Treatment and Management of Upper Respiratory Tract Infections
RELEASE DATE:
July 1, 2018
EXPIRATION DATE:
July 31, 2020
FACULTY:
Erin L. Thompson, PharmD, BCPS, BCACP
Assistant Professor of Pharmacy Practice
The University of Findlay College of Pharmacy
Findlay, Ohio
FACULTY DISCLOSURE STATEMENTS:
Dr. Thompson has no actual or potential conflicts of interest in relation to this activity.
Postgraduate Healthcare Education, LLC does not view the existence of relationships as an implication of bias or that the value of the material is decreased. The content of the activity was planned to be balanced, objective, and scientifically rigorous. Occasionally, authors may express opinions that represent their own viewpoint. Conclusions drawn by participants should be derived from objective analysis of scientific data.
ACCREDITATION STATEMENT:
Pharmacy
 Postgraduate Healthcare Education, LLC is accredited by the Accreditation Council for Pharmacy Education as a provider of continuing pharmacy education.
Postgraduate Healthcare Education, LLC is accredited by the Accreditation Council for Pharmacy Education as a provider of continuing pharmacy education.
UAN: 0430-0000-18-031-H01-P
Credits: 2.0 hours (0.20 ceu)
Type of Activity: Knowledge
TARGET AUDIENCE:
This accredited activity is targeted to pharmacists. Estimated time to complete this activity is 120 minutes.
Exam processing and other inquiries to:
CE Customer Service: (800) 825-4696 or cecustomerservice@powerpak.com
DISCLAIMER:
Participants have an implied responsibility to use the newly acquired information to enhance patient outcomes and their own professional development. The information presented in this activity is not meant to serve as a guideline for patient management. Any procedures, medications, or other courses of diagnosis or treatment discussed or suggested in this activity should not be used by clinicians without evaluation of their patients' conditions and possible contraindications or dangers in use, review of any applicable manufacturer's product information, and comparison with recommendations of other authorities.
GOAL:
To provide the pharmacist with an overview of common upper respiratory tract infections (URTIs), common pathogens, and recommended treatments.
OBJECTIVES:
After completing this activity, the participant should be able to:
- Identify the most typical pathogens for common URTIs in adults and differentiate between viral and bacterial causes of these URTIs.
- Recognize signs and symptoms of common URTIs in adults.
- Determine nonpharmacologic and pharmacologic treatments for adults with common URTIs.
- Recommend appropriate measures to prevent the development of URTIs.
ABSTRACT: Upper respiratory tract infections (URTIs), which occur when a pathogen infects the upper respiratory tract, are common ailments in children and adults and are a frequent reason for seeking medical care. Common URTIs include acute pharyngitis, acute sinusitis, acute otitis media, epiglottitis, croup, laryngitis, and the common cold. Pharmacists should be able to recognize the signs and symptoms of these conditions in order to properly refer patients. Also, because these infections are bacterial or viral in origin, it is important for pharmacists to identify when antibiotics are warranted and to practice good antimicrobial stewardship. Pharmacists can also be instrumental in recommending nonpharmacologic and adjunctive therapies, as well as suggesting vaccines that can help reduce the incidence of URTIs.
