Tracking Illicit Opioid Trends
RELEASE DATE
March 1, 2023
EXPIRATION DATE
March 31, 2025
FACULTY
Allie Cooper Ladner, PharmD Candidate Class of 2023
Kelcie Wilding, PharmD Candidate Class of 2023
Elina Delgado, PharmD, BCPS
William Carey University School of Pharmacy
Assistant Professor, Department of Pharmacy Practice
Biloxi, Mississippi
FACULTY DISCLOSURE STATEMENTS
Ms. Cooper Ladner, Ms. Wilding, and Dr. Delgado have no actual or potential conflicts of interest in relation to this activity.
Postgraduate Healthcare Education, LLC does not view the existence of relationships as an implication of bias or that the value of the material is decreased. The content of the activity was planned to be balanced, objective, and scientifically rigorous. Occasionally, authors may express opinions that represent their own viewpoint. Conclusions drawn by participants should be derived from objective analysis of scientific data.
ACCREDITATION STATEMENT
 Pharmacy
Pharmacy
Postgraduate Healthcare Education, LLC is accredited by the Accreditation Council for Pharmacy Education as a provider of continuing pharmacy education.
UAN: 0430-0000-23-027-H08-P
Credits: 2.0 hours (0.20 ceu)
Type of Activity: Knowledge
TARGET AUDIENCE
This accredited activity is targeted to pharmacists. Estimated time to complete this activity is 120 minutes.
Exam processing and other inquiries to:
CE Customer Service: (800) 825-4696 or cecustomerservice@powerpak.com
DISCLAIMER
Participants have an implied responsibility to use the newly acquired information to enhance patient outcomes and their own professional development. The information presented in this activity is not meant to serve as a guideline for patient management. Any procedures, medications, or other courses of diagnosis or treatment discussed or suggested in this activity should not be used by clinicians without evaluation of their patients' conditions and possible contraindications or dangers in use, review of any applicable manufacturer's product information, and comparison with recommendations of other authorities.
GOAL
To apprise pharmacists of the current trends in the illicit use of opioids so they are equipped to aid in the care of patients.
OBJECTIVES
After completing this activity, the participant should be able to:
- Recognize the history of illicit opioid use within the United States.
- Describe the composition of illicit opioid substances currently afflicting the American population.
- Discuss how one can determine if a tablet is counterfeit or homemade.
- Identify a therapeutic naloxone regimen to prevent overdose deaths from illicit opioids
ABSTRACT: Illicit drug use has been on the rise in the United States since the 1990s, and it is not slowing down. Heroin, once a prescribed synthetic opioid, was one of the first to be used recreationally. New trends in the opioid epidemic have emerged despite a concerted effort to mitigate prescriptive access. A few include “Rainbow Fentanyl,” isotonitazene, “Benzo Dope,” and “Tranq Dope.” The deaths related to these substances continue to rise, and the hazardous creativity of dealers is only growing. Pharmacists should focus their efforts on patient education, current news, and naloxone responsibility.
In the healthcare community, it is not uncommon to hear about the opioid crisis or the opioid epidemic. Part of the responsibility of healthcare providers is to be aware of faults in the system, especially when it comes to opioid prescribing now and in the past. It is, however, just as vital to educate on opioids not used in the healthcare setting. Illicit drug use has been on the rise in the United States since the 1990s, and it is not slowing down.1 From 2019 to 2020, the opioid death rate in the U.S. increased by 38%, and those specifically caused by synthetic opioids, excluding methadone, shot up by 56%. Over 82% of opioid overdose deaths in 2020 were due to synthetic opioids. The numbers continue to climb as time progresses, so the need for illicit opioid misuse and overdose education is also rising critically. Of course, pharmacists, as the most readily available healthcare workers to the general public, should be ready to educate patients and spread awareness on this topic.
