Medication Adherence in Patients With Type 2 Diabetes
RELEASE DATE:
June 5, 2019
EXPIRATION DATE:
June 30, 2021
FACULTY:
Erin K. Hennessey, PharmD, BCPS
Assistant Professor of Pharmacy Practice
St. Louis College of Pharmacy
Clinical Pharmacy Specialist, Internal/Family Medicine
Mercy Hospital St. Louis
St. Louis, Missouri
Golden L. Peters, PharmD, BCPS
Associate Professor of Pharmacy Practice
St. Louis College of Pharmacy
Clinical Pharmacy Specialist, Primary Care
Veterans Affairs St. Louis Health Care System, John Cochran Division
St. Louis, Missouri
FACULTY DISCLOSURE STATEMENTS
Dr. Hennessey and Dr. Peters have no actual or potential conflicts of interest in relation to this activity.
Postgraduate Healthcare Education, LLC does not view the existence of relationships as an implication of bias or that the value of the material is decreased. The content of the activity was planned to be balanced, objective, and scientifically rigorous. Occasionally, authors may express opinions that represent their own viewpoint. Conclusions drawn by participants should be derived from objective analysis of scientific data.
ACCREDITATION STATEMENT:
Pharmacy
 Postgraduate Healthcare Education, LLC is accredited by the Accreditation Council for Pharmacy Education as a provider of continuing pharmacy education.
Postgraduate Healthcare Education, LLC is accredited by the Accreditation Council for Pharmacy Education as a provider of continuing pharmacy education.
UAN: 0430-0000-19-048-H01-P
Credits: 2.0 hours (0.20 ceu)
Type of Activity: Knowledge
TARGET AUDIENCE:
This accredited activity is targeted to pharmacists. Estimated time to complete this activity is 120 minutes.
Exam processing and other inquiries to:
CE Customer Service: (800) 825-4696 or cecustomerservice@powerpak.com
DISCLAIMER:
Participants have an implied responsibility to use the newly acquired information to enhance patient outcomes and their own professional development. The information presented in this activity is not meant to serve as a guideline for patient management. Any procedures, medications, or other courses of diagnosis or treatment discussed or suggested in this activity should not be used by clinicians without evaluation of their patients' conditions and possible contraindications or dangers in use, review of any applicable manufacturer's product information, and comparison with recommendations of other authorities.
GOAL:
To provide pharmacists with an overview of medication adherence, including predictors, barriers, and strategies to enhance adherence in patients with type 2 diabetes.
OBJECTIVES:
After completing this activity, the participant should be able to:
- Describe the impact of medication adherence on treatment outcomes.
- Identify barriers to and predictors of poor medication adherence.
- Review strategies for promoting medication adherence.
- Discuss medication adherence in patients with type 2 diabetes.
ABSTRACT: Medication adherence is a vital aspect of type 2 diabetes management. Adherence to maintenance medications is estimated to be between 30% and 50%. The World Health Organization has identified five dimensions affecting adherence: patient-related, socioeconomic, condition-related, health system–related, and therapy-related. Solid communication skills are essential for promoting medication adherence and identifying barriers to adherence. Barriers to medication adherence are complex and varied, and strategies to promote adherence must be calculated and multidimensional. Four general categories for enhancing medication adherence have been identified: patient education, improved dosing regimens, enhanced communication between patient and provider, and increased provider availability. Extensive medication knowledge, experience with patient barriers, communication and interviewing skills, and access render the pharmacist the ideal healthcare provider to address and ensure medication adherence in patients with type 2 diabetes.
For medications to work, patients must take them as prescribed. The full benefits of medications can be achieved only if the medication regimen is followed as directed. Improving medication adherence can have a greater impact on patient outcomes than can a specific medication alone. This article will discuss adherence, predictors of poor adherence, communication, strategies to promote adherence, and the impact of clinical inertia.