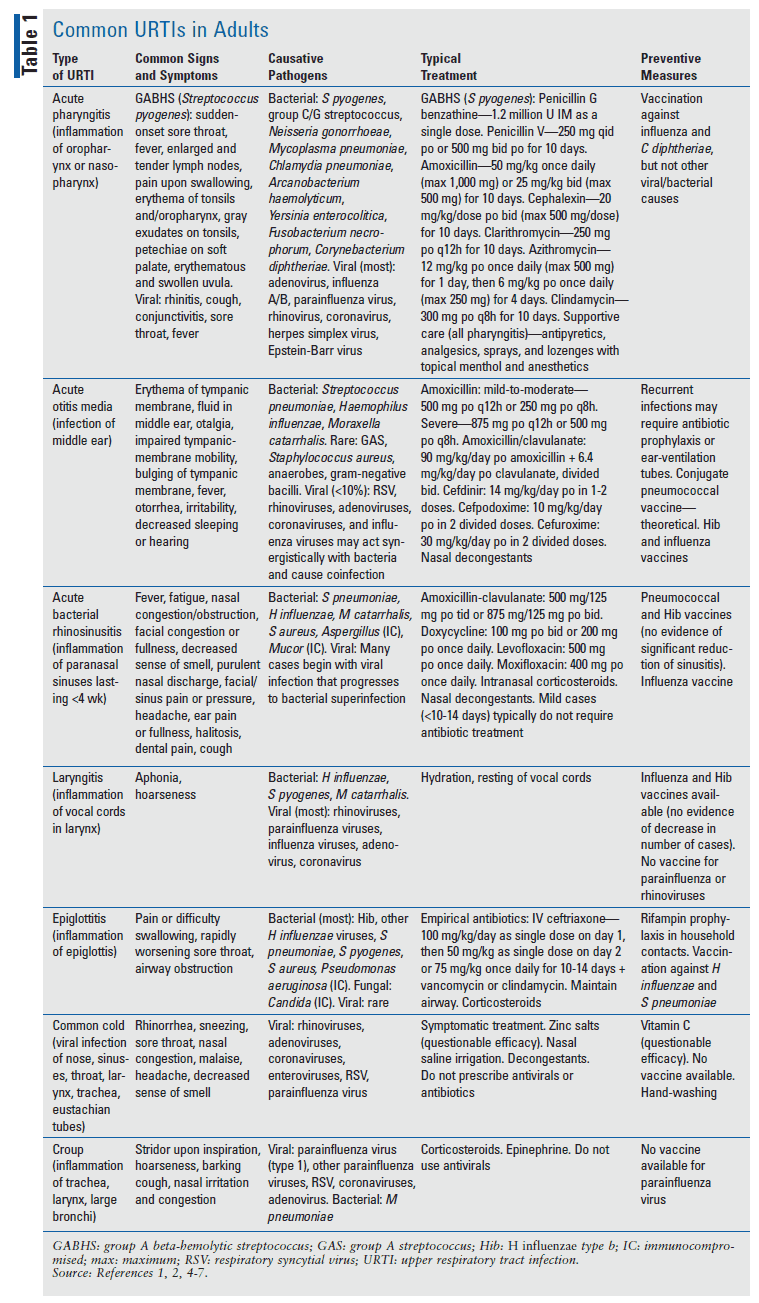
Upper respiratory tract infections (URTIs), which can involve the nose, oral cavity, larynx, and pharynx, are one of the most cited reasons for ambulatory-care office visits each year. Although URTIs are typically self-limiting, they may require pharmacologic therapy, and in certain cases they may necessitate hospitalization and even be life-threatening.1,2 The most common URTIs are otitis media, rhinosinusitis, and pharyngitis; others include tonsillitis, acute rhinitis, laryngitis, epiglottitis, croup, and the common cold.2-4 In most instances, URTIs are caused by viruses, but the most common bacterial pathogens are group A beta-hemolytic streptococcus (GABHS) and Streptococcus pneumoniae.4 TABLE 1 lists definitions, clinical presentations, causative pathogens, typical first-line treatments, and preventive measures for common URTIs in adults.1,2,4-7
Pharyngitis
Pharyngitis is inflammation of the throat that is usually viral in origin; however, some cases are caused by bacteria. In 10% of cases, the pathogen is GABHS (Streptococcus pyogenes).2,4 When GABHS is the cause of pharyngitis, the condition is known as strep throat. If GABHS is not treated efficiently and appropriately, it can lead to rare but severe sequelae, such as rheumatic fever. Additional complications include otitis media, necrotizing fasciitis, glomerulonephritis, reactive arthritis, mastoiditis, rhinosinusitis, cervical lymphadenitis, reactive arthritis, peritonsillar abscess, and retropharyngeal abscess.4 Viral causes of pharyngitis include rhinovirus, coronavirus, Epstein-Barr virus, parainfluenza virus, adenovirus, influenza A and B, Coxsackie virus, and herpes simplex virus. S pyogenes is the most alarming bacterial cause because of its sequelae; other bacterial causes of pharyngitis include Neisseria gonorrhoeae (sign of sexual abuse in children), Group C and G streptococci, Mycoplasma pneumoniae, Arcanobacterium haemolyticum, Corynebacterium diphtheriae, Chlamydia pneumoniae, Yersinia enterocolitica, and Fusobacterium necrophorum.2,4
Pharyngitis accounts for an estimated 12 million physician visits in the United States each year.1 Pharyngitis caused by S pyogenes has the greatest incidence in winter or early spring, and it is transmitted through droplets of salivary or nasal fluid. Therefore, those in close quarters, crowded areas, families, schools, and institutions are likely to transmit the bacteria to one another. There is typically an incubation period of 2 to 5 days before symptoms appear.4 Persons who contract pharyngitis from S pyogenes typically present with sore throat, pain upon swallowing, fever, red and swollen uvula, petechiae on the soft palate, enlarged lymph nodes, and erythema of tonsils with or without gray exudates. If pharyngitis is viral in origin, rhinitis, cough, and conjunctivitis are common, as well as fever and sore throat.
Pharyngitis can be diagnosed with use of a rapid antigen detection test (RADT) or a culture. RADT is highly specific (95%), but it is less sensitive than culture. If a child or adolescent has a negative RADT result, it is recommended to perform a culture. This is not required for adults because the risk of pharyngitis caused by S pyogenes and sequelae such as rheumatic fever is low.1,8