EVOLUTION OF OPIOIDS
Opium, taking its name from the Greek word “opos” meaning juice, is the liquid extracted from the opium poppy seed.2 The dates of discovery and initial use are unclear, but they are speculated to have occurred in ancient Sumeria in the third millennium BC. The spread of the use of opium for euphoric and analgesic properties also brought with it the spread of drug abuse and addiction. In China, smoking of opium soared once tobacco was outlawed, and efforts to suppress the use were futile. With immigration of Chinese workers to the U.S. in the 1800s to work on the railroads and mine gold came the use of opium and creation of opium dens. Since then, America has been in a constant battle to suppress addiction due to opiates.3
In 1803, Friedrich Sertürner, a German scientist, first isolated the active ingredient of opium, morphine, named after the god of dreams, Morpheus.3 Pure morphine is 10 times stronger than opium, making it a very effective painkiller but equally as addictive. The search for an equally effective but less addictive opioid analgesic has led to the creation of various drugs throughout history (e.g., heroin and oxycontin) but also has contributed to periods of increased use and abuse of certain opiates. In 2016, the CDC released a guideline for prescribing opioids for chronic pain to aid prescribers in the judicious use of opiates and reduce risk of dependence and overdose of opioid prescriptions.4
Morphine Milligram Equivalents
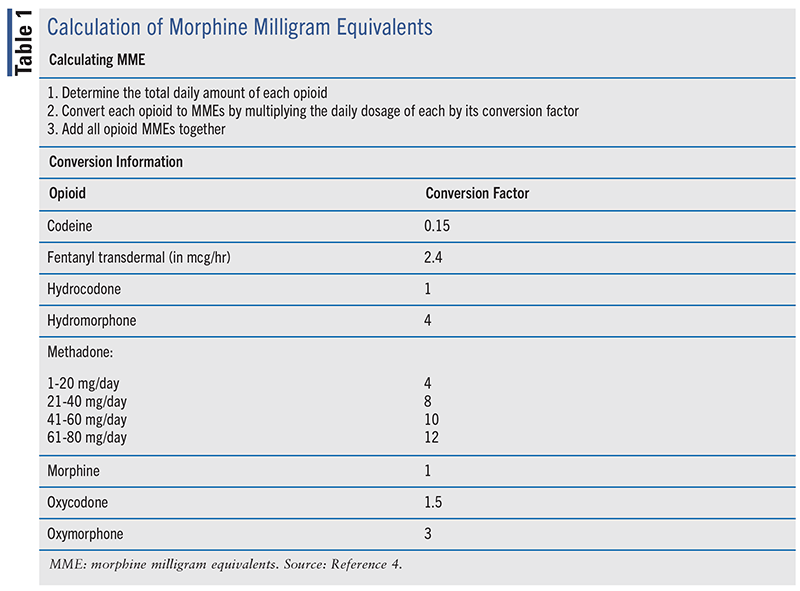
Per the CDC, morphine milligram equivalents (MME) are an opioid dosage’s equivalency to morphine.4 The metric MME/day should be used to gauge overdose potential and not to determine dose equivalence when converting between opioids. Calculation of the total daily dose of opiates can help ensure safe prescribing practices, to include total supply given, need for tapering, and naloxone. It can also allow for identification of patients who may benefit from closer monitoring. Information on how to calculate MME can be found in TABLE 1.
 |
 For acute pain (0-6 weeks), there is no clear guidance on an MME quantity that prescriptions should contain. Instead, the suggestion is to limit opioid use to the minimal dose and duration, along with utilization of nonpharmacologic and nonopioid therapies.5 For chronic pain, the recommendation is to prescribe immediate-release opioids instead of extendedrelease/long-acting and keep doses below 50 MME/day. Published information shows that there is an increased risk of overdose at 20 MME/day and an increased rate of dependence shown for patients on high-dose chronic therapy (odds ratio 3.03 for acute low-dose opioids [1-36 MME/day] vs. 122.45 for patients on chronic high-dose opioids [≥120 MME/day]). By curbing the introduction of opioids and taking steps to mitigate abuse dependence, the hope is to reduce the number of individuals seeking out illicit opioids.
