential OUD. One example is the Screener and Opioid Assessment for Patients with Pain, a 14-item screening tool that uses a 5-point Likert scale; it was created as a brief self-report measure to identify patients at risk for problems with long-term opioid medication use.38 The Rapid Opioid Dependence Screen is an 8-question screening tool based on DSM-IV criteria that uses binary (yes/no) responses and takes 2 minutes or less to administer.39 Wickersham and colleagues, in a 2015 article, reported the Structured Clinical Interview for DSM Disorders (SCID) as the gold-standard screening tool. The SCID consists of more that 500 questions, based on DSM-IV criteria, uses binary responses, and takes an average of 30 minutes to administer.39
When properly used, screening tools provide HCPs with an objective assessment to evaluate patients who may have, or be at risk for, OUD. Along with recognizing risks and using laboratory values, these screening tools are invaluable for the assessment and detection of opioid abuse/misuse and serve to aid HCPs in better caring for at-risk patients.
CONCLUSION
The opioid crisis is associated with many untoward effects, including an increase in the incidence of infectious diseases. Measures should be in place to prevent aberrant drug use, such as appropriate prescribing and counseling for opioids, regular use of prescription monitoring programs, dispensing abuse-deterrent formulations, and using screening tools/laboratory testing as necessary. Additionally, patients with high abuse potential should be immunized for vaccine-preventable diseases and/or receive PrEP treatment if engaging in risky behaviors (i.e., needle sharing or unprotected sex). Though prevention is preferable, treatment modalities should include providing patients at risk for overdose with reversal agents such as naloxone. Partial or full opioid agonists such as buprenorphine or methadone, respectively, may be used to effectively wean patients with less risk of precipitating a withdrawal. As potentially the first-line HCP contact with individuals at risk for opioid abuse/misuse, pharmacists must be vigilant in their efforts to combat OUD and its detrimental consequences.
REFERENCES
- Sayas A, McKay S, Honermann B, et al. Despite infectious disease outbreaks linked to opioid crisis, most substance abuse facilities don't test for HIV or HCV. www.healthaffairs.org/do/10.1377/hblog20181002.180675/full/. Accessed November 30, 2018.
- Vaida B. Infectious disease outbreaks rise with opioid epidemic. https://healthjournalism.org/blog/2018/08/infectious-disease-outbreaks-rise-with-opioid-epidemic/. Accessed November 30, 2018.
- Opioid abuse and dependence. Terminology. DynaMed Plus. Ipswich, MA: EBSCO Information Services. www.dynamed.com. Accessed December 17, 2018.
- Opioid withdrawal. Terminology. DynaMed Plus. Ipswich, MA. EBSCO Information Services. www.dynamed.com. Accessed December 17, 2018.
- CDC. Module 5: Assessing and addressing opioid use disorder (OUD). www.cdc.gov/drugoverdose/training/oud/accessible/index. html. Accessed December 18, 2018.
- Toxidromes. Background. DynaMed Plus. Ipswich, MA: EBSCO Information Services. www.dynamed.com. Accessed January 15, 2019.
- Opioid toxicity. Critical points. DynaMed Plus. Ipswich, MA: EBSCO Information Services. www.dynamed.com. December 17, 2018.
- Community management of opioid overdose. Geneva: World Health Organization; 2014. Glossary of terms used in these guidelines. www.ncbi.nlm.nih.gov/books/NBK264299/. Accessed December 20, 2018.
- The science of drug use and addiction: the basics. National Institute on Drug Abuse website. Updated July 2018. www.drugabuse.gov/publications/media-guide/science-drug-use-addictionbasics. Accessed December 26, 2018.
- Opioid overdose crisis. www.drugabuse.gov/drugs-abuse/opioids/opioid-overdose-crisis. Accessed March 22, 2019.
- Kolodny A. Courtwright DT, Hwang CS. The prescription opioid and heroin crisis: a public health approach to an epidemic of addiction. Annu Rev Public Health. 2015;36:559-574.
- HIV.gov. Hidden casualties: consequences of opioid epidemic on the spread of infectious diseases. U.S. Department of Health and Human Services. www.hiv.gov/blog/hidden-casualties-consequences-opioid-epidemic-spread-infectious-diseases. Accessed November 30, 2018.
- Strain E. Opioid use disorder: epidemiology, pharmacology, clinical manifestations, course, screening, assessment, and diagnosis. www.uptodate.com/contents/opioid-use-disorder-epidemiology-pharmacology-clinical-manifestations-course-screening-assessment-and-diagnosis. Accessed January 15, 2019.
- Opioid abuse and dependence. Diagnosis. DynaMed Plus. Ipswich, MA: EBSCO Information Services. www.dynamed.com. Accessed December 21, 2018.
- Opioid use disorder: What is opioid addiction? Providers Clinical Support System. https://pcssnow.org/resource/opioid-usedisorder-opioid-addiction/. Accessed January 15, 2019.
- Opioid abuse and dependence. Physical. DynaMed Plus. Ipswich, MA: EBSCO Information Services. www.dynamed.com. Accessed January 2, 2019.