Once a patient is diagnosed with pharyngitis, supportive care with analgesics, antipyretics, and topical sprays and lozenges may be used to reduce symptoms. It must be determined whether a patient requires antibiotics, which are overprescribed for this condition. Approximately 60% to 73% of patients reporting a sore throat receive antibiotics even though only about 10% of pharyngitis cases are bacterial in origin and require antibiotic treatment.2,4 Pharmacists can intervene with antimicrobial stewardship to minimize overprescribing of antibiotics for nonbacterial causes of pharyngitis. If S pyogenes is the cause of pharyngitis, the recommended treatment is a 10-day course of amoxicillin or penicillin in nonallergic patients.8 Patients who are allergic to penicillin but not anaphylactically sensitive may be given a first-generation cephalosporin for 10 days. Alternatives for patients who are allergic to penicillin include 10-day treatment with either clindamycin or clarithromycin and 5-day treatment with azithromycin.8 There is no vaccine for pharyngitis that is caused by S pyogenes; however, vaccination against influenza and C diphtheriae can help decrease pharyngitis arising from those pathogens.2
Otitis Media
Otitis media is inflammation of the middle ear. Otitis media can be acute or chronic, or fluid may be present in the middle ear without signs or symptoms of infection (otitis media with effusion). Acute otitis media (AOM) is the most common bacterial infection in children, but its incidence decreases with age. The incidence in adults is reported to be 0.25%.1 The anatomy of the Eustachian tube is more horizontal and shorter in children, making them more susceptible to AOM.4 AOM typically begins after a viral infection of the upper respiratory tract, which impairs the mucociliary function of the Eustachian tube and middle ear. The ear can then become clogged with fluid, resulting in a painful, bulging, and erythematous tympanic membrane. Because mucociliary function is impaired, bacteria colonize the middle ear, leading to infection.4 Signs and symptoms of AOM include otalgia, pressure and fluid in the ear, tugging or pulling at the ear (especially in children), fever, decreased hearing, irritability, bulging and erythema of the tympanic membrane, limited mobility of the tympanic membrane, otorrhea, and difficulty sleeping. To diagnose AOM, along with acute onset, both of the following must be present: middle-ear effusion and indications that the tympanic membrane is inflamed.1,4,5
Although both viruses and bacteria can cause otitis media, a viral cause alone is uncommon (<10%). However, it is common for a person to have an upper respiratory virus that predisposes them to a bacterial coinfection.1,5 Common viruses implicated in AOM include respiratory syncytial virus (RSV), rhinovirus, adenovirus, influenza, and coronavirus. The common bacterial pathogens are S pneumoniae, Haemophilus influenzae, and Moraxella catarrhalis. Other rare pathogens include GAS, Staphylococcus aureus, anaerobes, and gramnegative bacilli.1,5
When a clinical diagnosis of AOM has been made, treatment is empiric and directed toward the most common bacterial pathogens: S pneumoniae, H influenzae, and M catarrhalis. Some experts argue that if AOM is not severe, these patients can be observed and not treated with antibiotics. However, randomized trials have shown that antibiotic treatment helps resolve signs and symptoms more quickly and decreases complications such as perforation and otorrhea.1 Withholding antibiotics should be considered—at the provider's discretion—only in healthy patients with mild illness who are older than 2 years of age.1 The preferred treatment for AOM is amoxicillin (amoxicillinclavulanate in those with severe disease). If the