Preventive Treatment for Patients With Migraine and Cardiovascular Disease
RELEASE DATE:
December 4, 2018
EXPIRATION DATE:
December 31, 2020
FACULTY:
Kiran Panesar, BPharmS (Hons),
MRPharmS, RPh, CPh
Consultant Pharmacist and Medical Writer
Orlando, Florida
FACULTY DISCLOSURE STATEMENTS:
Dr. Panesar has no actual or potential conflicts of interest in relation to this activity.
Postgraduate Healthcare Education, LLC does not view the existence of relationships as an implication of bias or that the value of the material is decreased. The content of the activity was planned to be balanced, objective, and scientifically rigorous. Occasionally, authors may express opinions that represent their own viewpoint. Conclusions drawn by participants should be derived from objective analysis of scientific data.
ACCREDITATION STATEMENT:
Pharmacy
 Postgraduate Healthcare Education, LLC is accredited by the Accreditation Council for Pharmacy Education as a provider of continuing pharmacy education.
Postgraduate Healthcare Education, LLC is accredited by the Accreditation Council for Pharmacy Education as a provider of continuing pharmacy education.
UAN: 0430-0000-18-080-H01-P
Credits: 2.0 hours (0.20 ceu)
Type of Activity: Knowledge
TARGET AUDIENCE:
This accredited activity is targeted to pharmacists. Estimated time to complete this activity is 120 minutes.
Exam processing and other inquiries to:
CE Customer Service: (800) 825-4696 or cecustomerservice@powerpak.com
DISCLAIMER:
Participants have an implied responsibility to use the newly acquired information to enhance patient outcomes and their own professional development. The information presented in this activity is not meant to serve as a guideline for patient management. Any procedures, medications, or other courses of diagnosis or treatment discussed or suggested in this activity should not be used by clinicians without evaluation of their patients' conditions and possible contraindications or dangers in use, review of any applicable manufacturer's product information, and comparison with recommendations of other authorities.
GOAL:
To educate pharmacists about the cardiovascular (CV) disorders associated with migraines, the CV risks associated with current migraine therapies, and the properties of prophylactic therapies for migraine patients at risk for CV disease.
OBJECTIVES:
After completing this activity, the participant should be able to:
- Recognize the burden caused by migraine disorders.
- Discuss the current evidence available on migraine disorders and CV comorbidities and describe the CV risks associated with existing migraine therapies.
- Select suitable prophylactic therapies for migraine prevention in adults with CV risk or comorbidities.
- Recommend appropriate doses and counsel patients on the use of selected therapies
ABSTRACT: Migraine is a disabling disorder that also carries a significant economic burden. Migraines have been associated with a range of comorbid conditions, including cardiovascular disorders such as hypertension, stroke, and myocardial infarction. The triptans and ergot alkaloids indicated for the management of acute migraine attacks are often contraindicated in patients with an increased risk of cardiovascular disorders. The management of migraine patients with cardiovascular disorders, therefore, is challenging. In addition to emerging medications, there are existing prophylactic therapies that may be effective for preventing migraine attacks. Furthermore, many of the prophylactic therapies may be used to treat comorbid cardiovascular disorders.
Migraine is a common chronic disorder involving episodic attacks of moderate-to-severe throbbing headaches lasting 4 to 72 hours and often associated with nausea, vomiting, photophobia, and phonophobia.1,2 Migraine disorders may be classified as migraine without aura, migraine with aura, familial or sporadic hemiplegic migraine, and basilar migraine.3 About one-third of patients experience aura before or during migraines, including speech, sensory, visual, or motor symptoms.2
Migraines, which may begin in late childhood or early adolescence, follow a variety of clinical courses. The headaches may go into remission after a few years, recur in cycles of variable activity for many years or decades, or evolve into a chronic and more refractory state.4 Although in preadolescents migraines are more common in boys than in girls, in adults they are three times more common in women than in men (17.1% of women vs. 5.6% of men in the United States).2
The highest prevalence of migraine occurs in the fifth decade of life and significantly decreases in the sixth and seventh decades; migraine is rarely noted in later decades.4
Some studies have shown that the tendency to develop migraines may be inherited. There is a 40% chance that children with one parent who suffers from migraines will develop the disorder and a 75% chance that children in whom both parents get migraines will develop it.4
Migraine is responsible for 2.9% of all years of life lost to disability; accordingly, it is ranked as the seventh most disabling disorder among all diseases and the leading cause of disability among all neurologic disorders.5 Migraines are associated with various comorbidities and concomitant disorders that ultimately influence treatment plans, which affects how well migraines can be managed. Comorbid conditions are those that occur more frequently in association with a specific disease than they do in the general population.6 Concomitant disorders occur simultaneously in a patient and occur at the rate that would be assumed by chance. Diagnosing and treating migraine with comorbidities can be time-consuming, as more follow-up and monitoring of the various disorders is required.