For acute pain (0-6 weeks), there is no clear guidance on an MME quantity that prescriptions should contain. Instead, the suggestion is to limit opioid use to the minimal dose and duration, along with utilization of nonpharmacologic and nonopioid therapies.5 For chronic pain, the recommendation is to prescribe immediate-release opioids instead of extendedrelease/long-acting and keep doses below 50 MME/day. Published information shows that there is an increased risk of overdose at 20 MME/day and an increased rate of dependence shown for patients on high-dose chronic therapy (odds ratio 3.03 for acute low-dose opioids [1-36 MME/day] vs. 122.45 for patients on chronic high-dose opioids [≥120 MME/day]). By curbing the introduction of opioids and taking steps to mitigate abuse dependence, the hope is to reduce the number of individuals seeking out illicit opioids.
EVOLUTION OF STREET OPIOIDS
Heroin
Heroin, or diacetylmorphine, was once considered a wonder drug by the healthcare community.6 It was sold on a commercial scale in 1898 and was hailed as a novel drug, as penicillin and cortisone were when first discovered. The name heroin was German-derived for being “hero-ish.” It was prescribed for many general illnesses and insomnia and was hoped to be effective in combating addiction to morphine and codeine.
Diacetylmorphine is a potent morphine opiate derivative, with an MME of 3 to 4, that has significant central nervous system (CNS)–depressant effects, increases smooth muscle tone, and causes release of catecholamines and histamine.7 Its onset with typical IV administration is less than 1 minute. Metabolism is primarily through serum and liver esterases, and the metabolites 6-acetylmorphine and morphine are also active. Its terminal half-life ranges from 2 to 6 hours. All of these characteristics contribute to heroin’s high abuse potential and addictive properties.
Eventually, it was discovered that heroin posed risks for addiction, even more so than the existing opioids.6 Slowly, the news of a substance with increased euphoric effects compared with morphine and codeine started to spread; the once-novel drug was being used recreationally by many. The growing concern for addiction and abuse led to the public health service hospitals in the U.S. to halt all heroin dispensing in 1916. In 1920, the American Medical Association decided to eliminate all medical preparations of heroin, stop all prescriptions, and cease dispensing it.
Now, heroin is a well-known street drug. It is known for its incidence of overdose and misuse, for its IV administration, and for its addictive euphoric effects. In the healthcare setting, heroin use can be of concern not only for instances of overdose but for bacteremia, skin and soft-tissue infections, and HIV infection.
Opioid Epidemic
Although there were some concerns in the 1990s about opioid-abuse potential, drug companies encouraged healthcare providers to prescribe opioids to patients because of their ability to relieve pain.8,9 What the healthcare providers and drug companies did not know, at that time, was that this would be just the beginning of what is now known as the opioid epidemic. As the number of opioid prescriptions increased, more and more patients were misusing or abusing these drugs. Patients formed dependencies on opioids, and the cases of overdoses spiked.
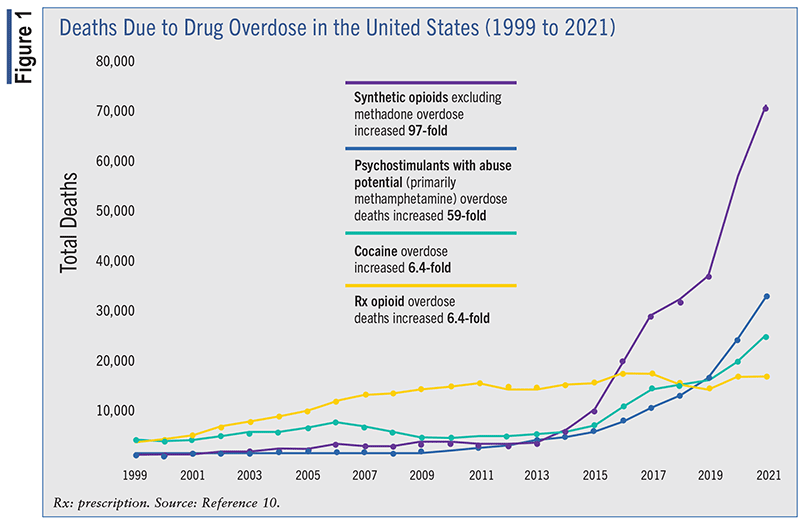
When physicians and other prescribers recognized that many people were becoming addicted to these drugs, providers decreased the number of opioids given or even completely stopped prescribing them, but that led to patients seeking opioids from other sources. Patients unable to obtain a prescription purchased illictly obtained opioids to achieve a “high” and mitigate withdrawal. One of the most profound issues with street drugs is an inability for consumers to ensure substance purity or concentration. This has led to an increase in overdoses, both fatal and nonfatal (see FIGURE 1).10 The Department of Health and Human Services reveals that synthetic opioid overdose death rates have been climbing since 2013, while the prescription opioid overdose death rates have been about the same since around 2007.