patient does not have a severe type 1 (anaphylactic) reaction to penicillin, cephalosporins may be used. Cefdinir, cefpodoxime, and cefuroxime are preferred in this case. For patients with a severe penicillin allergy, azithromycin and clarithromycin are also options. In severe cases of AOM, ceftriaxone may be considered in those who have failed therapy with amoxicillin-clavulanate or have a penicillin allergy that is not a type 1 (anaphylactic) reaction. Finally, clindamycin is recommended in patients who have failed prior therapy and also have a type 1 hypersensitivity reaction to penicillin.1
The recommended duration of treatment for AOM is controversial. Most recommendations call for 10 days of treatment; some argue for a treatment length of 5 days, but there are no conclusive data to support this theory. It is never recommended to prescribe a short duration of therapy in children younger than 2 years; however, in children aged 6 years and older with mild-to-moderate AOM, a 5to 7-day course of antibiotics may be considered.4
Other treatments, such as analgesics (acetaminophen, ibuprofen) and ear drops with local anesthetics (lidocaine, benzocaine), may be considered in appropriate patients. Decongestants and antihistamines are not recommended for the treatment of AOM.4 In children who have recurrent infections, the insertion of tympanostomy tubes should be considered to help aerate the middle ear and to prevent hearing and learning disabilities.4 In order to prevent AOM, vaccination against common pathogens may be considered. A Haemophilus influenzae type b (Hib) vaccine is available that can reduce AOM caused by that particular pathogen. The influenza vaccine should also be recommended annually for those without contraindications, as AOM often follows viral infections.4 The pneumococcal vaccine, which provides immunity to S pneumoniae, can theoretically prevent AOM, as it targets a common bacterial pathogen; however, it is less effective for preventing AOM compared with other pneumococcal disease.2 The use of antibiotics as prophylaxis is not generally recommended.4
Acute Rhinosinusitis
Acute bacterial rhinosinusitis (ABRS) is inflammation of the paranasal sinuses that typically begins with a viral URTI that leads to bacterial superinfection. Sinusitis may also be caused by fungi, such as Mucor and Aspergillus, in immunocompromised patients and those with diabetes.2 The most common bacterial pathogens are H influenzae and S pneumoniae (>50%-70% of cases). Less common bacterial causes include M catarrhalis, streptococci, anaerobes, and S aureus (rare).1,2,4 Sinusitis is a common URTI, with an estimated one in seven noninstitutionalized adults receiving a diagnosis in the past year.1 Of those who present with symptoms, only 2% to 10% have bacterial causes that will benefit from antibiotics. Sinusitis is one of the top five reasons why antibiotics are prescribed, and overprescribing has contributed to antibiotic resistance.1
Patients with ABRS may present with the following signs and symptoms: nasal congestion, postnasal drip, purulent nasal discharge, nasal obstruction, ear pain or fullness, cough, fatigue, sinus pressure, sinus pain, facial pain, dental pain, decreased sense of smell, fever, halitosis, and headache.1,2,4 Viral URTI often precedes acute bacterial sinusitis, similar to the development of AOM after a viral infection. When this happens, drainage of the sinuses by the sinus ostia can become obstructed, resulting in trapped mucosal secretions and leading to replication of bacteria and poor functioning of the body's defense mechanisms. Allergic rhinitis can also produce a decreased mucociliary response and cause an accumulation of mucus. 1,4 Maxillary and ethmoid sinuses are commonly infected. The ostium, which drains the maxillary sinus, is located above the maxillary sinus, and drainage must work against gravity.2,4