There is increasing evidence that individuals who get migraines, particularly migraines with aura, have a higher cardiovascular (CV) risk profile than persons who do not get migraines.
Although migraine pathophysiology is incompletely understood, vascular mechanisms are clearly implicated.1 These mechanisms include endothelial dysfunction, hypercoagulability, and pathological vascular reactivity.1 Additionally, the biological mechanisms that underlie the elevated risk remain unclear and complex.7
The high prevalence of both migraine and CV disorders, along with the consequences of CV disorders, means that a potential association between the two can result in a substantial impact on public health.1
HYPERTENSION
Although the relationship between migraine and hypertension remains unclear and is still being investigated, the prevalence of comorbid hypertension and migraine is substantial.8 Furthermore, compared with patients who are hypertensive, those with comorbid migraine and hypertension have a higher probability of a history of cerebrovascular events.8
A prospective cohort study of a Finnish working-age population that explored whether self-reported migraine at baseline predicted hypertension 5 years later demonstrated that the risk of hypertension was almost 1.5 times higher in persons with migraine than in those without initial migraine.7 It is important to note, however, that although the study was conducted in a homogenous population-based sample, the response rate was low, the occurrence of migraines was self-reported, and some patients may have mistaken other types of headaches for migraines.7 Additionally, because some patients were taking medication for migraines and some antihypertensive medications are also used for migraine prevention, the occurrence of migraines may have been underreported.7
On the other hand, the Nord-Trondelag Health Survey, a large-scale population-based cohort study, demonstrated an inverse relationship between blood pressure and subsequent development of headache. However, further research is needed to determine the mechanisms that may explain these findings.9 Other studies have found that poor control of blood pressure can increase the frequency and severity of migraines.10
The age-adjusted prevalence of hypertension among U.S. adults was 29.1% from 2011 through 2012.11 Owing to this high prevalence, continued research to establish the relationship between migraine and hypertension is clearly required. As some studies have shown disparities across racial and ethnic groups, the research should be tailored to identify these differences.12
CARDIOVASCULAR DISEASE
Although studies have not shown a direct relationship between migraine and coronary heart disease, there is a possible association between migraine and vasospastic disorders such as variant angina and Raynaud phenomenon.13 Raynaud phenomenon and other peripheral vascular diseases are sometimes a sign of increased risk of coronary artery disease.
A large-scale population-based study conducted over 10 years found that although the risk of angina was higher in patients who experienced migraines and higher still in patients who had migraines with aura, there was no relationship between coronary artery disease and migraine with aura.14
The Women's Health Study and the Physicians' Health Study concluded that participants who reported migraines were not at increased risk either for subsequent major coronary heart disease or for myocardial infarction or angina.13,15,16
PATENT FORAMEN OVALE
Patent foramen ovale (PFO) is a structural heart abnormality that can lead to a right-to-left cardiac shunt. Migraine with aura has been found to be 3.5 times more prevalent in patients with a right-to-left shunt than in those without the shunt. Furthermore, it has been noted that migraine symptoms disappear or improve after closure of the foramen ovale.17 PFO is a well-known risk factor for stroke.18
MIGRAINE AND ISCHEMIC STROKE
Although studies have consistently found an association between migraine and ischemic stroke, the underlying mechanism is still under investigation. A systematic review and meta-analysis of case-control and cohort studies determined that migraine with aura is associated with a twofold increased risk of ischemic stroke and that the risk is higher in women, persons aged younger than 45 years, smokers, and women taking oral contraceptives.1 A subset of ischemic stroke known as migrainous infarction may occur in the posterior circulation of younger women suffering from migraine. Various factors have been implicated in migrainous infarction, including gender, inflammation, vascular causes, PFO, endothelial structure, smoking, and oral contraceptives.2 The ergot alkaloids and triptans that are commonly used in the management of migraines have a vasoconstrictor effect and may also play a role in migrainous infarctions by increasing blood pressure.2
Rare genetic disorders such as cerebral autosomal-dominant arteriopathy with subcortical infarcts and leukoencephalopathy, retinal vasculopathy with cerebral leukodystrophy, and others may also cause migraines and infarcts.2
TREATING MIGRAINE IN THE PRESENCE OF CARDIOVASCULAR DISEASE