Adherence rates generally are higher in patients with acute conditions than in patients who have chronic conditions.1 Medication adherence in adults with chronic conditions is estimated at between 30% and 50%.2 Approximately 20% of new prescriptions are never filled.3 In the United States, nonadherence is linked to increased morbidity and mortality, totaling 125,000 deaths and roughly 10% of hospitalizations each year.2 Medication nonadherence is estimated to cost the U.S. healthcare system $100 billion to $317 billion annually.2,3
Adherence has been defined as the collaborative, voluntary action on the part of a patient to perform a mutually acceptable behavior to achieve a therapeutic result.4 Medication adherence refers to the extent to which a patient takes his or her medications as prescribed by the healthcare provider.1 Adherence implies a union or agreement between patient and provider. The term compliance is not preferred because of the implied passive role for the patient.5 Both adherence and compliance are flawed descriptors because they overvalue the control a provider has over the medication-taking behavior of the patient.5 Persistence is the duration of time that a patient is adherent to the treatment plan.5
Scope of Nonadherence in Type 2 Diabetes
Diabetes, a complicated disease state, is inherently difficult to understand and treat. To adequately manage diabetes, most patients require complex medication, diet, and exercise regimens, a situation that can potentially result in medication-adherence issues. One in three patients with type 2 diabetes reports missing at least one dose of oral hypoglycemic medication each month, and only 60% of patients taking insulin report medication adherence.3,6 Improved medication adherence in diabetes patients was found to result in an estimated annual savings of $661 million to $1.16 billion.7,8 Nonadherence to the treatment regimen is the most important factor determining therapeutic outcomes, especially in chronic diseases such as type 2 diabetes. Overall, the management of type 2 diabetes should incorporate medication adherence and appropriate medication selection based on patient-specific information.
Barriers to Adherence and Predictors of Poor Adherence
Barriers to medication adherence can frequently be anticipated and addressed if the pharmacist knows the common roadblocks and how to address them. The World Health Organization (WHO) lists five dimensions affecting adherence: patient-related, socioeconomic, condition-related, health system–related, and therapy-related.6,9 Barriers arising from each of these dimensions can affect patients with type 2 diabetes.
According to the WHO, patient-related factors encompass a patient's resources, knowledge, beliefs, perceptions, and expectations. Patient-related factors in diabetes may vary significantly depending on the extent of both nonpharmacologic and pharmacologic lifestyle changes that must be made and maintained. Diabetes management requires not only medication adherence but also adherence to monitoring, follow-up, and self-care. Additionally, with the approval of new medications, regimens may become increasingly complex, further challenging patients' understanding. Patients' comprehension of these regimens, the benefits and risks associated with their medications, and their disease state in general may impact their prioritization of medication adherence and is a vital aspect of patient education. This concept may be particularly challenging to instill in younger patients, who may not yet realize the consequences of nonadherence.6,9
Socioeconomic factors also figure in patient adherence to diabetes medication regimens. Lower socioeconomic status, illiteracy (and low health literacy), low educational level, lack of social support (including family instability), changing living situation (e.g., homelessness), culture, and high-cost medications have been reported to affect adherence. Age may also play a role, given that more than half of all prescription drug costs are incurred by elderly patients.6,9
Condition-related factors are elements specific to a particular disease state. For patients with type 2 diabetes, these may include symptom and complication severity (e.g., cardiovascular disease), level of disability (e.g., amputation), rate of disease progression, and availability of pharmacotherapy options. The last of these factors has become much less of a barrier for diabetes patients, although socioeconomic factors may influence a patient's ability to receive particular medications. The influence of condition-related factors depends on the patient's perception of the condition-related risks of diabetes and the disease severity.6,9
Health system–related factors may include inadequate time with a provider, insurance coverage and reimbursement (or lack thereof), poor follow-up, and difficulties with medication-distribution systems (e.g., drug shortages). In the case of diabetes, a complicated drug regimen (e.g., basal-bolus insulin regimen) requires provider time to reinforce education with sufficient follow-up. Additionally, the high cost of hypoglycemic drugs often leads to patient barriers resulting from inadequate insurance coverage.6,9