ABRS diagnosis is based on clinical findings and symptoms. CT and radiography may be used to confirm sinus involvement; however, they cannot differentiate viral from bacterial cause and therefore cannot determine whether antibiotics are needed.1,4 Sinus puncture is the gold standard for ABRS diagnosis, but it is painful and expensive. Therefore, clinicians rely on their clinical judgment for diagnosis, and most err on the side of prescribing an antibiotic.1,4 The Infectious Diseases Society of America (IDSA) has outlined clinical presentations suggestive of ABRS (not viral sinusitis) and recommend that if any of the three following clinical signs and symptoms are present, empiric antibiotics are warranted: 1) persistent signs and symptoms of sinusitis for 10 or more days without improvement; 2) severe symptoms with high fever (102°F [38.9°C] or higher), facial pain, or purulent nasal discharge lasting 3 to 4 days; and 3) worsening signs or symptoms with new-onset fever, headache, or increased nasal discharge after a viral URTI that lasted 5 to 6 days and was initially improving.6
Once it is determined that the patient has ABRS, antibiotics are warranted and treatment can begin with first-line therapy. Per the IDSA Clinical Practice Guidelines for Acute Bacterial Rhinosinusitis in Children in Adults, the first-line treatment is amoxicillin-clavulanate, with a recommended treatment duration of 5 to 7 days in adults and 10 to 14 days in children. In adults with penicillin allergy, doxycycline or a respiratory fluoroquinolone (levofloxacin or moxifloxacin) is recommended as an alternative agent; in children with a type I hypersensitivity reaction to penicillin, levofloxacin is recommended. Combination therapy with a third-generation cephalosporin (cefpodoxime, cefixime) and clindamycin is recommended for children with non–type I penicillin allergy.6
Nasal saline irrigation may be recommended for adjunctive treatment with antibiotics. However, it is not recommended to use antihistamines or topical or oral decongestants.9 These products may be popular with patients, who feel that they help with nasal patency; however, there is little evidence supporting this claim or the suggestion that they speed up recovery.1,6 These products may also dry the nasal mucosa and prevent clearance of mucosal secretions, which is counterproductive.4 Nasal decongestants (oxymetazoline and phenylephrine) also carry a risk of rebound congestion, so their use for nasal patency and patient comfort should be limited to 3 days.4 To help reduce inflammation, intranasal corticosteroids are recommended as adjunctive therapy, especially in patients with allergic rhinitis.9 Finally, mucolytics such as guaifenesin may be used to help thin mucus, assist its clearance, and improve nasal congestion.4 In terms of sinusitis prevention, vaccines are available to prevent two bacterial causes: Hib and the pneumococcal vaccine. There is no evidence that these vaccines significantly reduce sinusitis occurrence.2 The influenza vaccine should be recommended to all patients aged 6 months and older, and it can help prevent a viral infection that may predispose a patient to developing acute sinusitis.