Treatment plans for migraine and comorbid or concomitant conditions must be designed to take into account all of the conditions present, as well as the tolerability and adverse effects associated with treatment drugs. Ergot alkaloids have been shown to induce arterial vasoconstriction, thereby increasing blood pressure, whereas triptans produce contractions of the coronary arteries.19,20
Triptans are contraindicated in the presence of CV, cerebrovascular, and peripheral vascular diseases. Although severe CV reactions such as stroke, myocardial infarction, and ischemic heart disease have been reported with triptan use, the incidence is estimated at less than one in 4 million treatments.4 However, even though the CV risk and risk of mortality are very low in general practice, prescribers tend to avoid the use of triptans in patients with a CV risk profile.20-25 Furthermore, only 50% to 60% of patients consistently respond to triptans.26 Because untreated migraine can cause substantial debility, it is important that prescribers effectively manage migraine patients with a CV risk profile.20 Unfortunately, because most data on triptans are derived from patients without known CV disease, they cannot be applied to patients with CV disease without further investigation. The difficulty lies in determining whether a patient with potential unrecognized CV disease is an appropriate candidate for triptan therapy.27 One panel of experts suggested that although prescribers should use caution when recommending triptans to patients with two or more CV risk factors, patients who have fewer than two CV risk factors and moderate-to-severe migraines should be considered for triptan therapy.28
The prescribing of ergot alkaloids, which cause vasoconstriction, is also lower in patients with a CV risk profile.29
Therefore, the selection of treatment for patients with migraine must take into account not only the patient's risk factors, but also age, gender, and other medications that could result in potential drug interactions.2 These include innovative drug-delivery systems to reduce side effects and the use of prophylactics to reduce migraine attacks.
New Drug-Delivery Systems
Traditional migraine agents administered via innovative drug-delivery systems that increase the bioavailability of the drug and provide rapid relief may enable dose reduction and, consequently, potentially lessen CV side effects.2 This could allow the use of these drugs in patients with a greater CV risk. Mucoadhesive buccal discs and polymeric carriers administered intranasally have been tested with regard to this effect.2,30,31
Prophylactic Therapies
Prophylactic therapy is indicated for patients with recurrent migraines that interfere with daily activity; those with a contraindication to, failure of, overuse of, or adverse effects from acute therapy; those preferring this type of therapy; and those with uncommon migraine types (e.g., hemiplegic, basilar).4 The goals of preventive therapy include reducing the frequency, severity, and duration of attacks; improving the response to treatment of acute attacks; and improving function and reducing disability.32
Migraine prophylaxis includes migraine-trigger avoidance, lifestyle changes, and nonpharmacologic and pharmacologic therapy. Selection of prophylactic therapy should be based on efficacy, patient preference, comorbid conditions, and the drug's side-effect profile. Patients in whom prophylactic therapy is indicated should also be counseled on migraine triggers and lifestyle-related factors that can precipitate a migraine. TABLE 1 lists some of these factors.33
Nonpharmacologic methods for migraine prophylaxis include relaxation training and thermal biofeedback combined with relaxation training, electromyography biofeedback, and cognitive-behavioral therapy. Randomized, controlled trials have shown that these techniques reduce migraine frequency by 30% to 50%.4
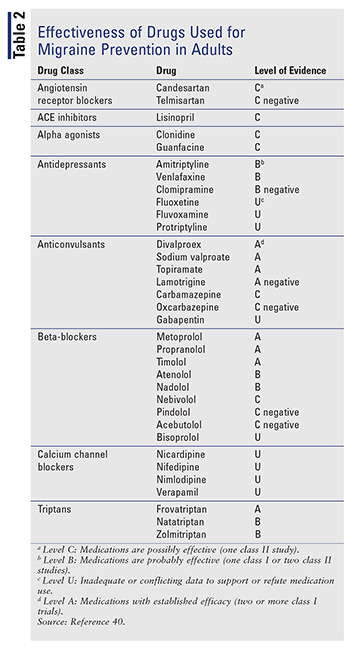
A range of pharmacologic options are available for migraine prophylaxis, from traditional to more recent medications. Traditional agents (beta-blockers, ACE inhibitors, angiotensin II receptor blockers [ARBs], anticonvulsants, and antidepressants) typically have primary indications for other conditions, some of which are relatively common in persons with migraine, including stroke, myocardial infarction, Raynaud syndrome, epilepsy, affective disorders, and anxiety disorders.4 TABLE 2 summarizes the effectiveness of these agents. Emerging medications include botulinum type A toxin and tonabersat, but further research is required to establish their place in migraine prophylaxis.34 Statins, including those given in combination with vitamin D, have been shown to reduce the frequency, severity, and disability of migraines.35-39
Beta-blockers are indicated in the management of atrial tachyarrhythmias and atrial fibrillation, thyrotoxicosis (short-term), essential tremor, perioperative hypertension, and migraine. A number of beta-blockers, including atenolol, metoprolol, nadolol, timolol, and propranolol, have been found effective for migraine prevention.40,41 Since beta-blockers may be used to treat both hypertension and migraines and the drug interactions are minimal or limited, these drugs can be a utile and cost-effective option for managing migraine patients with comorbid hypertension.