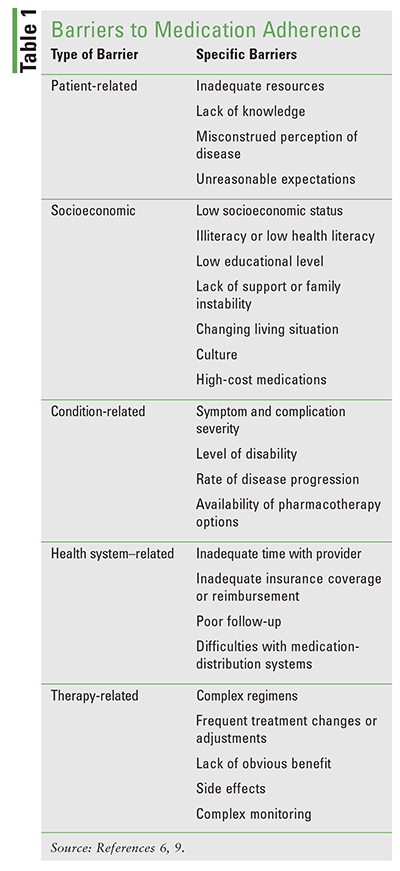 The term therapy-related factors refers to treatment modalities. Some factors include complex regimen, frequent treatment changes or adjustments, lack of obvious benefit, and side effects. All of these have significant implications for a diabetes medication regimen, especially if insulin is involved. On top of complicated medication regimens, patients may also have to deal with increasingly complex disease and glucose monitoring as their diabetes progresses. A recent systematic review and meta-analysis of 48 studies involving a total of 1,696,939 patients was conducted to compare adherence rates of hypoglycemic medications and classes.10 The following medications and classes were included: metformin, sulfonylureas (SUs), thiazolidinediones (TZDs), dipeptidyl peptidase-4 (DPP-4) inhibitors, and glucagon-like peptide-1 (GLP-1) agonists. Among studies comparing oral agents, TZDs had better mean adherence than SUs, and both had better mean adherence than metformin. Although meta-analysis could not be performed for comparison, the authors noted that in all studies comparing DPP-4 inhibitors with TZDs or SUs, adherence was better with DPP-4 inhibitors. Similarly, although meta-analysis was not performed, the authors found that adherence was better with SUs and DPP-4 inhibitors than with GLP-1 agonists in studies making these comparisons.10 Because of heterogeneity among studies and because adherence is only one component of the larger decision-making picture, results of this systematic review should be interpreted and used with caution. Barriers to medication adherence are presented in TABLE 1.6,9
The term therapy-related factors refers to treatment modalities. Some factors include complex regimen, frequent treatment changes or adjustments, lack of obvious benefit, and side effects. All of these have significant implications for a diabetes medication regimen, especially if insulin is involved. On top of complicated medication regimens, patients may also have to deal with increasingly complex disease and glucose monitoring as their diabetes progresses. A recent systematic review and meta-analysis of 48 studies involving a total of 1,696,939 patients was conducted to compare adherence rates of hypoglycemic medications and classes.10 The following medications and classes were included: metformin, sulfonylureas (SUs), thiazolidinediones (TZDs), dipeptidyl peptidase-4 (DPP-4) inhibitors, and glucagon-like peptide-1 (GLP-1) agonists. Among studies comparing oral agents, TZDs had better mean adherence than SUs, and both had better mean adherence than metformin. Although meta-analysis could not be performed for comparison, the authors noted that in all studies comparing DPP-4 inhibitors with TZDs or SUs, adherence was better with DPP-4 inhibitors. Similarly, although meta-analysis was not performed, the authors found that adherence was better with SUs and DPP-4 inhibitors than with GLP-1 agonists in studies making these comparisons.10 Because of heterogeneity among studies and because adherence is only one component of the larger decision-making picture, results of this systematic review should be interpreted and used with caution. Barriers to medication adherence are presented in TABLE 1.6,9
Communicating About Adherence
To successfully promote medication adherence and assess barriers to adherence, a solid communication skill set is required. Communication with patients about adherence necessitates pointed question-asking as well as education and support. Approaching these conversations with a specific definition of adherence is a good first step toward ensuring that the healthcare provider and the patient have a shared understanding. Some common misconceptions about adherence relate to lack of awareness of who the responsible party is (e.g., patient vs. provider), inaccurate knowledge of what constitutes ideal adherence (e.g., 80%? 100%?), attitudes about barriers, and insufficient understanding of how a medication affects the disease process. Medication adherence requires patients to understand the disease process and how their medication works, be motivated to take their medication, and implement lifestyle and behavioral changes. With all this in mind, the pharmacist can approach discussions about adherence strategically. Important steps include gathering data, establishing a cooperative relationship, engaging in open-ended questioning, actively educating, and addressing barriers.11
Data gathering may be undertaken prior to the discussion. This step is important because objective information can be identified that may help frame the conversation. Objective data include prescription refill records, measures of disease control (e.g., A1C, fasting lipid panel), and consistency in making healthcare-maintenance appointments. A formal approach to assessing refill history is to calculate a medication possession ratio (MPR). The MPR is the sum of the days' supply of fills for a drug (i.e., number of tablets/capsules of a specific drug dispensed in a specific timeframe) divided by the number of days in that timeframe. For example, if a patient taking glipizide 5 mg twice daily received 120 tablets in 90 days (120 ÷ 2 times daily = 60 days filled), then the MPR is 60 divided by 90 days, which equals 0.67, or 67%. Nearly perfect adherence includes MPRs in the range of 0.9 to 1.1. Because of the timeconsuming procedure for calculating an MPR, healthcare professionals typically will simply estimate adherence based on whether refill dates are roughly on time.11
During an interview, a variety of information may need to be gathered. If it is determined prior to the conversation that a patient is nonadherent based on refill history, this may provide an important opportunity for the pharmacist to assess and address barriers. However, care must be taken not to appear accusatory. One way to ask about inconsistent refill history is, "Many patients have difficulty remembering to take their medication. What kind of problems have you experienced?" Similar open-ended questions will give the patient the opportunity to open up about potential issues he or she is experiencing. Asking patients how they take their medication creates another opportunity to assess adherence. Patients who give vague replies (e.g., "I take it how I'm supposed to take it") or are unable to answer may not be adherent to their regimen.11 Setting expectations early on about the types of questions that may be asked will help patients feel less scrutinized or challenged when they are queried about potential adherence problems.