Laryngitis
Acute laryngitis is inflammation of the vocal cords of the larynx. The hallmark symptoms are aphonia and hoarse voice. Also, the throat may be dry, feel sore, and have a tickling sensation. In some cases, patients with laryngitis have a dry cough.2,6 URTIs that are viral in origin usually precede laryngitis.2 Common viral causes include rhinoviruses and parainfluenza viruses (most common), influenza, adenovirus, and coronavirus. Bacteria are less likely to cause laryngitis, but when they do, H influenzae, S pyogenes, and M catarrhalis are likely pathogens.2 Laryngitis may also be caused by straining the vocal cords or overusing one's voice.8 Diagnosis is made clinically, and treatment involves the use of nonpharmacologic measures, such as adequate hydration, resting the voice, avoiding throat-clearing, limiting caffeine and alcohol, and avoiding smoking or exposure to second-hand smoke.2,6 No vaccine is available to prevent the most common viral infections that lead to laryngitis: rhinoviruses and parainfluenza viruses. The influenza and Hib vaccines theoretically could protect patients from acquiring these pathogens, but there is no evidence that they reduce the number of patients who develop laryngitis.2
Epiglottitis
Acute epiglottitis, often called supraglottitis, is inflammation of the epiglottis. Because it can cause airway obstruction, it is a medical emergency and requires urgent care. In persons with compromised airways, a mortality rate of 3% to 7% has been reported worldwide.6 Signs and symptoms of epiglottitis have a rapid onset and include dysphagia, pain upon swallowing, fever, sore throat, muffled voice, drooling, inspiratory stridor, and preference for sitting forward.1,4,6 The diagnosis of epiglottitis is made via fiberoptic nasolaryngoscopy, through which the red (sometimes referred to as cherry red), swollen epiglottis can be observed. Additionally, ultrasound may be used to view the epiglottis longitudinally for the presence of an alphabet P sign (visualization made by hyoid bone shadow and epiglottis). Following the introduction of the Hib vaccine, the incidence of epiglottitis has decreased.6 Epiglottitis is now considered a rare disease, with reports of only 0.02 cases per 100,000 population per year in children. In adults, the reported incidence is approximately 1.9 cases per 100,000 population per year.1 It is difficult to culture the epiglottis, and blood cultures in these patients are often negative. Therefore, treatment is typically directed by pathogens taken from throat cultures. Hib is the most common bacterial pathogen, but epiglottitis is also caused by other bacteria, including other types of H influenzae, S aureus, S pyogenes, and S pneumoniae. Viral etiology for epiglottitis is rare.1,4
Antibiotic treatment includes empiric therapy against the common bacterial pathogens, with careful attention to providing coverage for penicillin-resistant S pneumoniae and community-acquired methicillin-resistant S aureus. If culture and sensitivity are performed, antimicrobial therapy can be adjusted.6 Therefore, a third-generation cephalosporin (ceftriaxone) plus vancomycin or clindamycin is the preferred treatment.1,2 Since epiglottitis is considered a medical emergency, IV antibiotics with greater bioavailability should be used instead of oral antibiotics. Corticosteroids are considered to help decrease inflammation, although this is not clearly supported in the literature; however, they have been noted to reduce ICU length of stay.6 Patients with epiglottitis are monitored in an ICU, with precautions taken to keep the airway open. Children should be intubated; however, adults without a compromised airway may simply be monitored closely.1,2 Preventive vaccines for S pneumoniae and Hib may be recommended, as they are common bacterial pathogens. As history has shown, vaccination targeting Hib has been effective at significantly reducing the number of patients who develop epiglottitis.