 |
Fentanyl Analogues
Fentanyl, a synthetic opioid that is 50 times stronger than heroin and 100 times stronger than morphine, is one of top contributors to drug overdoses in the U.S.11 Fentanyl is a schedule II controlled substance often used in medical practice to manage severe pain. but it has a known high risk of dependence and respiratory distress. Outpatient, it is best known as the 72-hour transdermal patch but is also available in different formulations, such as sublingual tablets, injections, and IV. Illicit fentanyl analogues have been created by altering the chemical structure of fentanyl; these have the same pain-relieving properties as fentanyl but are much more potent. Some fentanyl analogues include acetylfentanyl, carfentanyl, and furanylfentanyl. Carfentanyl (Wildnil), one of the most commonly seen analogues, is known to be 100 times more potent than fentanyl.
The fentanyl obtained from distributors other than reputable healthcare sources is not the same as the fentanyl dispensed by pharmacies and hospitals. While some users are intentionally seeking out these analogues, many are not meaning to consume fentanyl or fentanyl analogues.11 Most cases of fentanyl overdose are related to illicitly used or manufactured fentanyl. It is often mixed with other drugs due to its extreme potency. This helps sellers to produce more powerful, more addictive, and more dangerous illicit drug products for a lower price. Many buyers are often not aware of the added fentanyl in other illicit drugs. It is often mixed with heroin, cocaine, methamphetamine, and even THC.12 Popular street names for illicit substances containing fentanyl and fentanyl analogues are “White Heroin,” “Perc-O-Pops,” and “Redrum” (murder spelled backwards).11 More than 150 people die daily from fentanyl-related overdoses, so it is critical to educate and make the general public aware of how dangerous and how prevalent fentanyl use is, whether people know they are receiving this product or not. A few common street names for fentanyl are Apache, Murder 8, Jackpot, and Dance Fever.12
NOVEL SYNTHETIC OPIOIDS
“Rainbow Fentanyl”
The most recent and alarming trend in the black market has been the colorful fentanyl tablets hitting the streets across the U.S.13 The name “Rainbow Fentanyl” has been in the media since August 2022. These are highly potent fentanyl tablets of various colors targeted toward the younger generations by dealers and cartels. They have been seen in various shapes and sizes, some resembling candy and sidewalk chalk. Many of the people who are manufacturing and selling these tablets do not control the amount of fentanyl in each tablet, making their strengths unpredictable and potentially deadly, especially to younger-aged children. The colorful synthetic drug has been seized by the Drug Enforcement Administration (DEA) in 26 states as of October 2022. In New York City, over 15,000 pills bearing imprints of “M” and “30” were seized. Investigators suspect that these imprints are meant to resemble those on oxycodone hydrochloride 30-mg tablets.14 Among the tablets seized, according to a DEA special agent, over 40% of the pills contained a lethal dose of fentanyl.