Motivational interviewing is a well-accepted method for questioning and educating patients, particularly if they are nonadherent, passive, or reluctant. Designed to assess and assist patients in the process of change, motivational interviewing consists of five main communication principles: 1) roll with resistance, 2) express empathy, 3) avoid argumentation, 4) develop discrepancy, and 5) support self-efficacy. Self-efficacy may be described as the patient's belief and/or confidence in achieving his or her goals. This type of interaction requires the healthcare provider to develop a partnership with the patient to facilitate information exchange and shared decision making. When approaching this type of interview, the healthcare provider must be aware of his or her own barriers to good communication. These include such things as body positioning (e.g., facing a computer rather than the patient), tone (e.g., judgmental), active listening (e.g., mind on other issues instead of the patient), and approaching education or recommendations with authority rather than with the patient's specific circumstances in mind. Motivational interviewing should include such strategies as nonjudgmental, open-ended questioning; active listening and empathic responding; supporting and affirming self-efficacy; and summarizing conversation points. Overall, the goal of motivational interviewing is to help patients determine reasons for changing their behavior (in the case of medications, to adhere to prescribed therapy for reasons that are meaningful to the patient).12
Addressing specific barriers is an important part of the communication process. Particular communication challenges with adherence arise with the use of injectable agents, and based on the growing body of evidence for GLP-1 agonists, the use of injectables is increasing. The prescribing of injectables may stimulate particular fears in patients, including the perception that their diabetes is worsening, injection-related anxiety, fear of hypoglycemia, fear of weight gain, and concern about the monitoring burden. Strategies for these injectable-specific concerns have been suggested. Education is a large component of addressing patient fears, particularly those concerning disease progression. Reinforcing the patient's understanding of the progressive nature of the diabetes disease process throughout treatment may make the initiation of injectables less threatening. Injection-related fears may be allayed by practice opportunities, careful instruction in appropriate injection technique, explanation of device and needle design to minimize discomfort, and minimizing the number of daily injections and monitoring points when possible. Fears regarding hypoglycemia and weight gain may be addressed depending on the type of injectable prescribed. For example, GLP-1 agonists may promote weight loss and are associated with a low risk of hypoglycemia. Weight gain associated with basal insulin use may be mitigated through adherence to metformin and minimized with concomitant diet and exercise. The use of basal insulin in general, and especially the newer basal insulin analogues, has been associated with lower hypoglycemia risk.13,14
Strategies to Promote Adherence
Barriers to medication adherence are intricate and diverse, and solutions to promote adherence need to be strategic and multidimensional.5 Current literature suggests that implementation of one intervention to promote medication adherence is only modestly successful.4 Because medication nonadherence is multifaceted, multiple strategies should be employed to help improve adherence when possible. There are four general categories for improving medication adherence: patient education, improved dosing regimens, enhanced communication between patient and provider, and increased provider availability.1,15,16
To help improve adherence, educational interventions should be implemented at diagnosis, individualized, and repeated. Interventions should include the patient, any caregivers, and family members, when feasible. When the pharmacist is creating and implementing educational interventions, care should be taken to foster a shame-free environment in which patients feel comfortable asking questions.5 Face-to-face education has been the most successful at improving adherence. When possible, teach-back methods should be used to verify understanding. If handouts are used for educational purposes, they should have a minimum of text, use pictures and diagrams, and incorporate audiovisual materials when feasible.5 For text, lay language written at a fifth-grade level should be used. Educational strategies are generally acceptable to patients; however, they typically require additional healthcare personnel and a significant time commitment.