ACE Inhibitors: Lisinopril is effective prophylactic treatment for frequent migraine attacks, as demonstrated by a number of studies.35 It has been rated as a level C agent (possibly effective) by the American Academy of Neurology.40 Lisinopril's primary pharmacologic action is to block the conversion of angiotensin I to angiotensin II. Other pharmacologic actions include altering sympathetic activity, inhibiting free-radical activity, increasing prostacyclin synthesis, and blocking the degradation of bradykinin, encephalin, and substance P. It has been observed that migraine without aura seems to be more common in persons with the DDACE gene, and migraineurs with this gene also have higher ACE activity and a higher frequency of attacks than other migraine sufferers.35
Angiotensin II Receptor Blockers: These agents block the renin-angiotensin system without interfering with bradykinin, substance P, or tachykinin metabolism; therefore, they do not cause the usual adverse effects associated with ACE inhibitors, such as coughing and angioneurotic edema. Candesartan is the only ARB that has been shown to be possibly effective, and it may be considered for migraine prevention.42
Antidepressants: A meta-analysis of studies assessing the efficacy of antidepressants for migraine prophylaxis showed that patients who took antidepressants were more likely to experience a reduction of headache burden compared with patients given placebo.43 Amitriptyline and venlafaxine (level B) are considered effective and may be considered for migraine prevention.44
Anticonvulsants: Among the anticonvulsants, valproic acid and topiramate seem to be the most effective, as reported in controlled studies.45
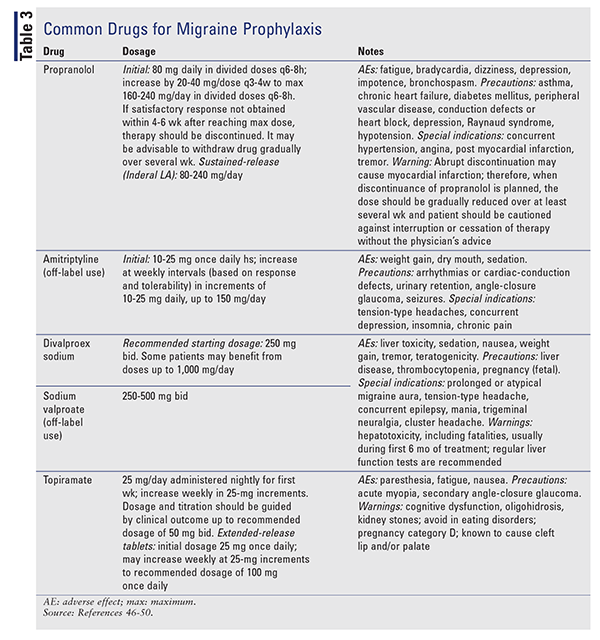
TABLE 3 summarizes some of the drugs that are commonly used in the prophylactic management of migraine headaches.46-50 The medications are FDA-approved unless otherwise indicated in the table.
CONCLUSION
The management of migraine patients with comorbid CV disorders requires careful consideration of the conditions present, potential adverse effects, and possible drug interactions. Therapy is not the same for all migraine patients; a variety of nonpharmacologic and pharmacologic options are available, as well as emerging therapies such as galcanezumab, eptinezumab, erenumab, and fremanezumab.51 Pharmacists are well equipped and ideally placed to suggest tailor-made solutions for each patient and to provide counseling and support to those patients who are already on medication.