- Opioid withdrawal. Physical. DynaMed Plus. Ipswich, MA: EBSCO Information Services: www.dynamed.com. Accessed January 2, 2019.
- Substance Abuse and Mental Health Services Administration. 2016 National Survey on Drug Use and Health. www.samhsa.gov/ data/sites/defaut/files/NSDUH-FFR1-2016/NSDUH-FFR1-2016. pdf. Accessed January 9, 2019.
- Peters PJ, Pontones P, Hoover KW, et al. HIV infection linked to injection use of oxymorphone in Indiana, 2014-2015. N Engl J Med. 2016;375:229-239.
- Van Handle MM, Rose CE, Hallisey EJ, et al. County-level vulnerability assessment for rapid dissemination of HIV or HCV infections among persons who inject drugs, United States. J Acquir Immune Defic Syndr. 2016;73(3):323-331.
- CDC. About HIV/AIDS. www.cdc.gov/hiv/basics/whatishiv. html. Accessed March 6, 2019.
- Sax P. Screening and diagnostic testing for HIV infection. www. uptodate.com/contents/screening-and-diagnostic-testing-for-hiv-infecti on?topicRef=7804&source=see_link. Accessed December 4, 2018.
- Guidelines for prevention and treatment of opportunistic infections in HIV-infected adults and adolescents. https://aidsinfo. nih.gov/contentfiles/lvguidelines/AdultOITablesOnly.pdf. Accessed March 6, 2019.
- Parry N. Infectious diseases on the rise amid the opioid epidemic. ContagionLive.com. www.contagionlive.com/news/infectious-diseases-on-the-rise-amid-the-opioid-epidemic. Accessed November 30, 2018.
- Wolitski R, Dan C. Three medical societies identify specific infections of concern in relation to the opioid crisis. www.hhs.gov/hepatitis/blog/2018/06/13/experts-link-opioid-crisis-and-infectious-diseases.html. Accessed November 30, 2018.
- HIV.gov.What do you need to know about STDs? U.S. Department of Health and Human Services. www.hiv.gov/hivbasics/staying-in-hiv-care/other-related-health-issues/sexuallytransmitted-diseases. Accessed March 6, 2019.
- Moss R, Munt B. Injection drug use and right sided endocarditis. Heart. 2003;89(5):577-581.
- Springer S, Korthuis P, Rio C. Integrating treatment at the intersection of opioid use disorder and infectious disease epidemics in medical settings: a call for action after a national academies of sciences, engineering, and medicine workshop. http://annals.org/aim/fullarticle/2687952/integrating-treatment-intersection-opioid-use-disorder-infectious-disease-epidemics-medical. Accessed November 30, 2018.
- Dowell D, Haegerich T, Chou R. CDC Guideline for prescribing opioids for chronic pain. United States, 2016. MMWR Recomm Rep. 65(1):1-49.
- Chou R, Fanciullo GJ, Fine, PG, et al. American Pain Society American Academy of Pain Medicine Opioids Guidelines Panel. Clinical guidelines for the use of chronic opioid therapy in chronic non-cancer pain. 2009;10(2):113-130.
- FDA. Abuse-deterrent opioid analgesics. Updated April 23, 2018. www.fda.gov/Drugs/DrugSafety/PostmarketDrugSafetyInformationfor PatientsandProviders/ucm600788.htm. Accessed January 9, 2019.
- CDC. PrEP. www.cdc.gov/hiv/basics/prep.html. Accessed March 6, 2019.
- CDC. HIV and substance use in the United States. www.cdc. gov/hiv/risk/substanceuse.html. Accessed January 9, 2019.
- Substance Abuse and Mental Health Services Administration. TIP 63 Part 2: Addressing opioid use disorder in general medical settings. https://store.samhsa.gov/system/files/sma18-5063pt2.pdf. Accessed January 13, 2019.
- Kaye AD, Jones MR, Kaye AM, et al. Prescription opioid abuse in chronic pain: an updated review of opioid abuse predictors and strategies to curb opioid abuse: part 1. Pain Physician. 2017;20 (2S):S93-S109.
- Strain E. Opioid use disorder: epidemiology, pharmacology, clinical manifestations, course, screening, assessment and diagnosis. Laboratory evaluation. www.uptodate.com/contents/opioiduse-disorder-epidemiology-pharmacology-clinical-manifestations course-screening-assessment-and-diagnosis#H546649335. Accessed December 30, 2018.
- Opioid abuse and dependence. Testing overview. DynaMed Plus. Ipswich, MA: EBSCO Information Services. http://www. dynamed.com. Accessed January 10, 2019.
- Akbik H, Butler SF, Budman SH, et al. Validation and clinical application of the Screener and Opioid Assessment for Patients with Pain (SOAPP). J Pain Symptom Manag. 2006;32:287-293.
- Wickersham J, Azar M, Cannon C, et al. Validation of a brief measure of opioid dependence: the Rapid Opioid Dependence Screen (RODS). J Correct Health Care. 2015;21(1):12-26.