Addressing the treatment regimen's complexity can have a positive effect on adherence. The dosing regimen can be simplified in many different ways. Methods include employing pillboxes, switching to once-daily dosing, changing to combination medications, maximizing each medication prior to initiating a new one, establishing reminders for taking medications, and using 90-day prescriptions for maintenance medications.1,5
Enhancing the provider-patient relationship can increase medication adherence, and the first step is effective communication. Creating an open, friendly environment can help cultivate meaningful communication. A patient-centered approach should be employed to involve patients in treatment decisions, when appropriate; this method has increased medication adherence.5 Ways to involve the patient include asking what time of day the patient would like to take the medication, offering a choice of treatment options, explaining the rationale for a treatment option (e.g., risk vs. benefit, side-effect profile), and encouraging their input.5 Discussing potential medication side effects prior to starting the new agent increases the likelihood of medication adherence.
Increasing the provider's availability has been shown to improve medication adherence. Ways to enhance provider availability include increased convenience of appointment scheduling, expanded clinic hours (including evenings), telehealth encounters, and greater number of ancillary healthcare providers such as pharmacists, nurses, and behavioral specialists.2 Team-based care also improves medication adherence. Use of a pharmacist-led medication reconciliation, tailored regimens, patient education, and collaborative care between pharmacist and provider has yielded positive results in medication adherence.17
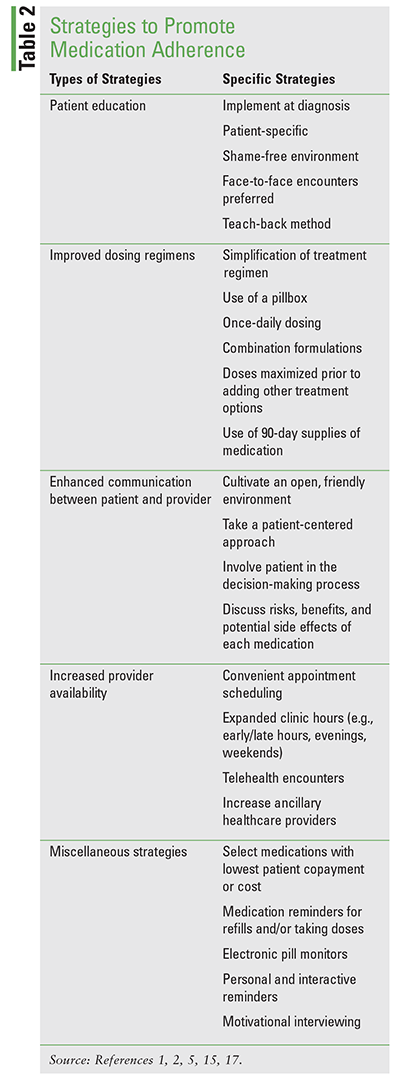 Other strategies for enhancing medication adherence that do not fall under one of the above categories have been identified. Prescribing medications with the lowest patient cost or copayment positively affects medication adherence.2 Medication-taking reminders such as text messaging, telephone calls, refill messages, and electronic drug monitors help increase medication adherence. Electronic pill monitors can remind patients to take their medications and communicate missed doses to the provider, which has been shown to increase medication adherence.17 Personalized and interactive reminders are more effective than generic prerecorded messages.2 Cognitive-behavioral interventions such as motivational interviewing, planned behavior education, and self-management strategies may enhance adherence. Strategies to promote medication adherence are presented in TABLE 2.1,2,5,15,17
Other strategies for enhancing medication adherence that do not fall under one of the above categories have been identified. Prescribing medications with the lowest patient cost or copayment positively affects medication adherence.2 Medication-taking reminders such as text messaging, telephone calls, refill messages, and electronic drug monitors help increase medication adherence. Electronic pill monitors can remind patients to take their medications and communicate missed doses to the provider, which has been shown to increase medication adherence.17 Personalized and interactive reminders are more effective than generic prerecorded messages.2 Cognitive-behavioral interventions such as motivational interviewing, planned behavior education, and self-management strategies may enhance adherence. Strategies to promote medication adherence are presented in TABLE 2.1,2,5,15,17
Clinical Inertia
Despite the known importance and benefits of early achievement of glycemic goals, many patients with type 2 diabetes do not receive prompt treatment intensification upon failure of the initial therapy to achieve glycemic control. The failure of healthcare providers to initiate or intensify therapy when indicated, a topic frequently discussed in the context of diabetes, has been termed clinical inertia. Clinical inertia is increasingly recognized as a widespread problem that can affect diabetes patients at every disease stage, but it may have particular impact early in the disease; this is because prolonged hyperglycemia leads to disease progression as well as to microvascular and macrovascular complications.14,18,19 Factors that contribute to clinical inertia in diabetes include elements specific to both healthcare providers and patients, all of which may be impacted by overarching system-level issues. Pharmacists may have a beneficial impact at several points to prevent clinical inertia from negatively impacting patient care.