Isotonitazene
Isotonitazene, now also known as nitazene or ISO, was originally synthesized and patented by a Swiss pharmaceutical company in 1959 as an analgesic 500 times more potent than morphine.15 It was studied along with three close analogues, one of which is etonitazene. Etonitazene is technically an analogue of isotonitazene, but ISO was sold under this name for its first appearances in the U.S. illicit drug market. Isotonitazene is a synthetic opioid newer to the streets whose effects are similar to fentanyl, as it is more potent than heroin and morphine. It was first identified due to drug seizures in the Midwest by the DEA in 2019 and has since spread across the U.S. This drug can be a yellow, brown, or off-white powder. It has been mixed with other drugs such as heroin or fentanyl and increases the chances of overdose in those who take it. Most consumption is done unknowingly because, just as with fentanyl, this drug is being added to other substances being sold to increase potency at a cheaper price. Specifically, it has been identified in counterfeit tablets being falsely marketed as hydromorphone M-8 tablets and oxycodone M30 tablets. Compared with fentanyl use, isotonitazene prevalence is relatively low, but it has been steadily rising in popularity to sellers in the U.S., and it is important to note when discussing today’s synthetic illicit opioids.16 As discussed with illicit fentanyl, since this is not a commercially available drug in the U.S., the identity, purity, and quantity of the drug are not regulated, increasing the already-present danger for overdose. There have been multiple deaths related to the use of this drug, and along with the other commonly abused opioids, it poses an increased risk to public health.17
"Benzo Dope"
For pharmacists, benzodiazepines (benzos) are commonly seen in practice. There are common risks associated with them that most in the healthcare field are aware of, a few of which are related to their potential for misuse, physical dependence, and tolerance. It is also commonly known that benzos are contraindicated with opioid use and alcohol use due to CNS and respiratory depression. The new “Benzo Dope” formulations take advantage of that.18 This dangerous combination involves a benzo and an opioid mixed together in one hazardous tablet, putting those who consume them in danger of multiple health risks, including the risk for overdose doubling. Benzos possess their own potential for overdose, which often can last longer than opioid overdoses. This, of course, presents a heightened issue for healthcare workers since this combination makes it harder to save those who are already in a state of possible overdose. Naloxone, the rescue drug for opioid overdose, does not have therapeutic effect during a benzo overdose. Not only is the use of naloxone possibly not effective in an emergency situation, but it may also potentially bring the patient into opioid withdrawal while a benzo overdose is simultaneously occurring. As one can see, this deadly combination poses exponential risk for death when an overdose is at hand.
 The most commonly used opioids in Benzo Dope formulations are those that are commonly misused illicitly: heroin and fentanyl. The most commonly used benzodiazepines are flualprazolam (closely related to Xanax), bromazolam (triazolobenzodiazepine synthesized in 1976 but never marketed), and etizolam (a benzo analogue).19 These are obviously not observed much in practice but are still considered benzodiazepines by their structure and physiological effects.
The most commonly used opioids in Benzo Dope formulations are those that are commonly misused illicitly: heroin and fentanyl. The most commonly used benzodiazepines are flualprazolam (closely related to Xanax), bromazolam (triazolobenzodiazepine synthesized in 1976 but never marketed), and etizolam (a benzo analogue).19 These are obviously not observed much in practice but are still considered benzodiazepines by their structure and physiological effects.
"Tranq Dope"
“Tranq Dope” is very much like Benzo Dope, but instead of using a benzodiazepine, a tranquilizer is used in the formulation.18 The most common tranquilizer on the streets in this new combination is xylazine, which is a horse tranquilizer. Xylazine is an alpha-2 adrenergic agonist. It decreases the release of norepinephrine and dopamine in the CNS, resulting in depressive physiological effects (e.g., analgesia, sedation, and muscle relaxation). Often, this substance may include heavy doses of caffeine to offset the strength of the tranquilizing effects. Xylazine’s first recognized appearance in the illicit drug market was in 2002, and it is still popular in the U.S., especially on the East Coast.20
Tranq Dope, like all other illicit synthetic opioids, carries a risk for overdose, but this combination poses other significant health risks.18 Xylazine use may cause severe hypoglycemia. It interferes with insulin’s physiological activity, as well as the body’s ability to absorb glucose. In many instances of Tranq Dope use, finger and toe amputations, severe skin ulceration, and reduced oxygen in the fingers, toes, and skin have been seen. This increased risk, on top of the above-average risk for overdose, makes Tranq Dope one of the most dangerous drugs on the black market.
Overdose with this substance is almost always fatal. There are no known reversal agents or rescue drugs to date, and overdoses usually last for days. Overdoses including this horse tranquilizer constitute 30% to 50% of all synthetic opioid overdose deaths, depending on the region.