Common Cold
The common cold is a self-limiting viral illness of the upper respiratory tract. Despite its mild nature, the common cold is a leading cause of missed work and school. It is estimated that the common cold accounts for 18 million days of work absence and 23 million days of school absence annually.10 Most colds in the U.S. are contracted during the fall through spring seasons.1,2 Adults average two to four colds per year, whereas children average six to eight per year.1 Common colds are spread through droplets that are transmitted through hand-to-hand contact, sneezing, or hand-to-fomite contact. The virus is then passed to the recipient through contact with the mucous membranes. Viruses that commonly cause the common cold include rhinoviruses (most common), influenza, coronaviruses, adenoviruses, enteroviruses, RSV, and parainfluenza. Rarely, bacteria may be cultured from patients with the common cold. The reason for this is unclear, but this circumstance may be a result of a secondary infection, colonization, or the bacterium causing the cold. Bacterial pathogens that have been isolated include C pneumoniae, H influenzae, S pneumoniae, and M pneumoniae.1,2,10
Signs and symptoms of the common cold include rhinorrhea, sneezing, decreased sense of smell, nasal congestion, sore throat, and malaise.2 A cold usually resolves in 12 to 14 days. If symptoms last more than 2 weeks, other conditions should be ruled out.10 Treatment of the common cold should include symptom reduction through the use of decongestants and nasal saline irrigation. Antihistamines, zinc, vitamin C, cough suppressants, and herbal products are not recommended based on a lack of evidence for their efficacy.2,10 There is no vaccine for any of the viruses that cause the common cold, so the best form of prevention is hand-washing and using hand disinfectants to prevent transmission of the virus.
Because the use of vitamin C for preventing and treating the common cold is often discussed, pharmacists should be able to answer patients' questions regarding its efficacy. The literature on the use of vitamin C for this purpose is highly conflicting; some studies support its effectiveness and others do not. Most literature does show that, in high doses, vitamin C can reduce the duration of the common cold by 1 to 1.5 days.11 In terms of prevention, data suggest that in patients exposed to physical stressors, vitamin C (in high doses of 1-2 g daily) can decrease the number of colds they contract. The effect seems to be dose dependent, with 2 g being more effective than 1 g. Doses of this magnitude increase the risk of side effects, so the benefits of a day or two of symptom relief may not outweigh the risks.11 Also, these benefits have not been observed in the general population. Therefore, the use of vitamin C for treating the common cold is not routinely recommended, nor does evidence support the practice of taking vitamin C to prevent the common cold.
Croup
Croup, which is inflammation of the trachea, larynx, and large bronchi, refers to a group of diseases known as croup syndrome. Croup is a mainly viral illness that causes swelling of the subglottic area of the larynx.12 This URTI is primarily seen in children aged younger than 6 years, with most cases occurring from age 3 months to 3 years.1,12 Croup is more common in boys and in the winter, fall, and spring.1 Patients presenting with croup have inspiratory stridor, "seal's bark" cough, fever, and hoarse voice. These symptoms typically follow the onset of other URTI symptoms by 2 days.1,2 Typical viral pathogens that cause croup include parainfluenza type 1 (most common), RSV, adenovirus, coronavirus, and influenza. M pneumoniae is an atypical bacterium that can cause croup.1,2
A diagnosis of croup is made according to clinical findings. Radiograph evidence may show a steeple sign, which indicates constriction by the inflamed trachea and larynx and looks like an inverted V.2 Viral causes of croup may be detected via polymerase chain reaction or rapid viral antigen techniques.1 Croup is treated based on its severity, which is determined by the Westley Croup Score. This score evaluates air entry, cyanosis, stridor, and retractions, and scores are assigned to each category based on severity.1 Children with mild symptoms (score 2 or under) may be treated as outpatients and monitored closely. Patients with a score of 3 or higher (indicative of moderate-to-severe disease) should be treated in a facility capable of managing airway obstruction.1 The treatment for this condition typically involves nebulized epinephrine, corticosteroids, and humidified air. Nebulized dexamethasone and budesonide are preferred; however, oral or IM administration may also be effective.1,2 For children with mild symptoms who will be managed and monitored at home, the pharmacist can make nonpharmacologic treatment recommendations for providing humidified air for the patient to breathe. Hot water may be run in the shower with the bathroom door closed to fill the air with steam, which the child can then breathe in. If the warm, moist air does not improve stridor, cough, or breathing difficulty, the extent of disease may be more severe, and the child should immediately return to the hospital for further evaluation and treatment.13 Antiviral medications are not recommended.2 There are no preventive vaccines that target the most common pathogen, which is parainfluenza virus.2
Conclusion
URTIs are quite common in the U.S. Most are not life-threatening and can be treated with antibiotics, OTC medications, or nonpharmacologic recommendations. Pharmacists, particularly those in community and ambulatory-care settings, must be able to recognize signs and symptoms of common URTIs and refer patients for medical attention, if needed. This is particularly important in life-threatening conditions, such as epiglottitis, and when prescription therapy with antibiotics and airway management may be warranted. Pharmacists should also be prepared with recommendations for OTC and nonpharmacologic therapies based on the patient's presenting signs and symptoms if they determine that the patient is a candidate for self-treatment. Finally, pharmacists can be instrumental in providing patient education for disease prevention, including the use of vaccines that may be administered in their pharmacy.