REFERENCES
- Schürks M, Rist PM, Bigal ME, et al. Migraine and cardiovascular disease: systematic review and meta-analysis. BMJ. 2009;339:b3914.
- Zhang Y, Parikh A, Qian S. Migraine and stroke. Stroke Vasc Neurol. 2017;2(3):160-167.
- Estemalik E, Tepper S. Preventive treatment in migraine and the new US guidelines. Neuropsychiatr Dis Treat. 2013;9:709-720.
- MacGregor EA. In the clinic. Migraine. Ann Intern Med. 2013;159(9):ITC5-1-ITC5-16.
- Steiner TJ, Stovner LJ, Birbeck GL. Migraine: the seventh disabler. J Headache Pain. 2013;14:1.
- Lipton RB, Silberstein SD. Why study the comorbidity of migraine? Neurology. 1994;44(10 suppl 7):S4-S5.
- Entonen AH, Suominen SB, Korkeila K, et al. Migraine predicts hypertension—a cohort study of the Finnish working-age population. Eur J Public Health. 2014;24(2):244-248.
- Mancia G, Rosei EA, Ambrosioni E, et al. Hypertension and migraine comorbidity: prevalence and risk of cerebrovascular events: evidence from a large, multicenter, cross-sectional survey in Italy (MIRACLES study). J Hypertens. 2011;29(2):309-318.
- Fagernaes CF, Heuch I, Zwart JA, et al. Blood pressure as a risk factor for headache and migraine: a prospective population-based study. Eur J Neurol. 2015;22(1):156-162,e10-e11.
- Prentice D, Heywood J. Migraine and hypertension. Is there a relationship? Aust Fam Physician. 2001;30(5):461-465.
- Nwankwo T, Yoon SS, Burt V, Gu Q. Hypertension among adults in the United States: National Health and Nutrition Examination Survey, 2011-2012. NCHS Data Brief. 2013;133:1-8.
- Gardener H, Monteith T, Rundek T, et al. Hypertension and migraine in the Northern Manhattan Study. Ethn Dis. 2016;26(3):323-330.
- Rosamond W. Are migraine and coronary heart disease associated? An epidemiologic review. Headache. 2004;44(suppl 1):S5-S12.
- Rose KM, Carson AP, Sanford CP, et al. Migraine and other headaches: associations with Rose angina and coronary heart disease. Neurology. 2004;63(12):2233-2239.
- Kurth T, Schürks M, Logroscino G, et al. Migraine, vascular risk, and cardiovascular events in women: prospective cohort study. BMJ. 2008;337:a636.
- Pierangeli G, Cevoli S, Zanigni S, et al. The role of cardiac diseases in the comorbidity between migraine and stroke. Neurol Sci. 2004;25(suppl 3):S129-S131.
- Wammes-van der Heijden EA, Tijssen CC, Egberts ACG. right-to-left shunt and migraine: the strength of the relationship. Cephalalgia. 2006;26(2):208-213.
- Katsarava Z, Weimar C. Migraine and stroke. J Neurol Sci. 2010;299(1-2):42-44.
- Tajti J, Majláth Z, Szok D, et al. Drug safety in acute migraine treatment. Expert Opin Drug Saf. 2015;14(6):891-909.
- Dodick DW. Introduction: cardiovascular safety and triptans in the acute treatment of migraine. Headache. 2004;44(suppl 1):S1-S4.
- Maassen Van Den Brink A, Saxena PR. Coronary vasoconstrictor potential of triptans: a review of in vitro pharmacologic data. Headache. 2004;44 (suppl 1):S13-S19.
- Allen C, Dayno J. Tolerability of sumatriptan: clinical trials and postmarketing experience. Cephalalgia. 2001;21(8):855-856.
- Dahlöf CG, Mathew N. Cardiovascular safety of 5HT1B/1D agonists—is there a cause for concern? Cephalalgia. 1998;18(8): 539-545.
- Dodick DW, Martin VT, Smith T, Silberstein S. Cardiovascular tolerability and safety of triptans: a review of clinical data. Headache. 2004;44(suppl 1):S20-S30.
- Bigal ME, Golden W, Buse D, Chen YT, Lipton RB. Triptan use as a function of cardiovascular risk. A population-based study. Headache. 2010;50(2):256-263.
- Ferrari MD, Roon KI, Lipton RB, Goadsby PJ. Oral triptans (serotonin 5-HT1B/1D agonists) in acute migraine treatment: a metaanalysis of 53 trials. Lancet. 2001;358(9294):1668-1675.