COUNTERFEIT TABLET DETECTION
The DEA has discovered that an average of six out of every 10 counterfeit prescription pills contain at least 2 mg of fentanyl.21 This is a potentially lethal dose of fentanyl, and these counterfeit pills are made to look like real prescription pills. Examples of an authentic prescription tablet and a counterfeit tablet are found in FIGURE 2. Although it can be nearly impossible to distinguish a counterfeit tablet from an authentic one without laboratory testing, there are some tips that may help22:
- Obtain medications only from licensed pharmacies.
- Look for bubbling or cracks in the tablets. Imperfections can be a sign of counterfeit tablets.
- Observe the packaging. Open or torn packages can be a sign of counterfeit tablets.
NALOXONE AND OPIOID OVERDOSE
 Commonly known by its brand name Narcan, naloxone is a pure-competitive opioid antagonist that displaces opioids at opioid receptor sites.23 Naloxone is used in the setting of an opioid overdose and is devoid of activity when not in the presence of an opioid. This characteristic makes naloxone an excellent drug in an emergency setting, as it poses no harm if there is no overdose present. For this reason, even when etiology is unknown, it is recommended to always give naloxone if symptoms associated with overdose are present. Overdose symptoms that should be recognized for naloxone administration include small pinpoint pupils; loss of consciousness; weak, slow, or absent breathing; choking sounds; limp body; and cold, clammy, possibly discolored skin, especially the lips and fingertips. In the event of a possible opioid overdose, it is important to call emergency personnel immediately by dialing 911. Naloxone should be administered next if available. Attempts should be made to keep patients conscious and breathing if they are awake, and they should be laid on their side to prevent choking if they do lose awareness.
Commonly known by its brand name Narcan, naloxone is a pure-competitive opioid antagonist that displaces opioids at opioid receptor sites.23 Naloxone is used in the setting of an opioid overdose and is devoid of activity when not in the presence of an opioid. This characteristic makes naloxone an excellent drug in an emergency setting, as it poses no harm if there is no overdose present. For this reason, even when etiology is unknown, it is recommended to always give naloxone if symptoms associated with overdose are present. Overdose symptoms that should be recognized for naloxone administration include small pinpoint pupils; loss of consciousness; weak, slow, or absent breathing; choking sounds; limp body; and cold, clammy, possibly discolored skin, especially the lips and fingertips. In the event of a possible opioid overdose, it is important to call emergency personnel immediately by dialing 911. Naloxone should be administered next if available. Attempts should be made to keep patients conscious and breathing if they are awake, and they should be laid on their side to prevent choking if they do lose awareness.
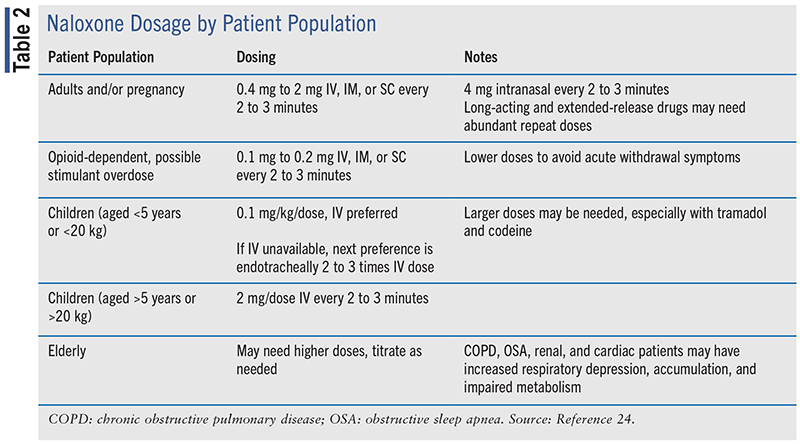
Naloxone is available in several formulations, such as nasal spray and solutions for injection (i.e., prefilled syringe and IM autoinjector).24 It should be administered as soon as possible in the event of a possible opioid overdose, as it has the potential to restore normal breathing within 2 to 3 minutes. The American Heart Association recommends intranasal or IM naloxone with a repeat dose as needed. Nasal naloxone is the most common. It is available in 4-mg and 8-mg doses. One spray in one nostril is the recommended dose for nasal naloxone. If another dose is needed, it may be given every 2 minutes by alternating nostrils. The IM injectable formulation is the second most common dosage form in the emergency setting. The initial dose ranges from 0.4 mg to 2 mg. The injection goes into the thigh and can be administered through clothing. Autoinjectors should be held to the skin 5 seconds after administration to ensure that the complete dose is given. There are many considerations to be made when dosing naloxone, ranging from previous opioid use to age. TABLE 2 includes recommendations for naloxone dosing based on patient population; however, if the specific recommendations are not obtainable in an emergent situation, any naloxone formulation should be used. Once 10 mg is met, other considerations for respiratory depression should be investigated.