In the past decade, many new medications for the treatment of diabetes have come to market. Additionally, a variety of formulations and administration methods are available among the different drug classes. Separate from these medication-specific considerations, many agents have been associated with a variety of risks and benefits, and the benefit of cardiovascular protection is of particular interest. This has resulted in guideline updates that allow for a more patient-centered—but also more complicated—treatment algorithm. As the available options and drug-specific considerations have grown more complex, so too has the decision-making process for treating individual patients with diabetes. Healthcare providers are frequently limited by time and resources, which affects their ability to assess patient-specific barriers; they also may limited in their scope of knowledge of the efficacy and safety of the many newer agents and guideline recommendations.19,20 Pharmacists, having that breadth of knowledge, are uniquely suited to educate prescribers, assess patient-specific factors, and make recommendations that help the prescriber select from the available pharmacotherapy options an agent that maximizes the benefits to the patient.
In addition to the increased number of medication options, the number and type of injectable options have expanded. GLP-1 agonists and basal insulins are recommended as standard second-line or later therapy-intensification options by the American Diabetes Association's Standards of Medical Care in Diabetes and the American Academy of Clinical Endocrinologists' Consensus Statement guidelines.21,22 Benefits of these therapies are numerous; however, all of these agents are formulated as injectables. Although drug companies continue to develop new injectable devices (e.g., pens) to ease the patient's burden of administration, many patients still perceive the need for injection as a significant drawback of these medications. The cost burden of these agents may also be a barrier to their use. Providers view patient reluctance and history of nonadherence as barriers to insulin initiation.14,20,23 A history of side effects (especially hypoglycemia) with medication use and multiple comorbidities may also influence decision making, not just for injectables but for intensification of therapy in general.20 Pharmacists are uniquely placed to educate providers and patients regarding risks and benefits and to help patients overcome barriers such as concerns about injections and cost. Newer data suggest that the involvement of an interdisciplinary team including pharmacists may improve treatment intensification.24
Finally, from a health-system standpoint, two of the most significant factors influencing clinical inertia are time and resources (e.g., supportive technologies). The creation of individualized pharmacotherapy plans is limited by the time a provider has to discuss and implement new and potentially complex options. In the absence of the time and resources needed to appropriately educate a patient about a new treatment, therapy intensification is less likely to occur.19 The implementation of interdisciplinary care is an option for maximizing resources in a complex care system.
The Pharmacist's Role
Patient adherence is imperative to maximizing the benefits of pharmacotherapy regimens for type 2 diabetes. Adherence is affected by a variety of actual and perceived barriers on the part of both the patient and the healthcare provider. There are a number of proven techniques by which healthcare providers can assist patients in achieving and maintaining optimal adherence, not the least of which is establishing a relationship that facilitates cooperation and encourages patient self-efficacy. Communication is a crucial factor in addressing barriers and motivating patients to adhere to their diabetes care plans. Clinical inertia is an important concept that may be influenced by, and can also influence, patients' ability to carefully adhere to their pharmacotherapy. All healthcare providers can play a role in ensuring the development and maintenance of an evidence-based, patient-centered medication regimen. Pharmacists, being widely placed throughout the healthcare system, can influence patient adherence at a number of key interaction points. Extensive knowledge of medications, experience with patient barriers (e.g., lack of understanding, administration concerns, cost issues), communication and interviewing skills, and access make the pharmacist the ideal healthcare provider to address and ensure medication adherence in patients with type 2 diabetes.