- Papademetriou V. Cardiovascular risk assessment and triptans. Headache. 2004;44(suppl 1):S31-S39.
- Dodick D, Lipton RB, Martin V, et al. Consensus statement: cardiovascular safety profile of triptans (5-HT agonists) in the acute treatment of migraine. Headache. 2004;44(5):414-425.
- Wammes-van der Heijden EA, Tijssen CC, Egberts ACG. Treatment choices and patterns in migraine patients with and without a cardiovascular risk profile. Cephalalgia. 2009;29(3):322-330.
- Gavini E, Rassu G, Ferraro L, et al. Influence of polymeric microcarriers on the in vivo intranasal uptake of an anti-migraine drug for brain targeting. Eur J Pharm Biopharm. 2013;83(2):174-183.
- Jelvehgari M, Valizadeh H, Ziapour S, et al. Comparative study of different combinational mucoadhesive formulations of sumatriptan-metoclopramide. Adv Pharm Bull. 2016;6(1):119-130.
- Morey SS. Guidelines on migraine: part 4. General principles of preventive therapy. Am Fam Physician. 2000;62(10):2359-2360,2363.
- Pringsheim T, Davenport WJ, Becker WJ. Prophylaxis of migraine headache. CMAJ. 2010;182(7):E269-E276.
- Barbanti P, Aurilia C, Egeo G, Fofi L. Migraine prophylaxis: what is new and what we need? Neurol Sci. 2011;32(suppl1):S111-S115.
- Schrader H, Stovner LJ, Helde G, et al. Prophylactic treatment of migraine with angiotensin converting enzyme inhibitor (lisinopril): randomised, placebo controlled, crossover study. BMJ. 2001;322(7277):19-22.
- Limmroth V, Michel MC. The prevention of migraine: a critical review with special emphasis on beta-adrenoceptor blockers. Br J Clin Pharmacol. 2001;52(3):237-243.
- Liberopoulos EN, Mikhailidis DP. Could statins be useful in the treatment of patients with migraine? Headache. 2006;46(4):672-675.
- Medeiros FL, Medeiros PL, Valença MM, Dodick D. Simvastatin for migraine prevention. Headache. 2007;47(6):855-856.
- Buettner C, Nir RR, Bertisch SM, et al. Simvastatin and vitamin D for migraine prevention: a randomized, controlled trial. Ann Neurol. 2015;78(6):970-981.
- Silberstein SD, Holland S, Freitag F, et al. Evidence-based guideline update: pharmacologic treatment for episodic migraine prevention in adults: report of the Quality Standards Subcommittee of the American Academy of Neurology and the American Headache Society. Neurology. 2012;78(17):1337-1345.
- Silberstein SD. Practice parameter: evidence-based guidelines for migraine headache (an evidence-based review): report of the Quality Standards Subcommittee of the American Academy of Neurology. Neurology. 2000;55(6):754-762.
- Tronvik E, Stovner LJ, Helde G, et al. Prophylactic treatment of migraine with an angiotensin II receptor blocker: a randomized controlled trial. JAMA. 2003;289(1):65-69.
- Xu XM, Yang C, Liu Y, et al. Efficacy and feasibility of antidepressants for the prevention of migraine in adults: a meta-analysis. Eur J Neurol. 2017;24(8):1022-1031.
- American Academy of Neurology. Update: pharmacologic treatment for episodic migraine prevention in adults. www.aan.com/ Guidelines/home/GetGuidelineContent/545. Accessed October 15, 2018.
- Chiossi L, Negro A, Capi M, et al. Sodium channel antagonists for the treatment of migraine. Expert Opin Pharmacother. 2014;15(12):1697-1706.
- Modi S, Lowder DM. Medications for migraine prophylaxis. Am Fam Physician. 2006;73(1):72-78.
- Parsekyan D. Migraine prophylaxis in adult patients. West J Med. 2000;173(5):341-345.
- Inderal (propranolol) package insert. Philadelphia, PA: Pfizer Inc; November 2017. Accessed October 15, 2018.
- Depakote (divalproex) package insert. North Chicago, IL: Abbott Laboratories; October 2011. Accessed October 15, 2018.
- Topamax (topiramate) package insert. Titusville, NJ: Janssen Pharmaceuticals Inc; October 2012.
- Reuter U. A review of monoclonal antibody therapies and other preventative treatments in migraine. Headache. 2018;58(suppl 1): 48-59.