 |
Naloxone comes in many different formulations, as mentioned above, but sometimes these formulations can be used off-label in different ways than intended.24 For instance, the IV naloxone formulation can be used intranasally or through inhalation. Continuous infusions are also used in instances of long-acting opioid exposure. When administering injectable naloxone intranasally, the total dose is given divided equally in each nostril by using a mucosal atomization device (MAD). If a MAD is not available, then a significant amount of drug will most likely be lost due to swallowing and first pass metabolism. When administering through inhalation, the typical 2-mg naloxone should be diluted with 3 mL of normal saline and administered via a nebulization mask. Many of these off-label uses are seen by emergency medical technicians in the field and by law enforcement officers.
PHARMACIST PRESCRIBING
All 50 states and the District of Columbia have some form of a naloxone access law.25 The laws vary significantly by state. Thirty-three states have a standing order for naloxone, 14 states and D.C. allow pharmacists to enter into an agreement with providers for naloxone prescribing, and in two states, pharmacists can prescribe and dispense naloxone. A standing order authorizes a specified person without prescribing rights to administer and/or supply specified medications.26 The boundaries for pharmacists are always being pushed and should continuously be pushed. This is a great development for patients prescribed opioids or who are at risk for opioid overdoses. Eighty percent of overdose deaths occur inside a home.23 Naloxone should be within reach for anyone who may need it to combat the rising opioid-related deaths in the U.S., and the current access laws allow for more progressive ways to prevent these deaths and possible injury.
CONCLUSION
Opioids are very effective when it comes to relieving pain, but they can have life-altering consequences if misused or abused. Pharmacists can help prevent misuse, dependence, and overdose by being educated on the faults in the system and as well as on the opioids that are being used outside of the healthcare setting. A pharmacist is the medication expert and an accessible healthcare provider; it is imperative that patients be given appropriate and thorough patient education on these drugs and on rescue therapy in case of an overdose.
The content contained in this article is for informational purposes only. The content is not intended to be a substitute for professional advice. Reliance on any information provided in this article is solely at your own risk.
REFERENCES
- CDC. Opioid basics. May 23, 2022. www.cdc.gov/opioids/basics/index.html. Accessed January 31, 2023.
- Brownstein MJ. A brief history of opiates, opioid peptides, and opioid receptors. Proc Natl Acad Sci USA. 1993;90(12):5391-5393.
- History.com. Heroin, morphine and opiates. June 10, 2019. www.history.com/topics/crime/history-of-heroin-morphine-and-opiates. Accessed January 1, 2023.
- Dowell D, Haegerich TM, Chou R. CDC guideline for prescribing opioids for chronic pain—United States, 2016. MMWR Recomm Rep. 2016;65(1):1-49.
- Agency Medical Directors’ Group. Interagency guideline on prescribing opioids for pain. June 2015. www.agencymeddirectors.wa.gov/files/2015amdgopioidguideline.pdf. Accessed January 1, 2023.
- United Nations. History of heroin. January 1, 1953. www.unodc.org/unodc/en/data-and-analysis/bulletin/bulletin_1953-01-01_2_page004.html. Accessed January 31, 2023.