REFERENCES
- Osterberg L, Blaschke T. Adherence to medication. N Engl J Med. 2005;353:487-497.
- Kini V, Ho PM. Interventions to improve medication adherence: a review. JAMA. 2018;320:2461-2473.
- American Association of Diabetes Educators. Fostering medication adherence: tips and tricks. www.diabeteseducator.org/docs/ default-source/living-with-diabetes/tip-sheets/medication-taking/ fostering_med_adherence.pdf?sfvrsn=4. Accessed May 15, 2019.
- Ho PM, Bryson CL, Rumsfeld JS. Medication adherence: its importance in cardiovascular outcomes. Circulation. 2009;119:3028-3035.
- Brown MT, Bussell JK. Medication adherence: WHO cares? Mayo Clin Proc. 2011;86:304-314.
- McGovern A, Tippu Z, Hinton W, et al. Systematic review of adherence rates by medication class in type 2 diabetes: a study protocol. BMJ Open. 2016;6:e010469.
- Zullig LL, Gellad WF, Moaddeb J, et al. Improving diabetes medication adherence: successful, scalable interventions. Patient Prefer Adherence. 2015;9:139-149.
- Egede LE, Gebregziabher M, Dismuke CE, et al. Medication nonadherence in diabetes: longitudinal effects on costs and potential cost savings from improvement. Diabetes Care. 2012;35:2533-2539.
- Sabaté E. Adherence to long-term therapies: evidence for action. Geneva, Switzerland: World Health Organization; 2003.
- McGovern A, Tippu Z, Hinton W, et al. Comparison of medication adherence and persistence in type 2 diabetes: a systematic review and meta-analysis. Diabetes Obes Metab. 2018;20:10401043.
- Dealing with patient adherence issues. In: Herrier RN, Apgar DA, Boyce RW, Foster SL, eds. Patient Assessment in Pharmacy. New York, NY: McGraw-Hill; 2015.
- Sherman J. Counseling and motivational interviewing. In: Ellis AW, Sherman JJ, eds. Community and Clinical Pharmacy Services: A Step-by-Step Approach. New York, NY: McGraw-Hill; 2013.
- Santos Cavaiola T, Kiriakov Y, Reid T. Primary care management of patients with type 2 diabetes: overcoming inertia and advancing therapy with the use of injectables. Clin Ther. 2019;41:352-367.
- Kruger DF, LaRue S, Estepa P. Recognition of and steps to mitigate anxiety and fear of pain in injectable diabetes treatment. Diabetes Metab Syndr Obes. 2015;8:49-56.
- McDonald HP, Garg AX, Haynes RB. Interventions to enhance patient adherence to prescriptions: scientific review. JAMA. 2002;288:2868-2879.
- Kocurek B. Promoting medication adherence in older adults… and the rest of us. Diabetes Spectrum. 2009;22(2):80-84.
- Neiman AB, Ruppar T, Ho M, et al. CDC grand rounds: improving medication adherence for chronic disease management—innovations and opportunities. MMWR Morb Mortal Wkly Rep. 2017;66:1248-1251.
- Phillips LS, Branch WT, Cook CB, et al. Clinical inertia. Ann Intern Med. 2001;135:825-834.
- Reach G, Pechtner V, Gentilella R, et al. Clinical inertia and its impact on treatment intensification in people with type 2 diabetes mellitus. Diabetes Metab. 2017;43:501-511.
- Aujoulat I, Jacquemin P, Rietzschel E, et al. Factors associated with clinical inertia: an integrative review. Adv Med Educ Pract. 2014;5:141-147.
- American Diabetes Association. Standards of medical care in diabetes—2019. Diabetes Care. 2019;42(suppl 1):S1-S2.
- Garber AJ, Abrahamson MJ, Barzilay JI, et al. Consensus statement by the American Association of Clinical Endocrinologists and American College of Endocrinology on the comprehensive type 2 diabetes management algorithm—2018 executive summary. Endocr Pract. 2018;24:91-120.
- Ratanawongsa N, Crosson JC, Schillinger D, et al. Getting under the skin of clinical inertia in insulin initiation: the Translating Research Into Action for Diabetes (TRIAD) Insulin Starts Project. Diabetes Educ. 2012;38:94-100.
- Gatwood JD, Chisholm-Burns M, Davis R, et al. Impact of pharmacy services on initial clinical outcomes and medication adherence among veterans with uncontrolled diabetes. BMC Health Serv Res. 2018;18:855.