References
- File TM Jr. Infections of the upper respiratory tract. In: Grippi MA, Elias JA, Fishman JA, et al, eds. Fishman's Pulmonary Diseases and Disorders. 5th ed. New York, NY: McGraw-Hill Education; 2015.
- Upper respiratory tract infections. In: Levinson W, Chin-Hong P, Joyce EA, et al, eds. Review of Medical Microbiology & Immunology: A Guide to Clinical Infectious Diseases. 15th ed. New York, NY: McGraw-Hill Education; 2018.
- NICE Short Clinical Guidelines Technical Team. Respiratory tract infections—antibiotic prescribing. Prescribing of antibiotics for selflimiting respiratory tract infections in adults and children in primary care. London, England: National Institute for Health and Clinical Excellence; 2008.
- Frei C, Frei B. Upper respiratory tract infections. In: DiPiro JT, Talbert RL, Yee GC, et al, eds. Pharmacotherapy: A Pathophysiologic Approach. 9th ed. New York, NY: McGraw-Hill Education; 2014.
- Ramakrishnan K, Sparks RA, Berryhill WE. Diagnosis and treatment of otitis media. Am Fam Physician. 2007;76:1650-1658.
- Guerra AM, Waseem M. Epiglottitis. StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing; 2018.
- Lexicomp Online. Hudson, OH: Lexi-Comp, Inc; 2018. http:// online.lexi.com. Accessed May 22, 2018.
- Shulman ST, Bisno AL, Clegg HW, et al. Clinical practice guideline for the diagnosis and management of group A streptococcal pharyngitis: 2012 update by the Infectious Diseases Society of America. Clin Infect Dis. 2012;55:1279-1282.
- Chow AW, Benninger MS, Brook I, et al. IDSA clinical practice guideline for acute bacterial rhinosinusitis in children and adults. Clin Infect Dis. 2012;54:e72-e112.
- Dabelić A. Respiratory problems. In: South-Paul JE, Matheny SC, Lewis EL, eds. CURRENT Diagnosis & Treatment: Family Medicine. 4th ed. New York, NY: McGraw-Hill Education; 2015.
- Vitamin C. Natural medicines comprehensive database. http:// naturaldatabase.therapeuticresearch.com/home.aspx. Accessed May 1, 2018.
- Rubin MA, Ford LC, Gonzales R. Sore throat, earache, and upper respiratory symptoms. In: Kasper DL, Fauci AS, Hauser SL, et al, eds. Harrison's Principles of Internal Medicine. 19th ed. New York, NY: McGraw-Hill Education; 2015.
- Symptoms related to the ears, nose, and throat. In: Herrier R, Apgar D, Boyce R, Foster S, eds. Patient Assessment in Pharmacy. New York, NY: McGraw-Hill Education; 2015.