- Saxe M. The rise and fall (?) of the opioid epidemic. WoodburyCT.org. https://woodburyct.org/vertical/Sites/%7B59751637-3DF2-41D3-B20A-866E470B1D1D%7D/uploads/Opioids_Talk_4.28.17_(002)(1).pptx. Accessed January 31, 2023.
- Department of Health and Human Services. What is the U.S. opioid epidemic? October 27, 2021. www.hhs.gov/opioids/about-the-epidemic/index.html. Accessed January 1, 2023.
- CDC. Understanding the opioid overdose epidemic. June 1, 2022. www.cdc.gov/opioids/basics/epidemic.html. Accessed January 31, 2023.
- Department of Health and Human Services. Overdose prevention strategy. www.hhs.gov/overdose-prevention/. Accessed January 31, 2023.
- Pacific Northwest National Laboratory. Fentanyl analogs: what are fentanyl analogs? https://www.pnnl.gov/explainer-articles/fentanylanalogs. Accessed January 31, 2023.
- CDC. Fentanyl facts. February 23, 2022. www.cdc.gov/stopoverdose/fentanyl/index.html. Accessed November 27, 2022.
- Drug Enforcement Administration. DEA warns of brightly-colored fentanyl used to target young Americans. August 30, 2022. www.dea.gov/press-releases/2022/08/30/dea-warns-brightly-colored-fentanylused-target-young-americans. Accessed January 31, 2023.
- Drug Enforcement Administration. Trafficker-quantities of “Rainbow Fentanyl” arrive in New York. October 4, 2022. https://www.dea.gov/press-releases/2022/10/04/trafficker-quantities-rainbow-fentanyl-arrive-new-york. Accessed January 31, 2023.
- Vandeputte MM, Krotulski AJ, Papsun DM, et al. The rise and fall of isotonitazene and brorphine: two recent stars in the synthetic opioid firmament. J Anal Toxicol. 2022;46(2):115-121.
- Drug Enforcement Administration. New, dangerous synthetic opioid in D.C., emerging in tri-state area. June 1, 2022. www.dea.gov/stories/2022/2022-06/2022-06-01/new-dangerous-synthetic-opioid-dcemerging-tri-state-area. Accessed January 31, 2023.
- Drug Enforcement Administration. Isotonitazene. December 2022. www.deadiversion.usdoj.gov/drug_chem_info/isotonitazene.pdf. Accessed January 31, 2023.
- Asana Recovery. Benzo Dope and Tranq Dope—what are they? June 20, 2022. https://asanarecovery.com/benzo-dope-and-tranq-dopewhat-are-they/. Accessed December 2, 2022.
- Drug Enforcement Administration. Flualprazolam. June 2020. www.deadiversion.usdoj.gov/drug_chem_info/flualp.pdf. Accessed January 31, 2023.
- Drug Enforcement Administration. Xylazine. November 2022. www.deadiversion.usdoj.gov/drug_chem_info/Xylazine.pdf. Accessed January 31, 2023.
- Drug Enforcement Administration. One pill can kill. www.dea.gov/onepill. Accessed January 31, 2023.
- CDC. Counterfeit medicines. https://wwwnc.cdc.gov/travel/page/counterfeit-medicine. Accessed January 31, 2023.
- CDC. Lifesaving naloxone. August 19, 2021. www.cdc.gov/stopoverdose/naloxone/index.html. Accessed January 31, 2023.
- Oclc.org Database. Naloxone. 2022. https://online-lexi-com.wmcarey.idm.oclc.org/lco/action/doc/retrieve/docid/patch_f/7338?cesid=2VFmOgl3iHA&searchUrl=%2Flco%2Faction%2Fsearch%3Fq%3DNaloxone%26t%3Dname%26acs%3Dfalse%26acq%3DNaloxone. Accessed December 2, 2022.
- Legislative Analysis and Public Policy Association. Naloxone: summary of state laws. July 2022. http://legislativeanalysis.org/wpcontent/uploads/2022/09/Naloxone-Access-Summary-of-State-Laws.pdf. Accessed January 31, 2023.
- Kokosky G. Understanding naloxone standing orders is vital. Pharm Times. 2018;84(11).